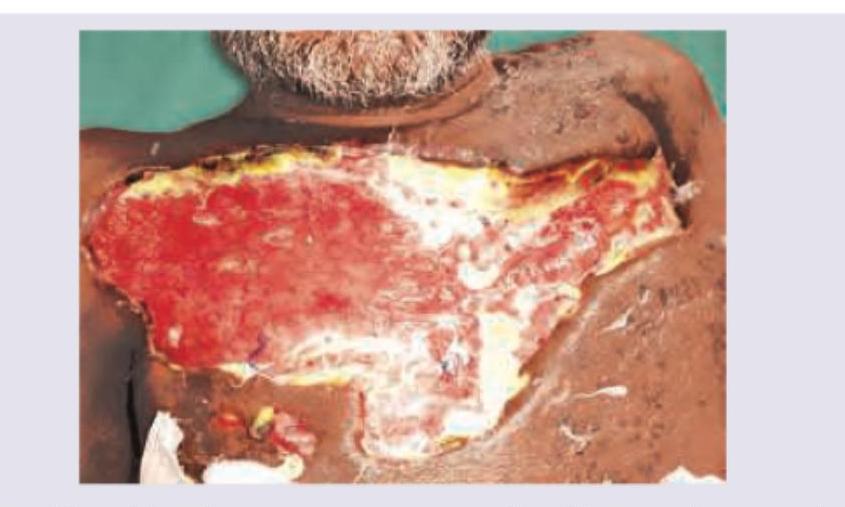
A 30-year-old construction worker had a partial traumatic nail avulsion. 3 weeks later he presents with the presentation shown below. What is the diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A 30-year-old construction worker had a partial traumatic nail avulsion. 3 weeks later he presents with the presentation shown below. What is the diagnosis?

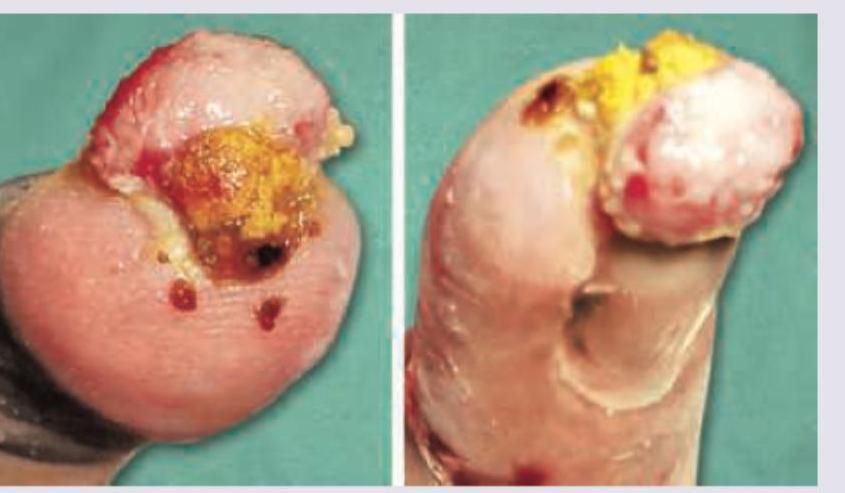
A 50-year-old smoker and hypertensive patient presents with the lesion shown below. It is painful and present bilaterally. Peripheral pulses are palpable. What is the diagnosis?
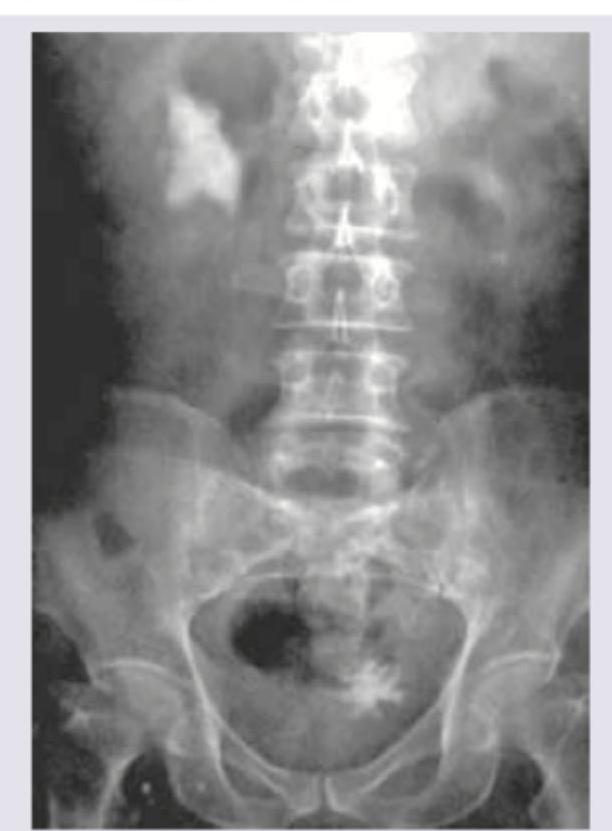
Which is incorrect about the procedure shown in the patient with right flank pain?
The image shows:
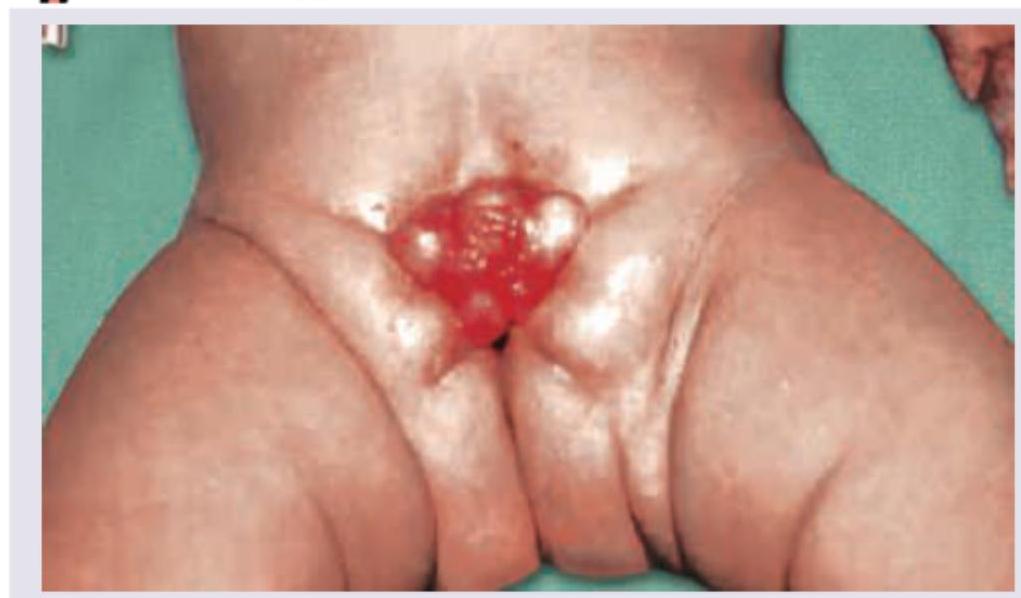
Identify the instrument shown in the image:

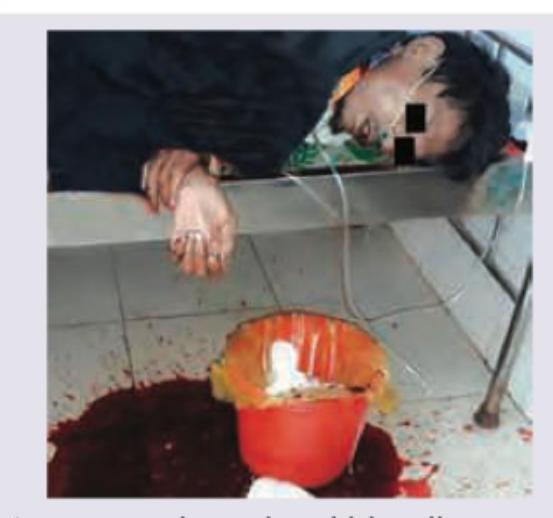
Which is correct about hematemesis (upper GI bleeding) in this patient?
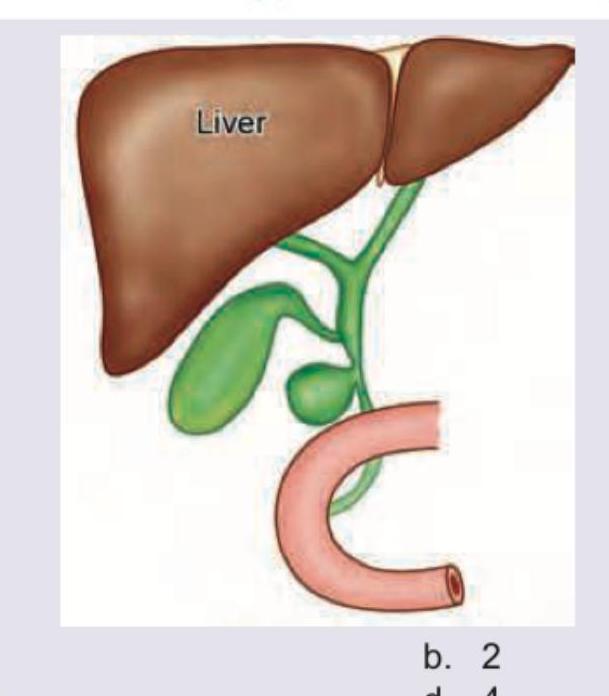
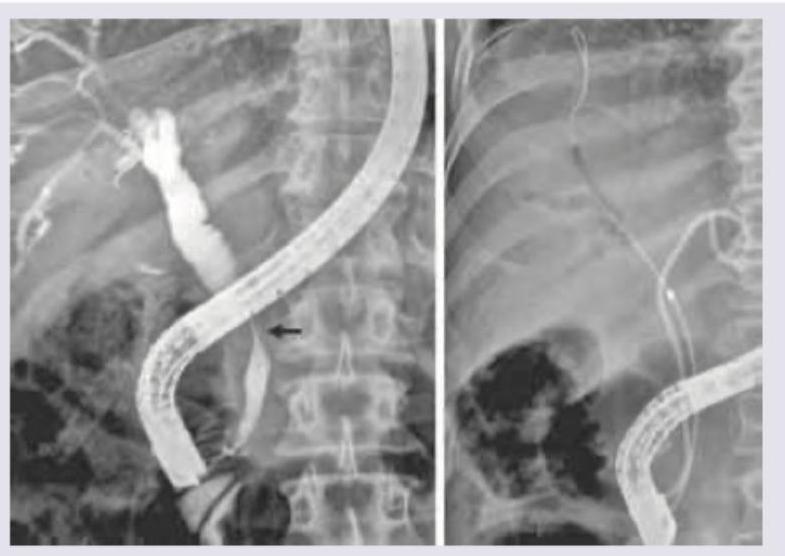
What type of choledochal cyst is shown in the image?
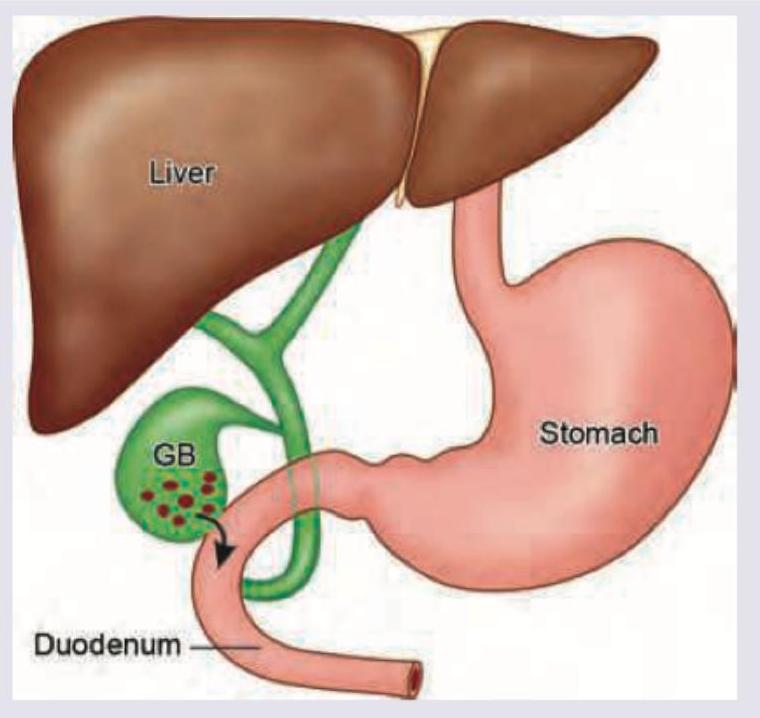
A patient with chronic cholelithiasis develops the complication shown in the image below. This leads to development of:
Which classification is used to evaluate the condition shown in the image below?
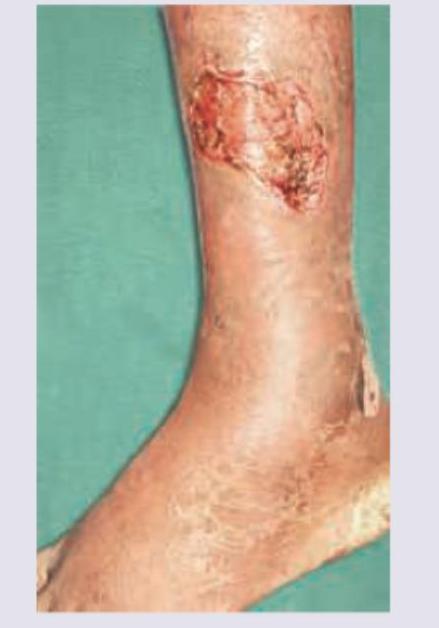
An HIV positive patient presents with symptoms of toxemia and foul smelling discharge from the lesion shown below. What is the diagnosis?