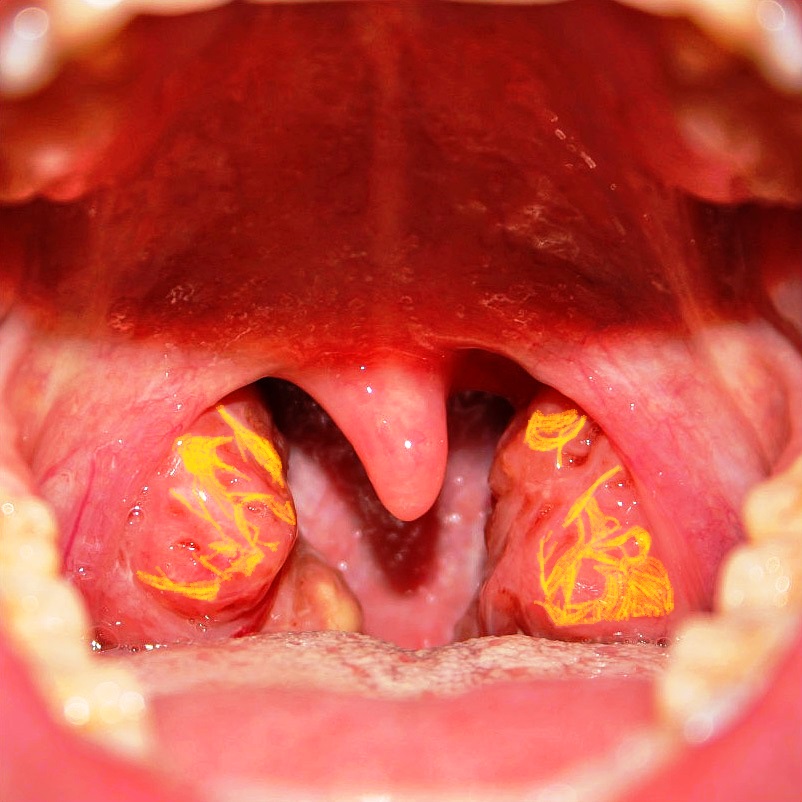
A patient presented with reduced levels of high-density lipoprotein, and ABCA1 mutation. On examination, tonsils appeared as shown in the image. What is the diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Arrange the following in the sequence of auditory pathway: 1. Cochlear nucleus 2. Spiral ganglion 3. Superior olivary nucleus 4. Inferior colliculus 5. Medial geniculate body
Deamination of methylated cytosine forms which of the following?
Increased H+ ions in the intermembrane space of mitochondria are due to?
A 35-year-old female patient presents with complaints of nasal obstruction and post-nasal drip. There is a past history of FESS for failed conservative management 5 years ago. Uncinectomy and maxillary ostium dilation was done during the previous FESS. A DNE done now shows patent ostia and mucosal edema of the maxillary sinus lining. What is the next best step in management? FESS - Functional endoscopic sinus surgery
A patient presented with reduced levels of high-density lipoprotein, and ABCA1 mutation. On examination, tonsils appeared as shown in the image. What is the diagnosis?

Antigen presented on MHC class I molecules activates which of the following cells?
Which of the following is true about anti-CMV IgG antibodies?
A baby is being evaluated for delayed developmental milestones. On examination, the child has hepatosplenomegaly. A microscopic image of the bone marrow evaluation is shown below. What is the most appropriate treatment?

Which of the following structures is pathognomonic for chromoblastomycosis?
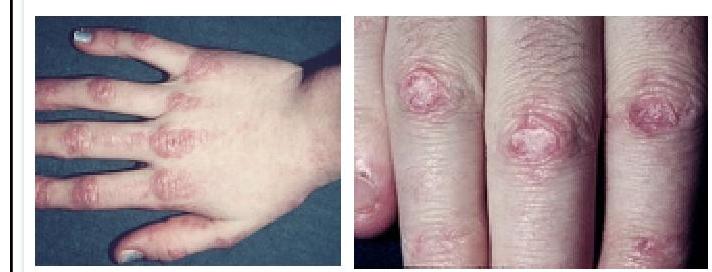
A 10-year-old boy presents with fever, joint pain, and a lesion over his hand, as seen in the image below. Which of the following is the clinical finding, and what is the likely diagnosis?