INI-CET 2022 — Surgery
12 Previous Year Questions with Answers & Explanations
Identify the given bone marrow biopsy instrument
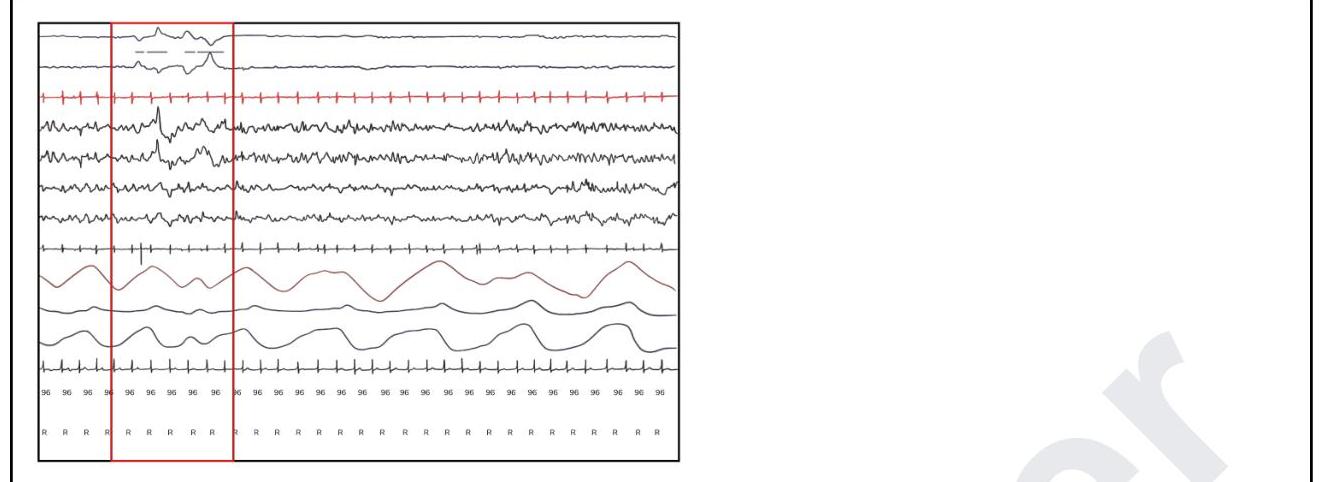
Which of these is the most life-threatening injury that can be identified by assessing the breathing component of the patient?
A 32-year-old female patient with Graves' disease with eye signs and enlarged thyroid planned for a total thyroidectomy. What can be given in the preoperative period to reduce intraoperative bleeding in the patient?
What is the correct sequence of management in a patient who presents to the casualty with an RTA? 1. Cervical spine stabilization 2. Intubation 3. IV cannulation 4. CECT
A patient presents with pneumothorax on chest x-ray. Which of the following is NOT a boundary of the triangle of safety for intercostal chest drain (ICD) insertion?
Which of the following cancers are correctly matched with the criteria for the minimum number of lymph nodes required for pathological staging? A. CA stomach -10 B. CA colon -12 C. CA gall bladder -6 D. CA breast -15
All the following are true about acute cholecystitis, except
Which of the following is not a relative contraindication for breast conservative surgery?
Which of the following is not a perineal approach for the condition shown in the image?
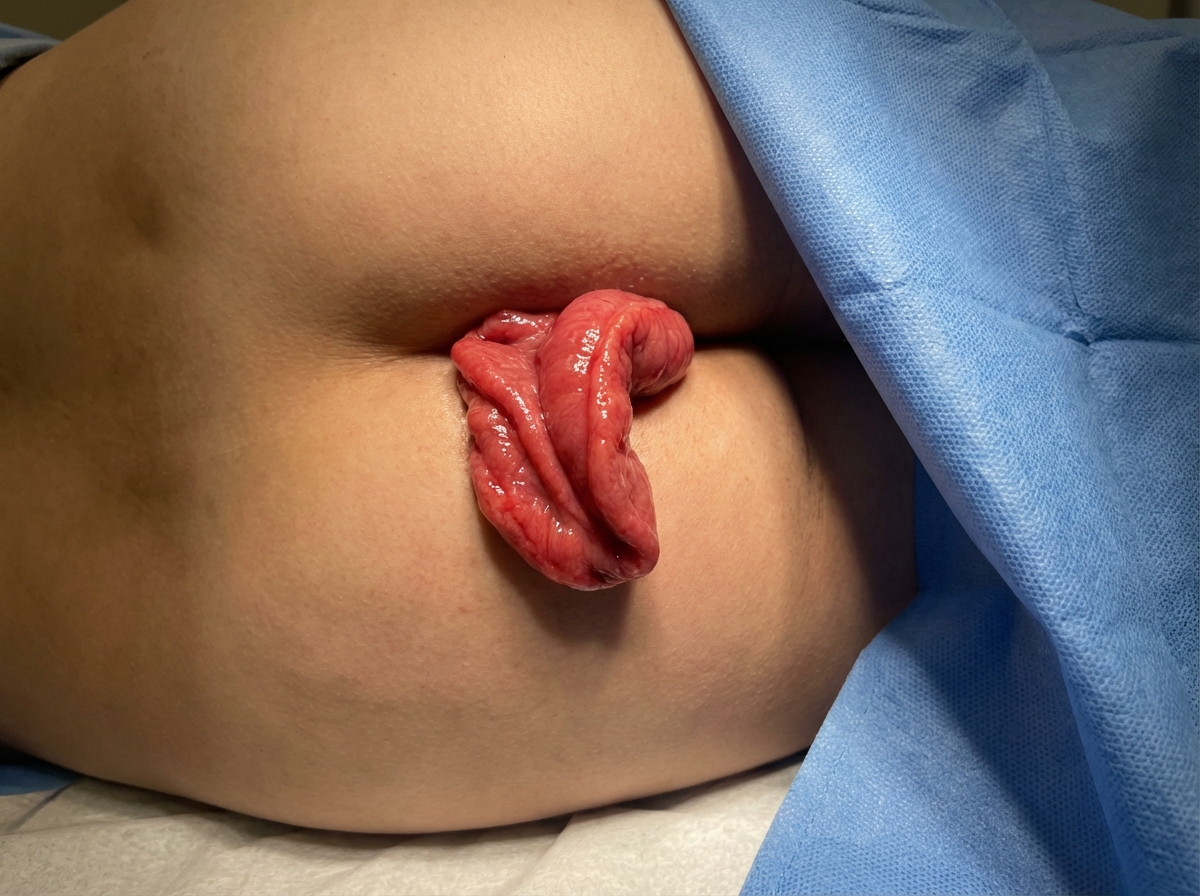
A 50-year-old alcoholic patient presents with a history of waxing and waning jaundice for the past 2 months. His CT examination reveals dilatation of the common bile duct and pancreatic duct. What is the most probable diagnosis in the patient?
INI-CET 2022 - Surgery INI-CET Practice Questions and MCQs
Question 1: Identify the given bone marrow biopsy instrument
- A. Jamshidi needle (Correct Answer)
- B. Salah needle
- C. Tru-cut needle
- D. Vim Silverman needle
Explanation: ***Jamshidi needle*** - The image displays a **Jamshidi needle**, characterized by its **tapered, beveled tip** designed to facilitate entry into the bone and procure an intact core of bone marrow. - This needle is widely considered the **gold standard** for bone marrow biopsy due to its effectiveness in obtaining high-quality trephine samples. *Salah needle* - A Salah needle is primarily used for **bone marrow aspiration**, not typically for a trephine biopsy, and it has a different design meant for aspirating liquid marrow. - It features a **shorter, sturdier design** with a sharp bevel, optimized for safely extracting marrow fluid. *Tru-cut needle* - The Tru-cut needle is primarily designed for obtaining **soft tissue biopsies** (e.g., liver, kidney, prostate) and is not typically used for bone marrow biopsies. - Its mechanism involves an inner cutting stylet and an outer cutting cannula, which is unsuitable for penetrating dense bone and retrieving a bone core. *Vim Silverman needle* - The Vim Silverman needle is also designed for **soft tissue biopsies**, similar to the Tru-cut, and not specifically for bone marrow. - It utilizes a split needle design to capture tissue, which is not appropriate for obtaining a solid bone marrow core.
Question 2: Which of these is the most life-threatening injury that can be identified by assessing the breathing component of the patient?
- A. Blunt cardiac injury
- B. Tension pneumothorax (Correct Answer)
- C. Cervical spine injury
- D. Laryngotracheal injury
Explanation: ***Tension pneumothorax*** - A tension pneumothorax is a **life-threatening condition** identified during the breathing assessment, as it severely impairs ventilation and causes **hemodynamic instability** by compressing major vessels. - Key signs include absent breath sounds on the affected side, **tracheal deviation**, and **hypotension** due to mediastinal shift. *Blunt cardiac injury* - While serious, blunt cardiac injury is typically identified during the **circulation assessment**, with signs like arrhythmias, hypotension, or cardiac tamponade. - Its direct impact on breathing is less immediate compared to a tension pneumothorax. *Cervical spine injury* - A cervical spine injury can affect breathing if it involves the **phrenic nerve** (C3-C5), leading to respiratory paralysis, but this is assessed during the **disability component** or secondary survey for neurological deficits. - It does not directly cause an acute, life-threatening compromise of lung function discernible primarily through a breathing assessment like a tension pneumothorax. *Laryngotracheal injury* - A laryngotracheal injury primarily affects the **airway component** (A in ABCDE), leading to immediate obstruction or stridor. - While critical, it is distinct from problems with the lungs' ability to expand or perform gas exchange, which are assessed under breathing.
Question 3: A 32-year-old female patient with Graves' disease with eye signs and enlarged thyroid planned for a total thyroidectomy. What can be given in the preoperative period to reduce intraoperative bleeding in the patient?
- A. Propylthiouracil
- B. Potassium iodide (Correct Answer)
- C. Betamethasone
- D. Propranolol
Explanation: ***Potassium iodide*** - **Potassium iodide** (e.g., Lugol's solution) is given preoperatively to patients with Graves' disease undergoing thyroidectomy because it **decreases the vascularity** of the thyroid gland, thereby reducing intraoperative bleeding. - It also helps to **block the release of thyroid hormones** from the thyroid gland, stabilizing the patient's thyroid function. *Propylthiouracil* - **Propylthiouracil (PTU)** is an **antithyroid drug** that prevents the synthesis of thyroid hormones by inhibiting the organification of iodine and the coupling of iodotyrosines. - Although it helps to achieve a **euthyroid state** before surgery, it does not directly reduce the vascularity of the thyroid gland to decrease intraoperative bleeding. *Betamethasone* - **Betamethasone** is a corticosteroid used for its **anti-inflammatory** and immunosuppressive effects. - It is not typically used preoperatively in Graves' disease to reduce thyroid vascularity or bleeding; its primary role might be in managing severe **ophthalmopathy** or thyroid storm, not surgical bleeding. *Propranolol* - **Propranolol** is a **beta-blocker** used to control the adrenergic symptoms of hyperthyroidism, such as **tachycardia**, palpitations, and tremors. - While it helps to achieve a more stable cardiac state for surgery, it does not directly impact the **vascularity** of the thyroid gland or reduce surgical bleeding.
Question 4: What is the correct sequence of management in a patient who presents to the casualty with an RTA? 1. Cervical spine stabilization 2. Intubation 3. IV cannulation 4. CECT
- A. 2,1,4,3
- B. 1,3,2,4
- C. 2,1,3,4
- D. 1,2,3,4 (Correct Answer)
Explanation: ***1,2,3,4*** - This sequence follows the **ATLS (Advanced Trauma Life Support)** protocol, prioritizing immediate life threats in order. - **Cervical spine stabilization** is the **first action upon patient contact** to prevent secondary neurological injury in any trauma patient. - **Airway management (intubation)** is then performed **with maintained in-line c-spine stabilization** - these occur nearly simultaneously but c-spine protection is instituted first. - **IV cannulation (circulation)** follows to establish vascular access for resuscitation and medications. - **CECT (imaging)** is performed last, once the patient is stabilized after addressing immediate life threats. - This follows the **ATLS Primary Survey: Airway (with c-spine protection) → Breathing → Circulation → Disability → Exposure**. *2,1,4,3* - This incorrectly places intubation **before** cervical spine stabilization is initiated. - In ATLS, **c-spine protection must be applied immediately upon patient contact** before any airway manipulation. - Delaying IV cannulation until after CECT is inappropriate as circulatory access is critical for early resuscitation. *1,3,2,4* - While this correctly starts with cervical spine stabilization, it incorrectly places **IV cannulation before intubation**. - In the ATLS primary survey, **Airway comes before Circulation** - securing the airway takes priority over establishing IV access. - This sequence could delay critical airway management in a patient with respiratory compromise. *2,1,3,4* - This sequence places **intubation before cervical spine stabilization**, which violates ATLS principles. - **C-spine stabilization must be the first action** upon approaching any trauma patient to prevent secondary spinal cord injury. - While intubation with in-line stabilization is possible, the c-spine protection must be instituted first, not after beginning airway manipulation.
Question 5: A patient presents with pneumothorax on chest x-ray. Which of the following is NOT a boundary of the triangle of safety for intercostal chest drain (ICD) insertion?
- A. Base of axilla
- B. Mid - clavicular line (Correct Answer)
- C. Lateral border of latissimus dorsi
- D. Lateral edge of pectoralis major
Explanation: ***Mid-clavicular line*** - The **mid-clavicular line** is **NOT** a boundary of the triangle of safety; it is a vertical reference line located centrally on the thorax. - The triangle of safety is located in the **mid-axillary region**, not at the mid-clavicular line. - The mid-clavicular line is used for other procedures but is **anterior to the safe zone** for ICD insertion. *Base of axilla* - The **base of the axilla** forms the **superior boundary** of the triangle of safety. - This boundary is typically at the level of the **5th intercostal space** (nipple level in males). - It helps guide ICD insertion away from the **brachial plexus** and axillary vessels. *Lateral border of latissimus dorsi* - The **lateral border of the latissimus dorsi muscle** forms the **posterior boundary** of the triangle of safety. - This landmark ensures the insertion is anterior to major back muscles and avoids injury to the long thoracic nerve. *Lateral edge of pectoralis major* - The **lateral edge of the pectoralis major muscle** forms the **anterior boundary** of the triangle of safety. - This ensures the ICD is inserted lateral to the pectoral muscle, avoiding breast tissue and superficial vessels.
Question 6: Which of the following cancers are correctly matched with the criteria for the minimum number of lymph nodes required for pathological staging? A. CA stomach -10 B. CA colon -12 C. CA gall bladder -6 D. CA breast -15
- A. A,B,C
- B. A,B,C,D
- C. B,C (Correct Answer)
- D. A,C,D
Explanation: ***B,C (Correct Answer)*** - **Colorectal cancer (B)** requires a minimum of **12 lymph nodes** for adequate pathological staging - **correctly matched** ✅ - **Gallbladder cancer (C)** requires at least **6 lymph nodes** for proper staging - **correctly matched** ✅ - These are the only two correctly matched pairs in the question - Adequate lymph node retrieval is essential to prevent **understaging** and ensure accurate prognostic assessment *A,B,C (Incorrect)* - While B and C are correct, **gastric cancer (A)** requires a minimum of **15 lymph nodes**, not 10 - The inclusion of A makes this combination incorrect *A,B,C,D (Incorrect)* - **Gastric cancer (A)** requires **15 lymph nodes**, not 10 - **incorrectly matched** - **Breast cancer (D)** requires a minimum of **10 lymph nodes**, not 15 - **incorrectly matched** - Only B and C are correctly matched *A,C,D (Incorrect)* - **Gastric cancer (A)** requires **15 lymph nodes**, not 10 - **incorrectly matched** - **Breast cancer (D)** requires **10 lymph nodes**, not 15 - **incorrectly matched** - C is correct, but A and D are both incorrectly matched
Question 7: All the following are true about acute cholecystitis, except
- A. Gall bladder thickness >3 mm on USG
- B. Murphy's sign positive
- C. Preferential visualization of gall bladder in HIDA scan (Correct Answer)
- D. Leukocytosis
Explanation: ***Preferential visualization of gall bladder in HIDA scan*** - In acute cholecystitis, the **cystic duct** becomes obstructed, preventing bile flow into the gallbladder. - A **HIDA scan** (hepatobiliary iminodiacetic acid scan) would show **non-visualization of the gallbladder** due to this obstruction, not preferential visualization. *Gall bladder thickness >3 mm on USG* - An **ultrasound (USG)** finding of gallbladder wall thickening **greater than 3 mm** is a common indicator of inflammation in acute cholecystitis. - This thickening is due to **edema** and inflammation of the gallbladder wall. *Murphy's sign positive* - A **positive Murphy's sign** involves tenderness and an inspiratory arrest upon palpation of the right upper quadrant, specifically over the gallbladder. - This clinical sign is a **classic indicator** of acute cholecystitis. *Leukocytosis* - **Leukocytosis**, an elevated white blood cell count, is a common systemic inflammatory response seen in acute cholecystitis. - It reflects the body's reaction to the **inflammation and possible infection** within the gallbladder.
Question 8: Which of the following is not a relative contraindication for breast conservative surgery?
- A. Multicentric disease
- B. Previous radiation to breast
- C. Large tumor size
- D. Small tumor size (<3cm) (Correct Answer)
Explanation: ***Small tumor size (<3cm)*** ✓ - A small tumor size is **NOT a contraindication** for breast-conserving surgery; it is actually a **favorable condition** and an indication for breast conservation. - Small tumors allow for complete tumor removal with good cosmetic outcomes and adequate margins. - This is the **correct answer** as it is the only option that is NOT a relative contraindication. *Multicentric disease* - **Multicentric disease** refers to the presence of multiple tumor foci in **different quadrants** of the breast, making complete surgical removal challenging with breast-conserving surgery. - This is a **relative contraindication** as it increases the risk of **positive margins** and local recurrence, making mastectomy often a more appropriate option. *Previous radiation to breast* - Prior radiation therapy to the breast is a **contraindication** (often considered absolute) for subsequent breast radiation, which is an essential component of breast-conserving therapy. - Re-irradiation carries a high risk of severe **skin and tissue toxicity**, making further breast conservation unfeasible. *Large tumor size* - A large tumor size is a **relative contraindication** as it can make it difficult to achieve **clear surgical margins** while maintaining an acceptable cosmetic result. - However, **neoadjuvant chemotherapy** may downstage large tumors to make them suitable for breast-conserving surgery. - Without tumor reduction, it often requires **mastectomy**.
Question 9: Which of the following is not a perineal approach for the condition shown in the image?
- A. Ripstein's procedure (Correct Answer)
- B. Delorme's procedure
- C. Altemeier's procedure
- D. Thiersch's procedure
Explanation: ***Ripstein's procedure*** - The Ripstein procedure is an **abdominal approach** used for performing a rectopexy to treat rectal prolapse, which is clearly visible in the image. - It involves **fixing the rectum to the sacrum** through an abdominal incision using a synthetic mesh sling. - This is the **only non-perineal approach** among the options listed. *Delorme's procedure* - This is a **perineal approach** for rectal prolapse. - Involves **mucosal stripping** and plication of the rectal muscle wall through the anus. - Suitable for patients unfit for abdominal surgery or with short segment prolapse. *Altemeier's procedure* - This is a **perineal rectosigmoidectomy** (perineal approach). - Involves **resection of the prolapsed rectum and sigmoid colon** through the perineum. - Often combined with levatoroplasty for better results. *Thiersch's procedure* - This is a **perineal encirclement procedure**. - Involves placing a **wire, suture, or synthetic material** around the anus to narrow the anal opening. - Simple perineal approach but has high recurrence rates; rarely used as definitive treatment.
Question 10: A 50-year-old alcoholic patient presents with a history of waxing and waning jaundice for the past 2 months. His CT examination reveals dilatation of the common bile duct and pancreatic duct. What is the most probable diagnosis in the patient?
- A. Common bile duct stone
- B. Head of the pancreas carcinoma
- C. Cholangiocarcinoma
- D. Periampullary carcinoma (Correct Answer)
Explanation: ***Periampullary carcinoma*** - **Waxing and waning jaundice** is the **most characteristic feature** of periampullary tumors, as the tumor may intermittently obstruct and then temporarily release the **ampulla of Vater** (due to tumor friability, inflammation, or necrosis allowing temporary drainage). - The combination of **dilated common bile duct (CBD)** and **pancreatic duct (double duct sign)** indicates obstruction at the level of the ampulla. - The **intermittent nature of jaundice** is the key distinguishing feature that makes periampullary carcinoma more likely than pancreatic head carcinoma in this case. *Head of the pancreas carcinoma* - A **carcinoma of the head of the pancreas** also causes the **double duct sign** and can present with obstructive jaundice. - However, pancreatic head tumors typically cause **progressive, persistent, and painless jaundice** rather than waxing and waning jaundice, as the tumor causes constant external compression of both ducts. - This is a close differential, but the **fluctuating jaundice** favors a periampullary lesion. *Common bile duct stone* - While a **CBD stone** can cause waxing and waning jaundice due to intermittent obstruction (stone moving in and out of ampulla), it is **less likely to cause isolated dilatation of both the pancreatic duct and CBD** (double duct sign). - Stones typically cause **biliary colic, cholangitis, or pancreatitis** rather than isolated double duct dilatation. - The **double duct sign** without inflammatory features points more strongly to malignancy at the ampulla. *Cholangiocarcinoma* - **Cholangiocarcinoma** can cause biliary obstruction and jaundice, but it typically arises within the bile ducts themselves (intrahepatic or hilar). - **Distal cholangiocarcinoma** near the ampulla can mimic periampullary carcinoma, but it is less common for it to cause the degree of **pancreatic duct dilatation** seen in the double duct sign. - Cholangiocarcinoma usually causes **progressive rather than fluctuating jaundice**.