Thrombolysis can be considered in all of these conditions, except:
A young patient presents to the clinic with erythematous lesions over the exposed areas of the skin like hands, arms, chest, etc. she also complaints of arthralgia and breathlessness. Which among the following antibodies will be useful in diagnosing this condition?
A patient presented with violent, flinging movements. Where is the lesion causing the hemiballismus seen?
What is the most common site of abdominal tuberculosis?
A woman presents with altered sensorium, breathlessness, hypotension and bradycardia. Examination revealed non-pitting edema of the extremities. She has a long -standing history of weight gain, constipation, cold intolerance, and menorrhagia. What is the most likely diagnosis?
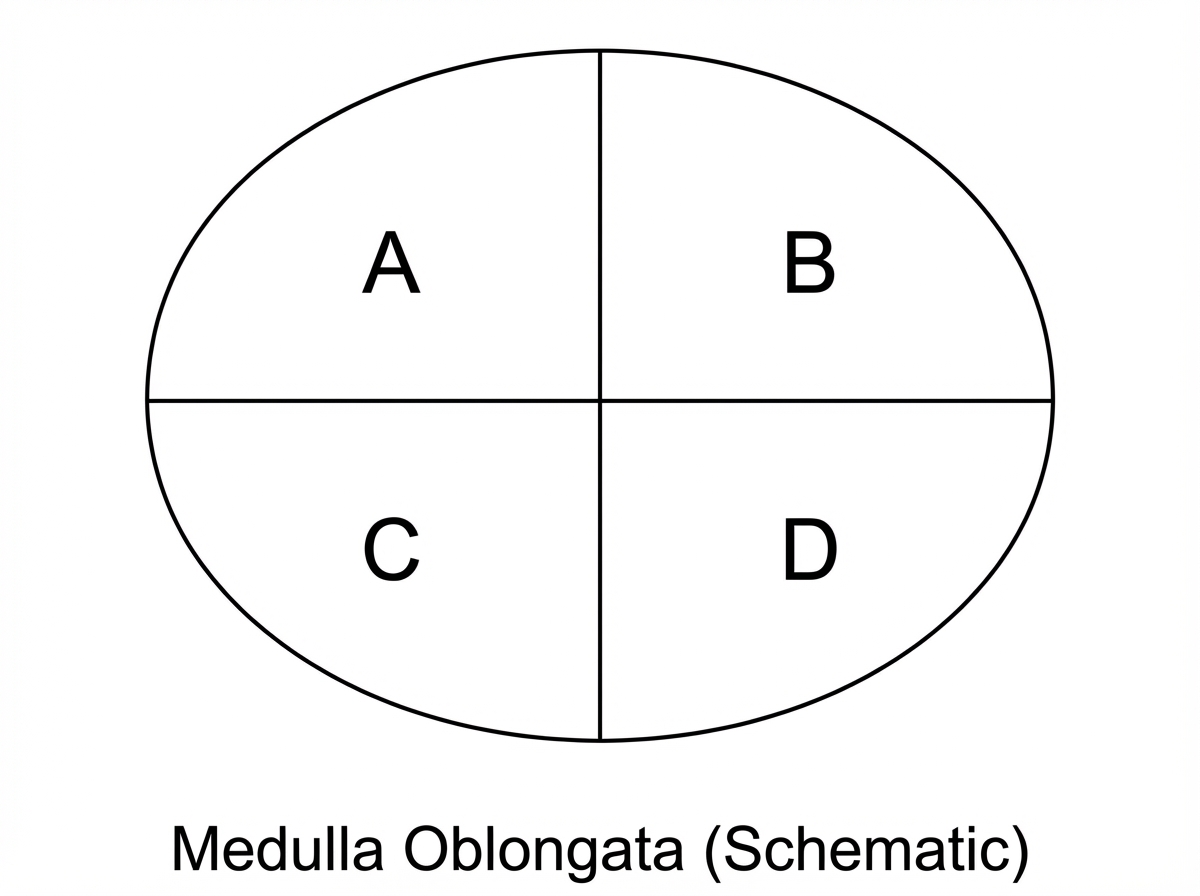
A patient presented with ipsilateral Horner's syndrome, ipsilateral loss of pain and temperature sensations in the face, vertigo with numbness and loss of sweating and dysarthria on the contralateral side. All these symptoms are caused due to a lesion in:
Seminal vesicles and vas deferens would be bilaterally absent congenitally in which of the following conditions?
All the following are criteria for SIRS, except