A man was brought to the emergency room after poisoning with an unknown substance. Muscarinic poisoning was suspected and he was treated for the same. What is the possible presenting feature which led to the diagnosis?
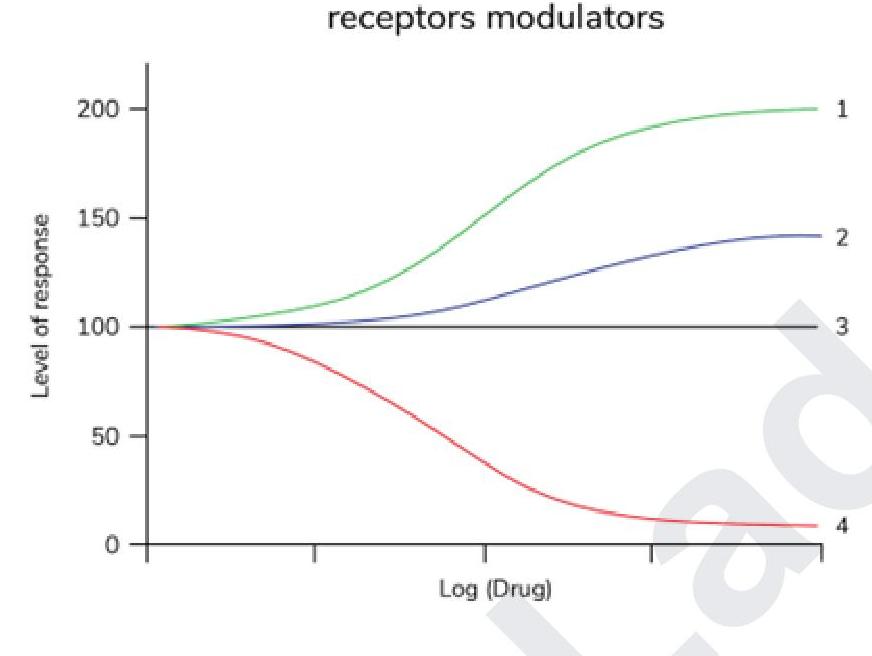
Which of the following statements is correct regarding the given graph?
Match the following antiarrhythmic drugs with their mechanism of action: | Mechanism of action | Drug | | :-- | :-- | | 1. Na+ channel blocker | A. Quinidine | | 2. K+ channel blocker | B. Digoxin | | 3. Na+K+ ATPase inhibitor | C. Esmolol | | 4. Beta-blocker | D. Ibutilide |
Treatment of choice for acute arsenic poisoning is:
Which of these is not a cardiac poison?
A child presents with complaints of fever, rash, body ache, and throat ache. He had a history of thorn prick injury a week back. What antibiotics would you give empirically to this child?
Match the following drugs with the targets of their actions: Drugs: A. Trastuzumab B. Infliximab C. Sirolimus D. Imatinib Targets: 1. BCR-ABL tyrosine kinase 2. mTOR 3. TNF alpha 4. HER2/neu