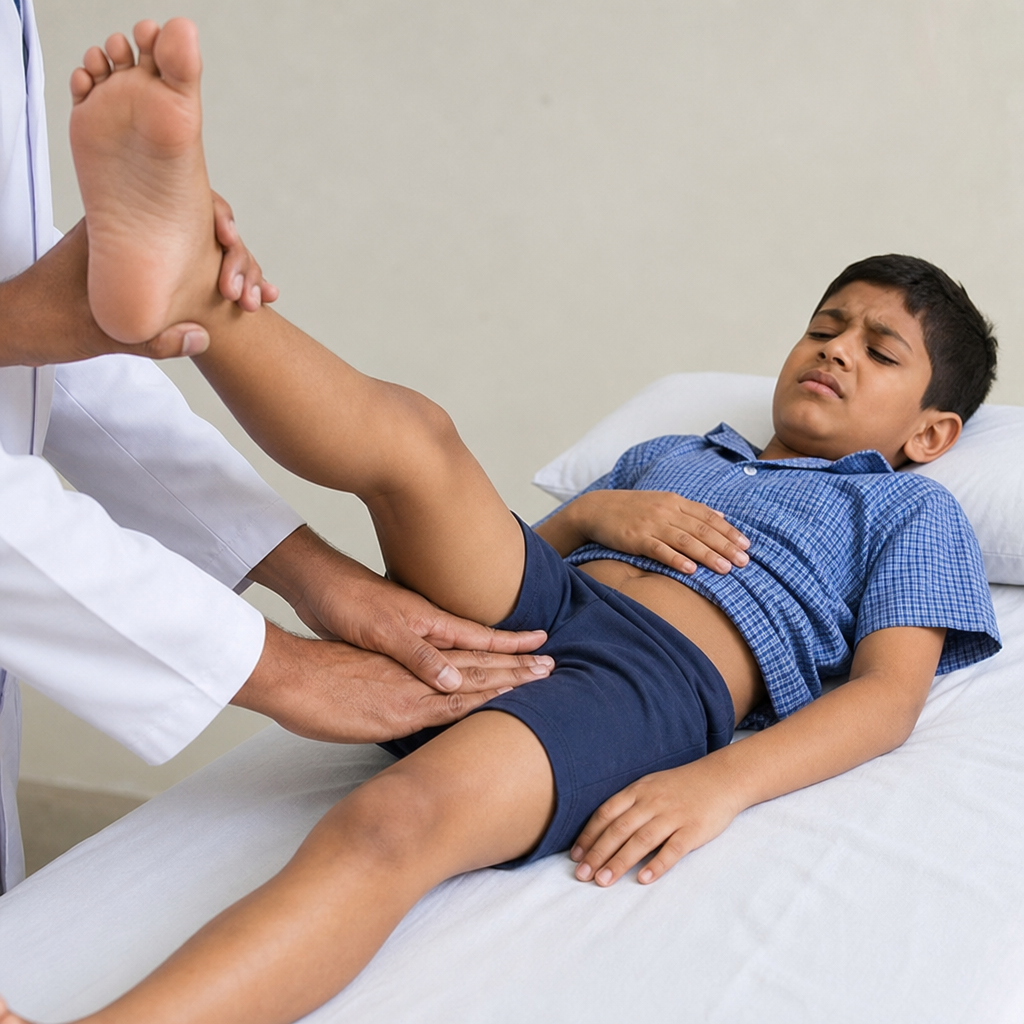
You are asked to put a 22-gauge cannula in a patient. Which of the following cannula will you put?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
You are asked to put a 22-gauge cannula in a patient. Which of the following cannula will you put?

A middle-aged man came to you with itchy rash caused by the following organism. Identify the condition: (AIIMS Nov 2017)
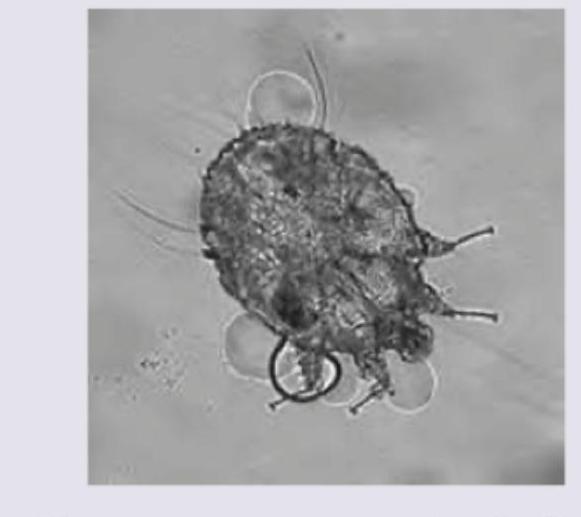
Identify the condition which is present since birth: (AIIMS May 2017)
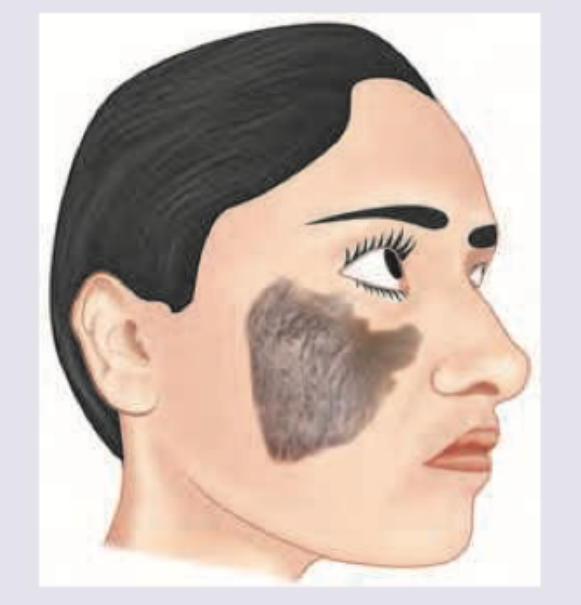
A child has been brought with the following scalp lesion with history of itching in scalp and hair loss for past 2 months. Which of the following is useful for diagnosis of this patient? (AIIMS May 2017)
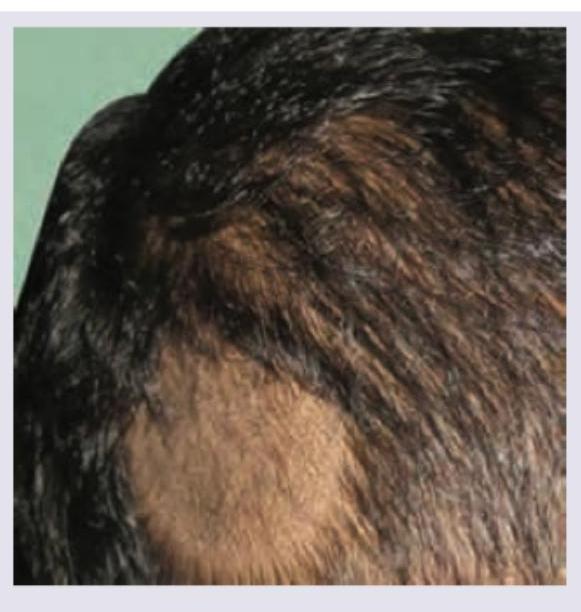
The following patient presented to the OPD with history of hair loss. There was no erythema, scarring or scratching. Diagnosis is:
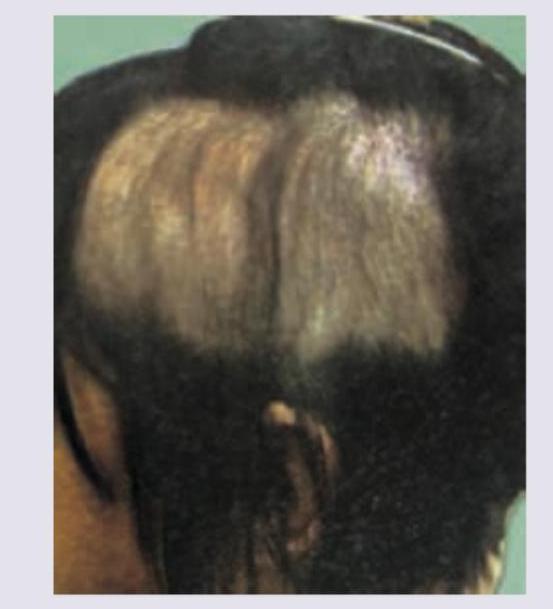
A patient with symptomatic cholecystitis underwent a cholecystectomy. The following specimen was obtained. What is the diagnosis?
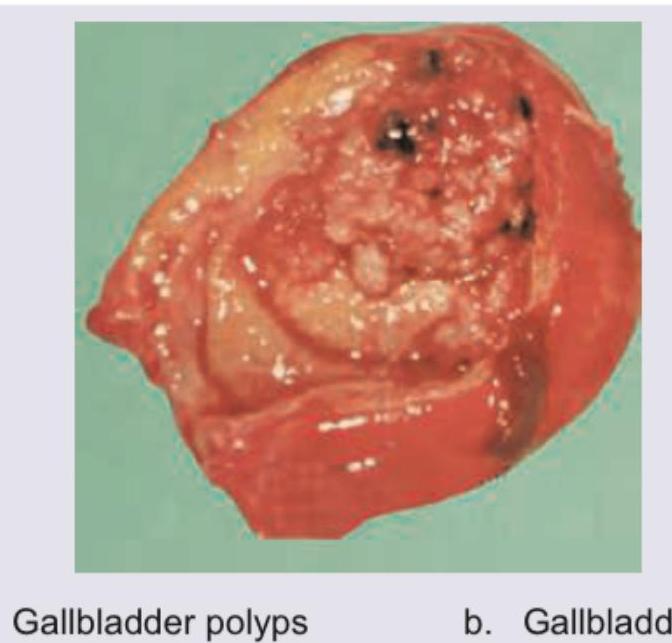
A 50-year-old man went for his annual medical check-up. CT scan is shown below. Diagnosis is?
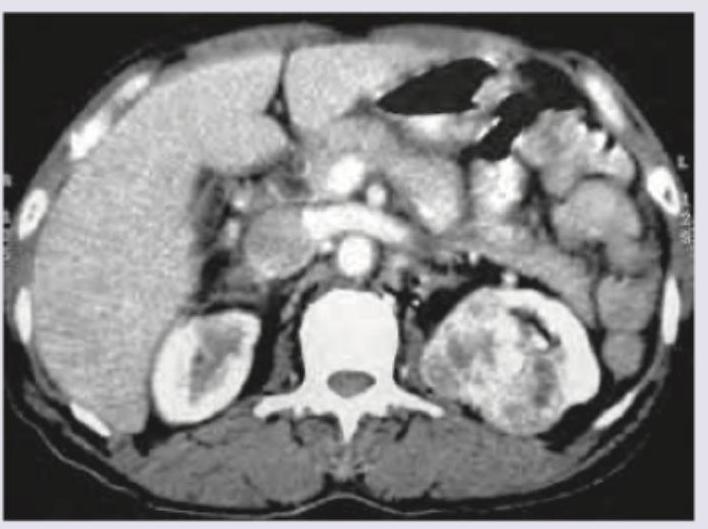
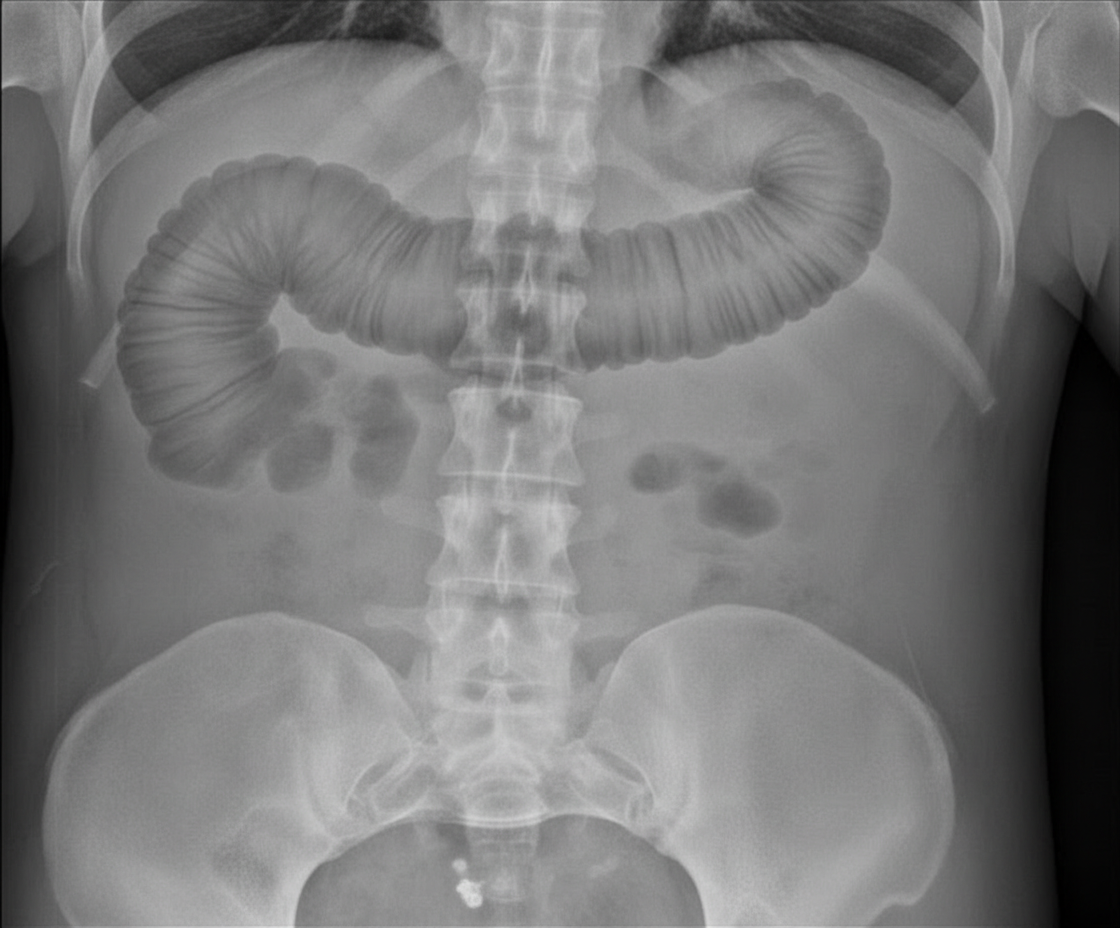
A 30-year-old man presents with abdominal pain and fever for one day. He has history of diarrhea for last several months which contains blood. What is the diagnosis?
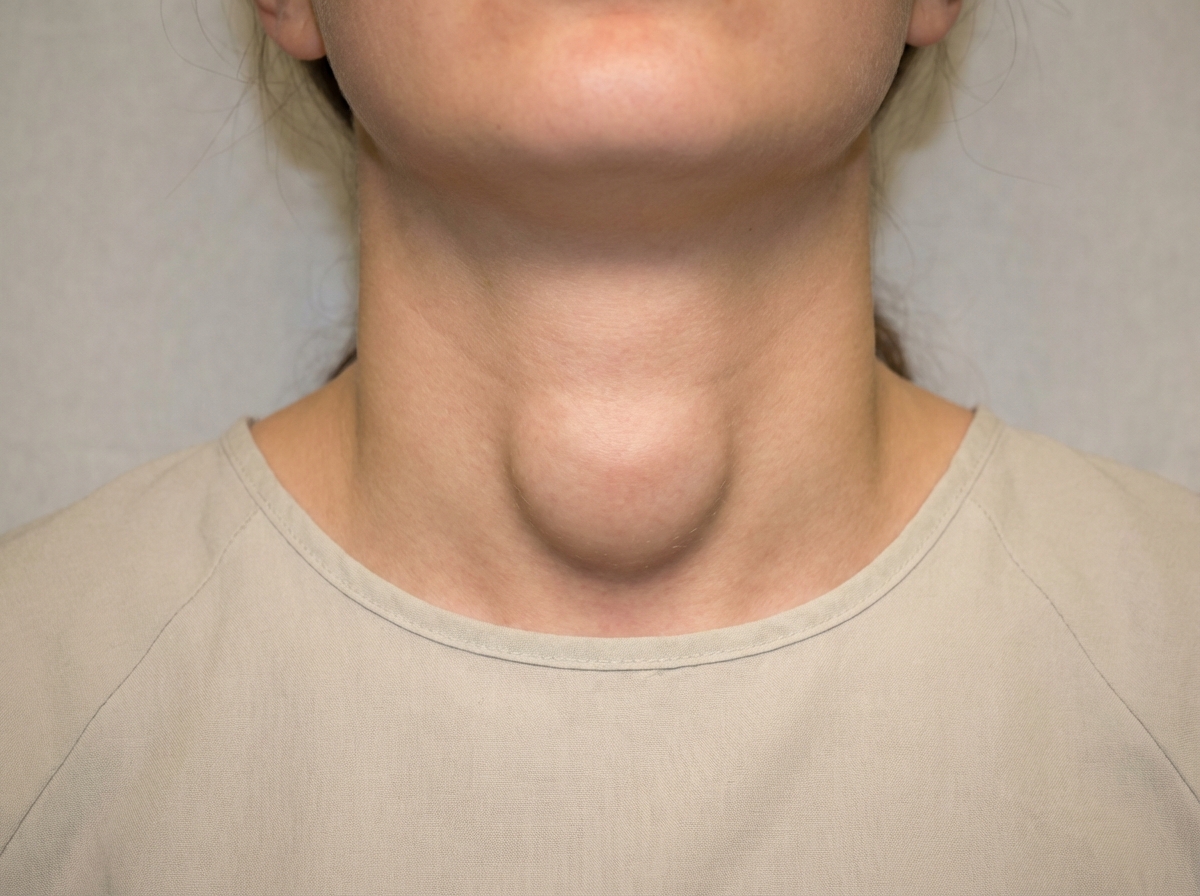
A 25-year-old patient presents with a neck swelling which moves with deglutition as shown below. Your diagnosis is?
An 8-year-old boy presents to the casualty with history of fever and abdominal pain. On examination he was febrile and the pulse rate was 104/min. Identify the sign?