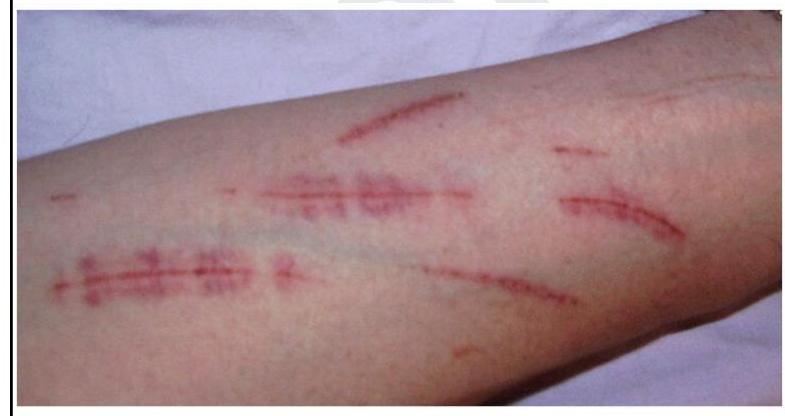
Post-mortem examination of a patient reveals the following. What is this finding known as?
Treatment of choice for acute arsenic poisoning is:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Fingerprint first develops in how many weeks of intrauterine life?
A 7-year-old child presents to the dermatology clinic with multiple small, painless, flesh-colored papules on the trunk and arms that have been present for 3 months. The lesions are 2-4 mm in diameter, dome-shaped with a smooth surface, and several have a characteristic central umbilication. The child is otherwise healthy and immunocompetent. The lesions are not pruritic and there is no associated lymphadenopathy. On closer examination, a white, cheesy material can be expressed from the central depression of some lesions. What is the most likely diagnosis?
Post-mortem examination of a patient reveals the following. What is this finding known as?

Treatment of choice for acute arsenic poisoning is:
Adrenocorticotropic hormone is the drug of choice in which of the following conditions?
Which of the following cyanotic heart diseases cause increased pulmonary blood flow? 1. Ebstein anomaly 2. Tetralogy of Fallot 3. Transposition of the great arteries (TGA) 4. Total anomalous pulmonary venous communication (TAPVC) Select the correct combination:
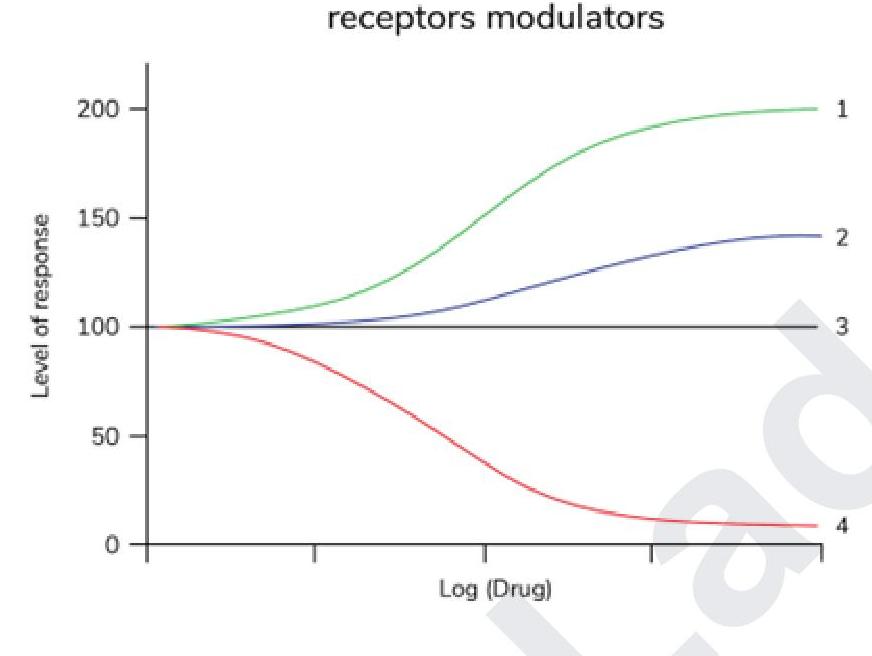
Which of the following statements is correct regarding the given graph?
Match the following antiarrhythmic drugs with their mechanism of action: | Mechanism of action | Drug | | :-- | :-- | | 1. Na+ channel blocker | A. Quinidine | | 2. K+ channel blocker | B. Digoxin | | 3. Na+K+ ATPase inhibitor | C. Esmolol | | 4. Beta-blocker | D. Ibutilide |
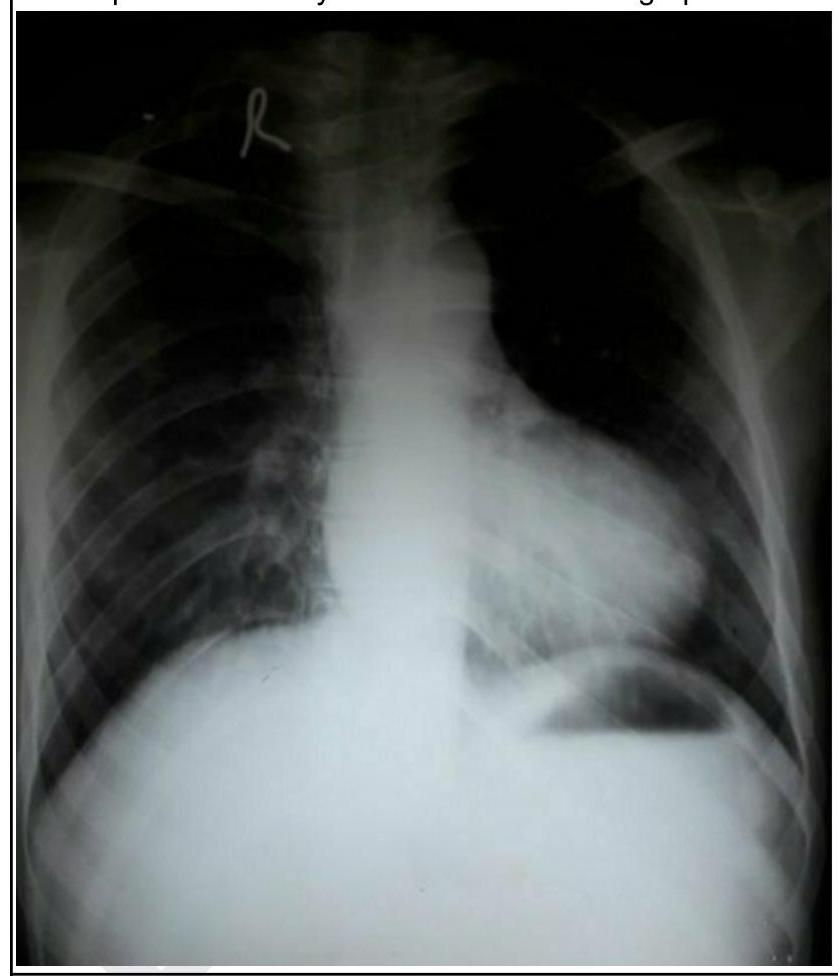
A child presents with cyanosis. His chest radiograph is shown below. What is the diagnosis?
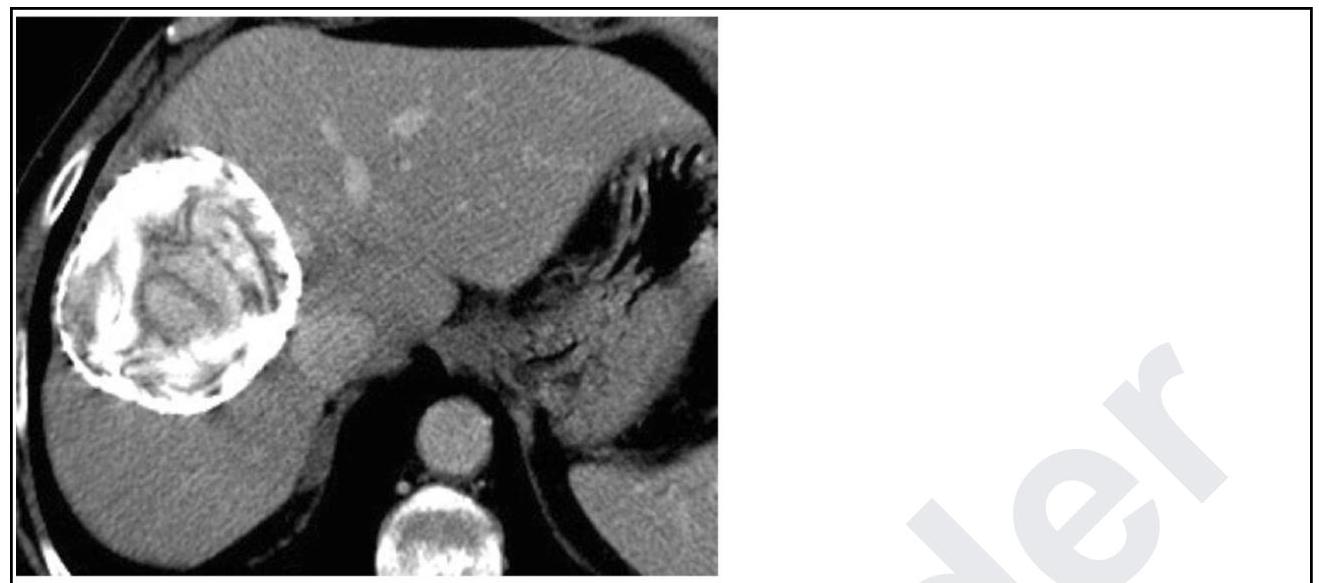
Identify the condition based on the non-contrast CT scan of a patient given below.