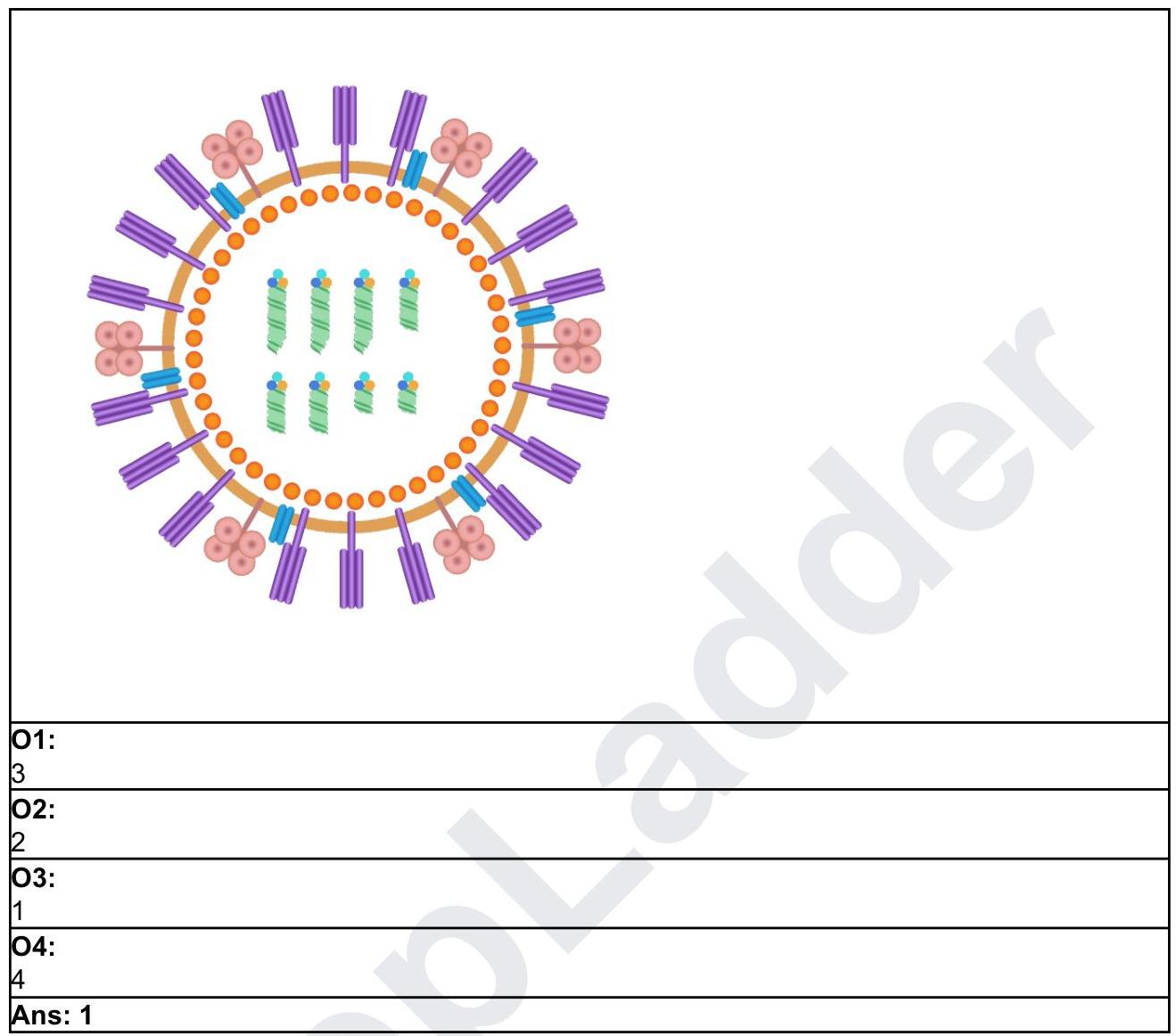
A young man presents with skin lesions as shown in the image below. All of the following organisms can spread through dermal and subcutaneous lymphatics, except
Which virus can be identified by a PCR method and is endemic to India?
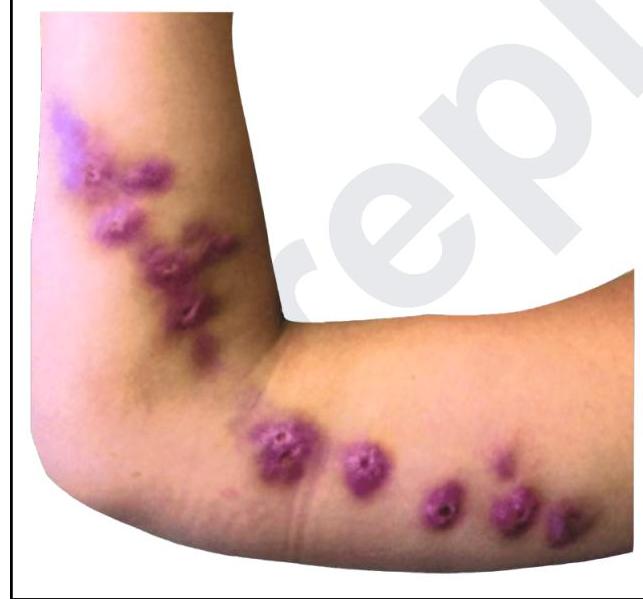
Which of the following is a gram-positive organism that shows the following appearance on Ziehl-Neelsen staining?
The following are parvovirus - related disease - population pairs. Identify the incorrect pair. 1. Aplastic anemia - Patient with hereditary hemolytic anemia 2. Non - immune hydrops - pregnant women 3. Erythema infectiosum - infants 4. Non - erosive arthritis - Patients of SLE
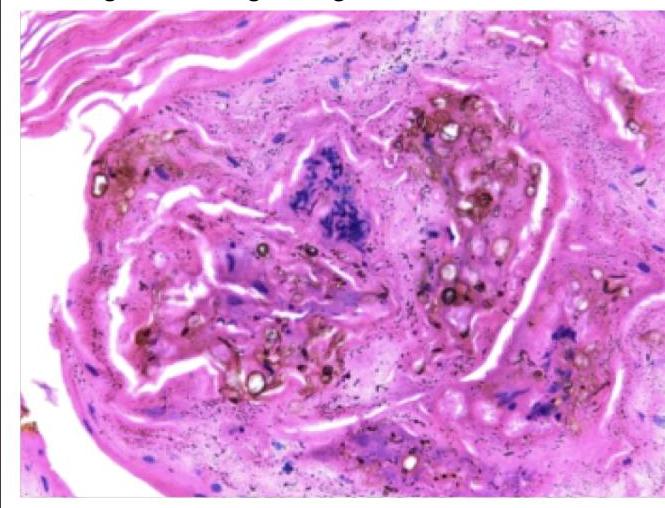
A forest worker developed skin lesions over the forearm, which initially started as macules but then became nodules. Histology of the nodule shows the following findings. Which of the following is true regarding this condition?
The viruses of the Filoviridae family like Ebola and Marburg resemble which of the following morphologies?