What is the most common site of abdominal tuberculosis?
A woman presents with altered sensorium, breathlessness, hypotension and bradycardia. Examination revealed non-pitting edema of the extremities. She has a long -standing history of weight gain, constipation, cold intolerance, and menorrhagia. What is the most likely diagnosis?
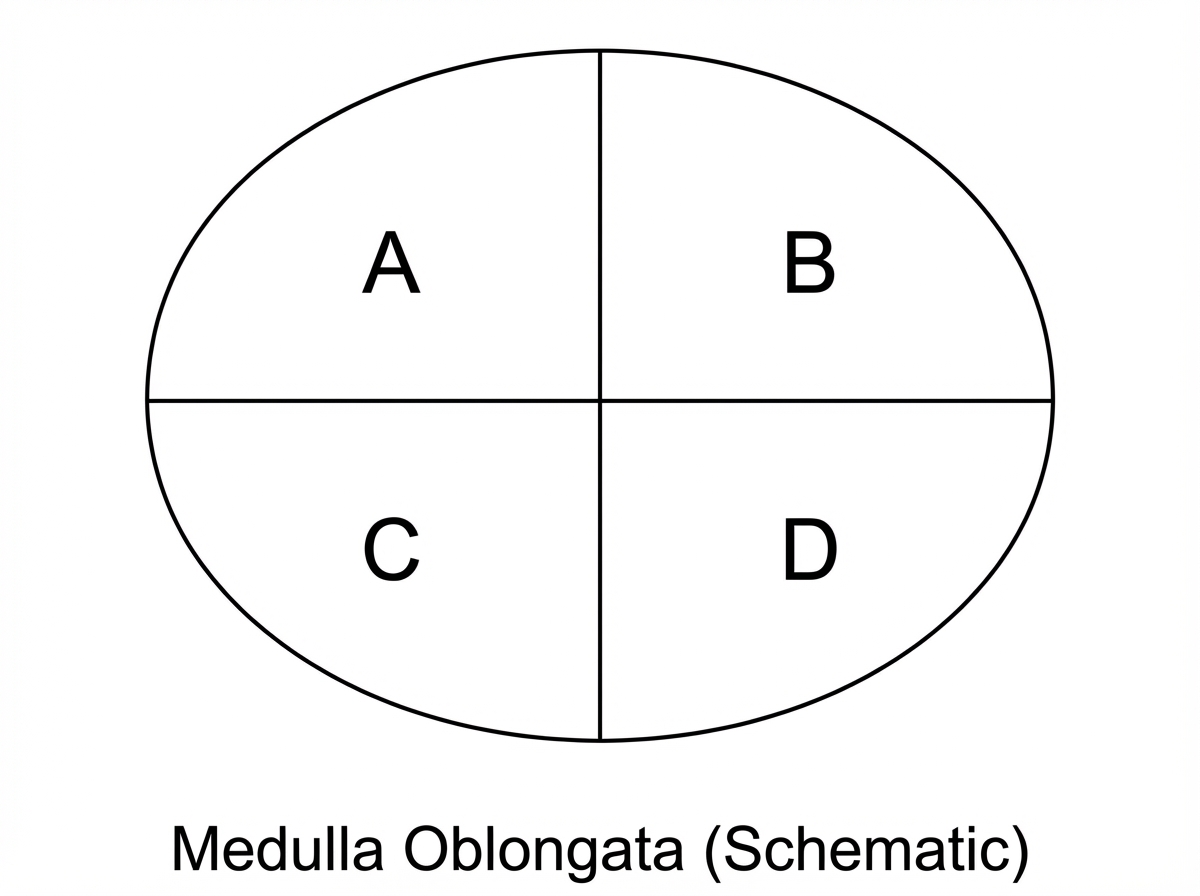
A patient presented with ipsilateral Horner's syndrome, ipsilateral loss of pain and temperature sensations in the face, vertigo with numbness and loss of sweating and dysarthria on the contralateral side. All these symptoms are caused due to a lesion in: