INI-CET 2022 — Pediatrics
7 Previous Year Questions with Answers & Explanations
A 10-year-old boy presented with fatigue. Investigations revealed: Hemoglobin, 9 g/dL; MCV, 60 fL; MCH, 20 pg; and serum ferritin, 185 µg/L. The TLC was elevated and showed predominant lymphocytes and neutrophils. What is the likely diagnosis in this patient? **Normal values:** - Serum ferritin: 50-150 µg/L
A 10-year-old boy presents with fever, joint pain, and a lesion over his hand, as seen in the image below. Which of the following is the clinical finding, and what is the likely diagnosis?
Adrenocorticotropic hormone is the drug of choice in which of the following conditions?
Which of the following cyanotic heart diseases cause increased pulmonary blood flow? 1. Ebstein anomaly 2. Tetralogy of Fallot 3. Transposition of the great arteries (TGA) 4. Total anomalous pulmonary venous communication (TAPVC) Select the correct combination:
An 11-year-old boy was brought to the outpatient clinic with intention tremor and poor scholastic performance. His sister has similar complaints. On examination, hepatomegaly is seen. The eye finding is shown in the image. What is the probable diagnosis?
An unconscious child is brought to the casualty. What is the correct sequence of the management?
A child presents with poor growth and swelling at joints. A radiograph of his wrist is given below. Lab investigations reveal serum ALP levels of >1500. What is the possible diagnosis?
INI-CET 2022 - Pediatrics INI-CET Practice Questions and MCQs
Question 1: A 10-year-old boy presented with fatigue. Investigations revealed: Hemoglobin, 9 g/dL; MCV, 60 fL; MCH, 20 pg; and serum ferritin, 185 µg/L. The TLC was elevated and showed predominant lymphocytes and neutrophils. What is the likely diagnosis in this patient? **Normal values:** - Serum ferritin: 50-150 µg/L
- A. Anemia of chronic disease
- B. Iron deficiency anemia
- C. Lead poisoning
- D. Beta thalassemia trait (Correct Answer)
Explanation: ***Beta thalassemia trait*** - The combination of **microcytic hypochromic anemia** (low MCV, MCH) with **normal to elevated ferritin** (185 µg/L is above the normal range of 50-150 µg/L) is highly suggestive of **beta thalassemia trait**, as iron stores are typically adequate or increased. - An elevated TLC with predominant lymphocytes and neutrophils is nonspecific but does not rule out thalassemia, as secondary infections or inflammatory processes can occur. *Anemia of chronic disease* - While anemia of chronic disease can cause **microcytic or normocytic anemia** and elevated ferritin (as ferritin is an acute phase reactant), the degree of **microcytosis** (MCV 60 fL) is more profound than typically seen in ACD. - ACD usually involves **inflammation or infection**, but the lab values provided more strongly point away from pure ACD. *Iron deficiency anemia* - **Iron deficiency anemia** is characterized by **microcytic hypochromic anemia** but would present with **low serum ferritin** levels, indicating depleted iron stores. - The patient's **elevated ferritin** (185 µg/L) rules out iron deficiency as the primary cause. *Lead poisoning* - **Lead poisoning** can cause **microcytic anemia** by interfering with heme synthesis, but it is typically associated with a **basophilic stippling** on peripheral blood smear and elevated blood lead levels. - It does not typically present with **elevated ferritin** as a classic feature, and the overall clinical picture is more consistent with a genetic hemoglobinopathy.
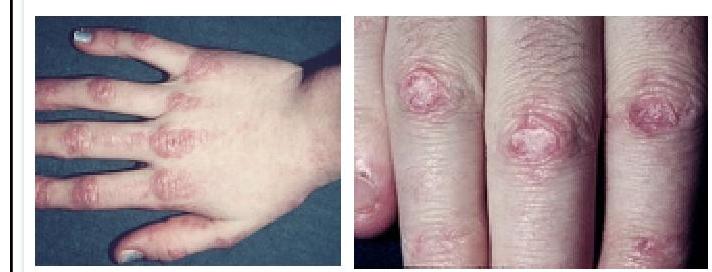
Question 2: A 10-year-old boy presents with fever, joint pain, and a lesion over his hand, as seen in the image below. Which of the following is the clinical finding, and what is the likely diagnosis?
- A. Malar rash - Systemic lupus erythematosus
- B. Heliotrope rash - Dermatomyositis
- C. Erythema multiforme - Stevens-Johnson syndrome
- D. Gottron's papules - Juvenile dermatomyositis (Correct Answer)
Explanation: ***Gottron's papules - Juvenile dermatomyositis*** - The image clearly displays **Gottron's papules**, which are **erythematous, scaling papules** symmetrically distributed over the **dorsal aspects of the interphalangeal joints** (MCP and PIP joints). - The clinical presentation of a 10-year-old boy with **fever, joint pain**, and these characteristic skin lesions is highly indicative of **juvenile dermatomyositis (JDM)**, an inflammatory myopathy. *Malar rash - Systemic lupus erythematosus* - A **malar rash** is a common finding in **systemic lupus erythematosus (SLE)**, but it typically presents as an **erythematous rash over the cheeks and bridge of the nose**, sparing the nasolabial folds, and does not exhibit the papular, scaly appearance over the knuckles seen in the image. - While SLE can cause fever and joint pain, the specific skin lesion depicted is not consistent with a malar rash. *Heliotrope rash - Dermatomyositis* - A **heliotrope rash** is another classic skin manifestation of **dermatomyositis**, characterized by a **purplish discoloration around the eyelids**, often accompanied by periorbital edema. - This is distinct from the lesions shown on the knuckles, which are diagnostic of Gottron's papules, not a heliotrope rash. *Erythema multiforme - Stevens-Johnson syndrome* - **Erythema multiforme** is characterized by **targetoid lesions** with concentric rings, often appearing acutely in response to infections or medications. - **Stevens-Johnson syndrome (SJS)** is a severe form of erythema multiforme, involving extensive epidermal detachment and mucosal involvement, which does not match the chronic-appearing, papular lesions on the knuckles in the image.
Question 3: Adrenocorticotropic hormone is the drug of choice in which of the following conditions?
- A. West syndrome (Correct Answer)
- B. Juvenile myoclonic epilepsy
- C. Rolandic epilepsy
- D. Lennox Gastaut syndrome
Explanation: ***West syndrome*** - **Adrenocorticotropic hormone (ACTH)** is considered the drug of choice for West syndrome, also known as infantile spasms, due to its efficacy in reducing spasm frequency and improving neurodevelopmental outcomes. - **Steroid therapy**, including ACTH, is thought to work by modulating cortisol levels and neurotransmitter activity, suppressing the abnormal brain activity characteristic of these seizures. *Juvenile myoclonic epilepsy* - The drug of choice for juvenile myoclonic epilepsy is typically **valproate**, or newer antiepileptic drugs like levetiracetam or lamotrigine, known for their efficacy against myoclonic seizures. - ACTH is not used in this condition, as it is generally effective for specific types of **epileptic encephalopathies** and not generalized idiopathic epilepsies like JME. *Rolandic epilepsy* - **Rolandic epilepsy** (benign epilepsy with centrotemporal spikes) often resolves spontaneously and may not require treatment, but if seizures are frequent, drugs like gabapentin or carbamazepine are used. - ACTH has no established role in the treatment of Rolandic epilepsy, which is a **focal idiopathic epilepsy** with a good prognosis. *Lennox Gastaut syndrome* - While a severe epileptic encephalopathy, the initial management for **Lennox-Gastaut syndrome** (LGS) typically involves a combination of antiepileptic drugs such as valproate, lamotrigine, clobazam, or rufinamide. - ACTH may be considered as an adjunctive treatment in refractory cases of LGS, but it is not the **first-line drug of choice**, unlike in West syndrome where it holds a primary role.
Question 4: Which of the following cyanotic heart diseases cause increased pulmonary blood flow? 1. Ebstein anomaly 2. Tetralogy of Fallot 3. Transposition of the great arteries (TGA) 4. Total anomalous pulmonary venous communication (TAPVC) Select the correct combination:
- A. 3,4 (Correct Answer)
- B. 1,2
- C. 2,4
- D. 1,4
Explanation: ***3,4 (TGA and TAPVC)*** - **Transposition of the great arteries (TGA)** involves two parallel circulations with the aorta arising from the right ventricle and pulmonary artery from the left ventricle. Mixing occurs through defects (ASD, VSD, or PDA), leading to **pulmonary overcirculation** as oxygenated blood recirculates through the lungs. - **Total anomalous pulmonary venous connection (TAPVC)** results in all pulmonary veins draining into the systemic venous circulation (typically right atrium). This causes **increased volume load on the right heart** and subsequently increased pulmonary blood flow, with obligatory mixing at the atrial level. *1,2 (Ebstein and ToF)* - Both conditions cause **decreased pulmonary blood flow**. - **Ebstein anomaly** involves apical displacement of the tricuspid valve with "atrialization" of the right ventricle, causing tricuspid regurgitation and right-to-left shunting through an ASD/PFO. - **Tetralogy of Fallot** features right ventricular outflow tract obstruction (pulmonary stenosis) as its defining feature, causing reduced pulmonary blood flow. *2,4* - Incorrect combination: **Tetralogy of Fallot causes decreased pulmonary blood flow** due to RVOT obstruction, not increased. *1,4* - Incorrect combination: **Ebstein anomaly causes decreased pulmonary blood flow**, not increased.
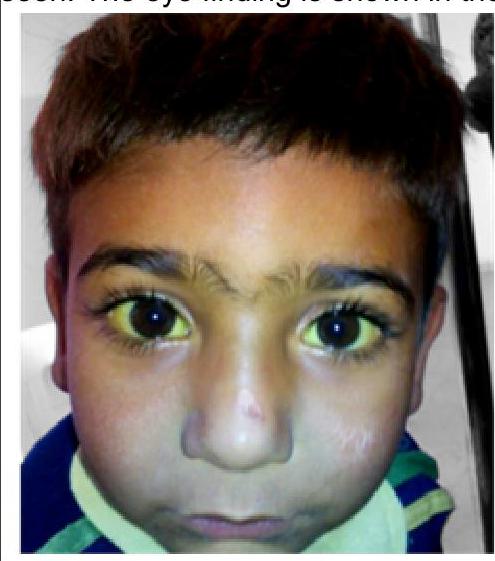
Question 5: An 11-year-old boy was brought to the outpatient clinic with intention tremor and poor scholastic performance. His sister has similar complaints. On examination, hepatomegaly is seen. The eye finding is shown in the image. What is the probable diagnosis?
- A. Glutaric aciduria
- B. Wilson's disease (Correct Answer)
- C. Hepatitis A
- D. Huntington's chorea
Explanation: ***Wilson's disease*** - The combination of **intention tremor**, **poor scholastic performance** (indicating neurological involvement), **hepatomegaly**, and the **eye finding** (Kayser-Fleischer ring seen in the image) points strongly to Wilson's disease. The sister having similar complaints suggests an **autosomal recessive** inheritance pattern, consistent with Wilson's disease. - The image shows **Kayser-Fleischer ring**, a golden-brown ring at the corneal limbus due to **copper deposition in Descemet's membrane**, which is pathognomonic for Wilson's disease with neurological involvement. - Wilson's disease is caused by mutations in the **ATP7B gene**, leading to impaired copper excretion and accumulation in the liver, brain, and cornea. *Glutaric aciduria* - This is a rare **autosomal recessive metabolic disorder** that primarily affects the brain, leading to **dystonia** and **developmental delay**. - While it can cause neurological symptoms, it typically does not present with **hepatomegaly** or **Kayser-Fleischer rings** as prominent features. *Hepatitis A* - **Hepatitis A** is an acute viral infection of the liver, causing symptoms like fever, fatigue, nausea, vomiting, and **jaundice**. - However, it typically does not cause **intention tremor**, **poor scholastic performance**, or have a familial pattern suggesting an inherited neurological disorder. It also does not cause Kayser-Fleischer rings. *Huntington's chorea* - **Huntington's chorea** is an **autosomal dominant neurodegenerative disorder** characterized by **chorea**, psychiatric symptoms, and cognitive decline, typically manifesting in adulthood. - It does not present with **hepatomegaly** or **Kayser-Fleischer rings** at this age and is not associated with the constellation of liver and neurological symptoms described.
Question 6: An unconscious child is brought to the casualty. What is the correct sequence of the management?
- A. Circulation, Airway, Breathing
- B. Breathing, Circulation, Airway
- C. Circulation, Breathing, Airway
- D. Airway, Breathing, Circulation (Correct Answer)
Explanation: ***Airway, Breathing, Circulation*** - The **ABC sequence** is the cornerstone of pediatric resuscitation as per **PALS (Pediatric Advanced Life Support) guidelines** - In an unconscious child, a patent **airway** is the absolute first priority - without this, no oxygen can reach the lungs regardless of breathing effort - Once airway patency is ensured, **breathing** must be assessed and supported to provide adequate ventilation and oxygenation - Only after securing airway and breathing should **circulation** be addressed, as effective circulation without oxygenation is futile - This sequence prevents **hypoxic brain injury**, which can occur within 4-6 minutes of oxygen deprivation *Circulation, Airway, Breathing* - This violates the fundamental **ABC principle** of emergency management - Prioritizing **circulation** before establishing a patent **airway** means attempting to circulate deoxygenated blood - Without airway patency, any circulatory support will fail to deliver oxygen to vital organs, leading to **irreversible hypoxic damage** - In pediatric emergencies, respiratory failure is more common than primary cardiac arrest, making airway management even more critical *Breathing, Circulation, Airway* - Attempting to support **breathing** before securing the **airway** is physiologically ineffective - An obstructed airway prevents air entry despite breathing efforts or bag-mask ventilation attempts - This sequence can lead to **gastric distension, aspiration**, and worsening hypoxia - Delays in airway management increase the risk of **cardiac arrest** from prolonged hypoxemia *Circulation, Breathing, Airway* - This sequence dangerously delays **airway management**, the most time-critical intervention - In an unconscious child, airway obstruction from tongue falling back or secretions is common and immediately life-threatening - Without a patent airway, neither breathing support nor circulatory measures can prevent **brain death** from anoxia - Following this sequence contradicts all **international resuscitation guidelines** (PALS, AHA, ERC)
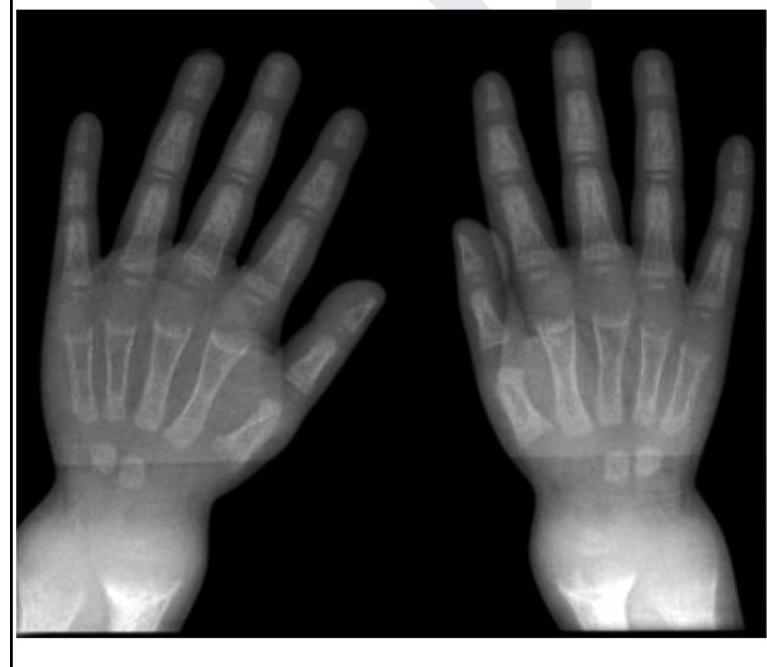
Question 7: A child presents with poor growth and swelling at joints. A radiograph of his wrist is given below. Lab investigations reveal serum ALP levels of >1500. What is the possible diagnosis?
- A. Rickets (Correct Answer)
- B. Osteoporosis
- C. Osteomalacia
- D. Osteogenesis imperfecta
Explanation: ***Rickets*** - The combination of **poor growth**, **joint swelling**, and **elevated alkaline phosphatase (ALP)** in a child strongly indicates rickets, a condition of defective bone mineralization in growing bones. - The radiograph of the wrist would likely show typical findings like **widened growth plates**, **fraying** and **cupping of metaphyses**, and **decreased bone density**, which are characteristic of rickets. *Osteoporosis* - This condition is characterized by **reduced bone mass** and **fragile bones**, typically seen in older adults or due to secondary causes, and is not primarily linked to joint swelling in children. - While ALP levels can be normal or slightly elevated in osteoporosis, a level of >1500 is highly suggestive of active bone formation or breakdown, not typically seen in osteoporosis. *Osteomalacia* - This is defective bone mineralization in adults after growth plates have fused, leading to **bone softening** and **pain**, typically not presenting with joint swelling as a primary symptom. - While it also involves high ALP and bone demineralization, the clinical context of a *child* with growth issues points more specifically to rickets. *Osteogenesis imperfecta* - This is a group of **genetic disorders** characterized by **brittle bones** that fracture easily, often accompanied by **blue sclerae** and **hearing loss**, which are not mentioned in the presentation. - While bone fragility is present, it does not typically cause the described joint swelling or the significantly elevated ALP levels seen in this case.