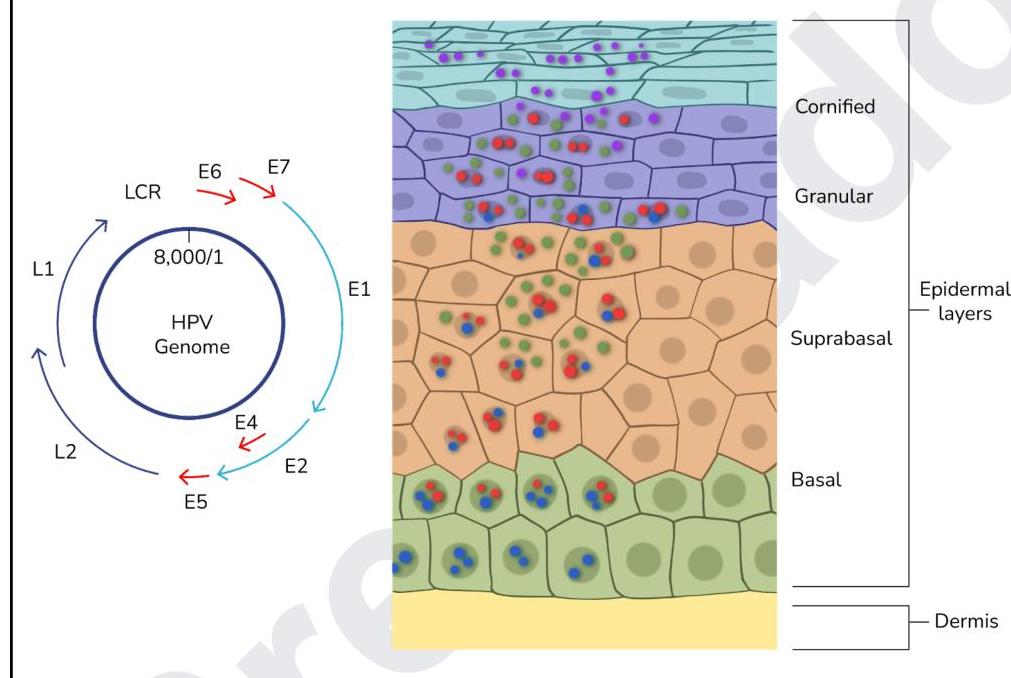
Which of the following statements regarding the given image is correct?
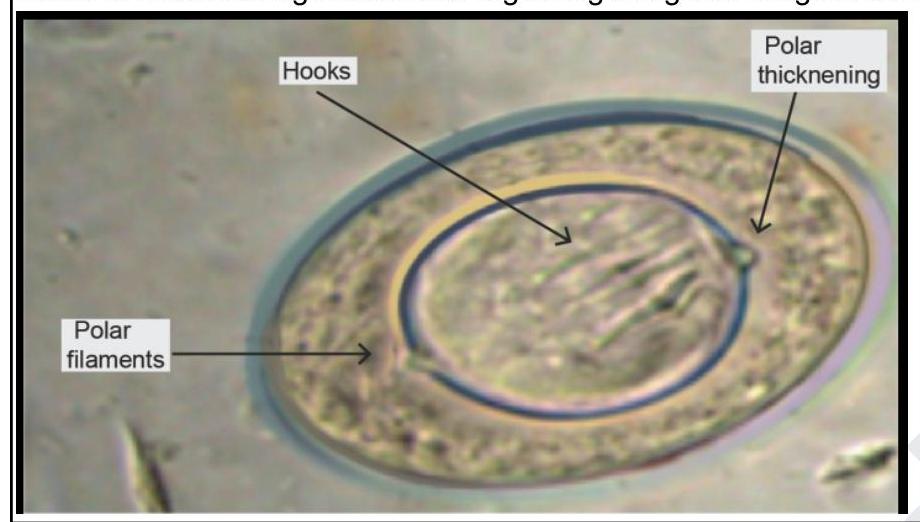
Which of the following are acid-fast staining organisms? 1. Nocardia 2. Mycobacterium leprae 3. Actinomyces 4. Cryptosporidium parvum 5. Isospora belli
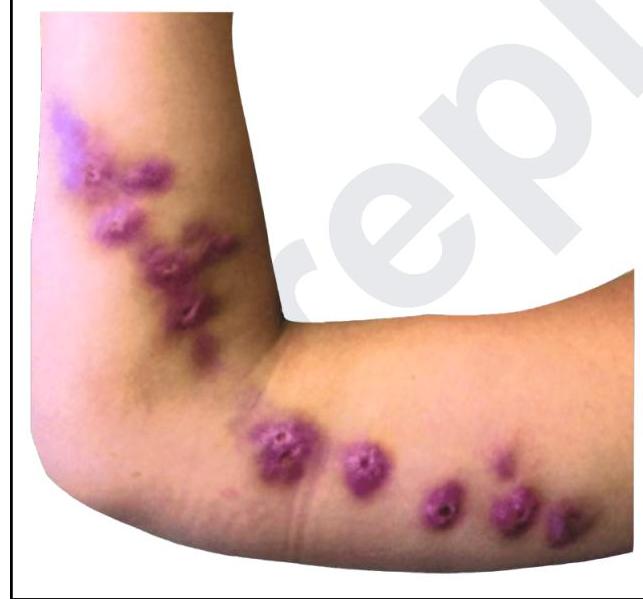
A young man presents with skin lesions as shown in the image below. All of the following organisms can spread through dermal and subcutaneous lymphatics, except