What is the volume of the prostate in normal adult males?
Which ligament connects medial cuneiform to the base of the 2nd metatarsal?
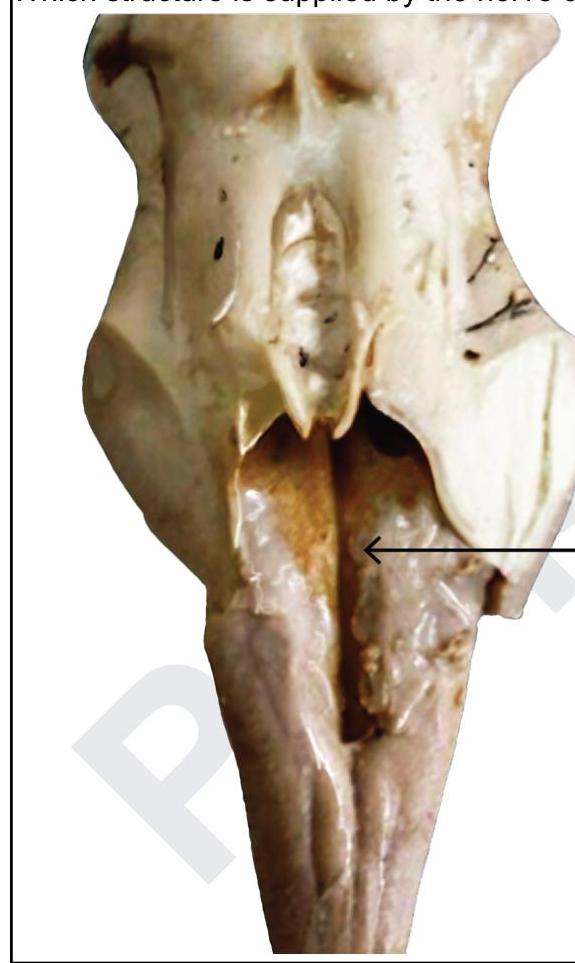
Which structure is supplied by the nerve causing this elevation?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
What is the volume of the prostate in normal adult males?
Which ligament connects medial cuneiform to the base of the 2nd metatarsal?
Which structure is supplied by the nerve causing this elevation?

Cyclooxygenase plays a role in which pathway?
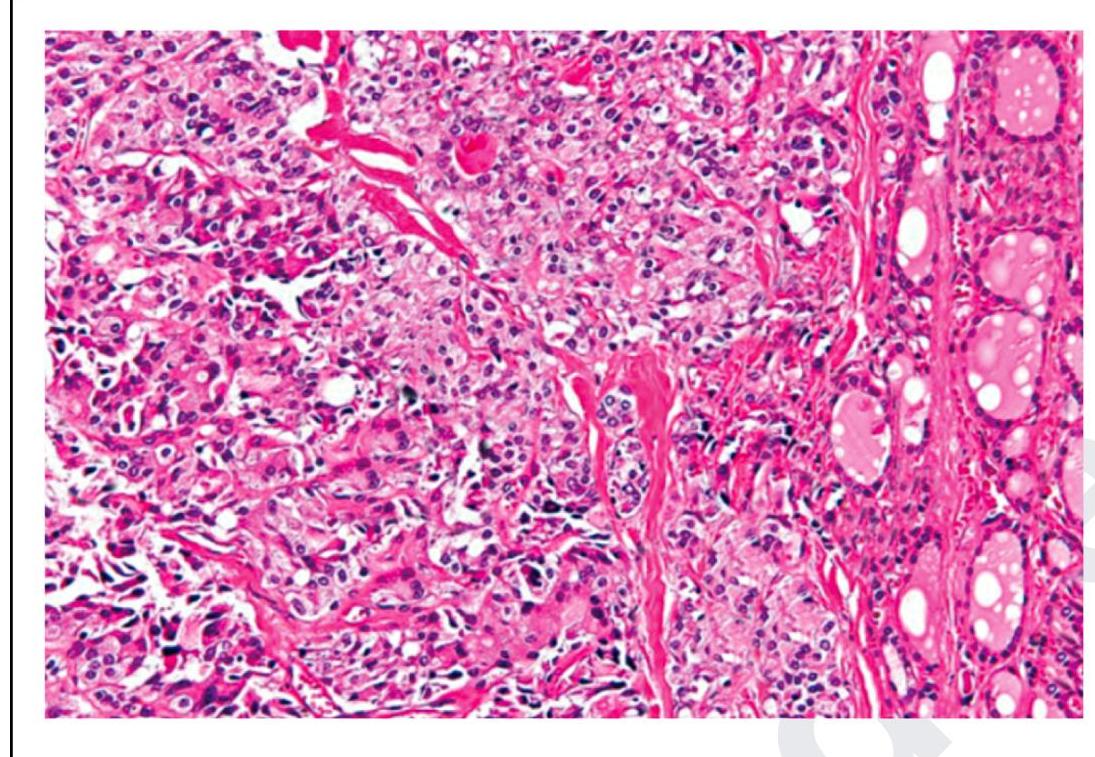
The following is a histopathological image of thyroid pathology. What is the diagnosis?
A 10-year-old boy presented with fatigue. Investigations revealed: Hemoglobin, 9 g/dL; MCV, 60 fL; MCH, 20 pg; and serum ferritin, 185 µg/L. The TLC was elevated and showed predominant lymphocytes and neutrophils. What is the likely diagnosis in this patient? **Normal values:** - Serum ferritin: 50-150 µg/L
A patient who is on treatment for hyperlipidemia develops gallstones. What is the mechanism of action of the causative drug that was given to this patient?
Choose the correct options regarding the route of administration and bioavailability. A- Intravenous =1 B- 0.75< Oral <1 C-0.75 <IM ≤ 1 D- 0.75<SC ≤ 1 IM - Intramuscular SC- Subcutaneous
Which of the following is the most effective oral drug for smoking cessation?
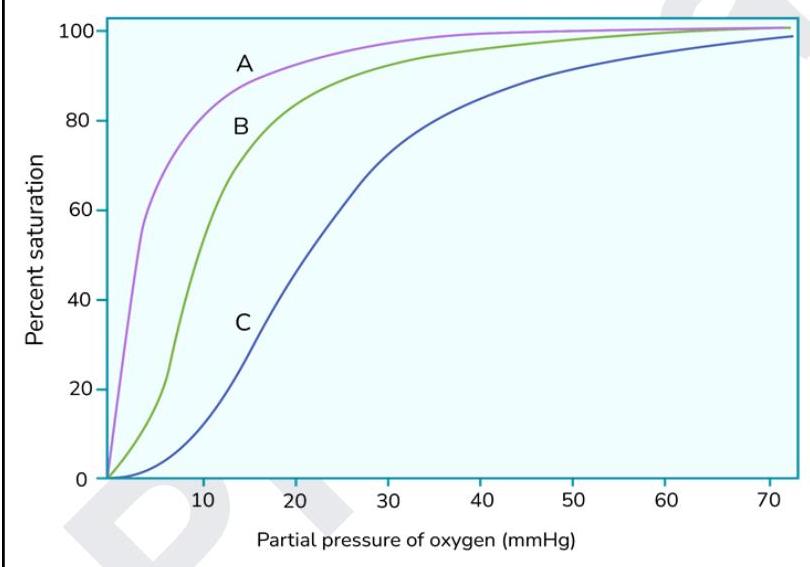
The graph below shows oxygen dissociation curves. What does the curve marked as 'A' indicate?