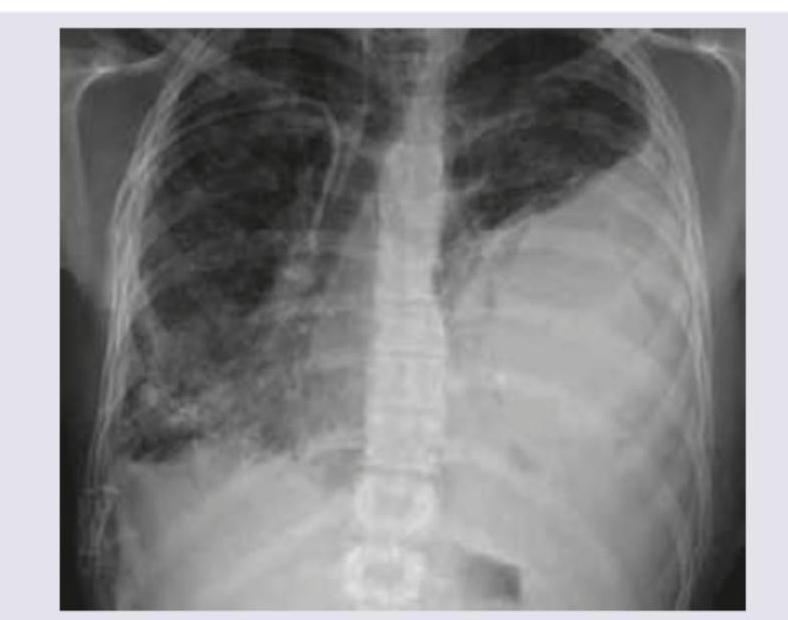
A child has a pruritic rash as shown below. His mother is an asthmatic. Comment on the diagnosis:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A child has a pruritic rash as shown below. His mother is an asthmatic. Comment on the diagnosis:

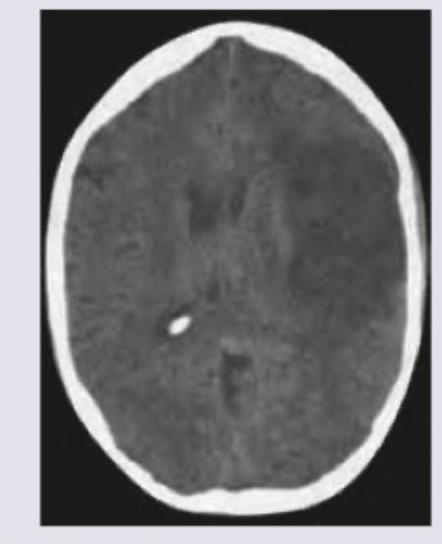
A middle-aged patient presents with history of left sided weakness for 2 days. Currently the patient is extremely drowsy and underwent a NCCT brain. Which of the following is the best treatment for this patient? (AIIMS Nov 2017)
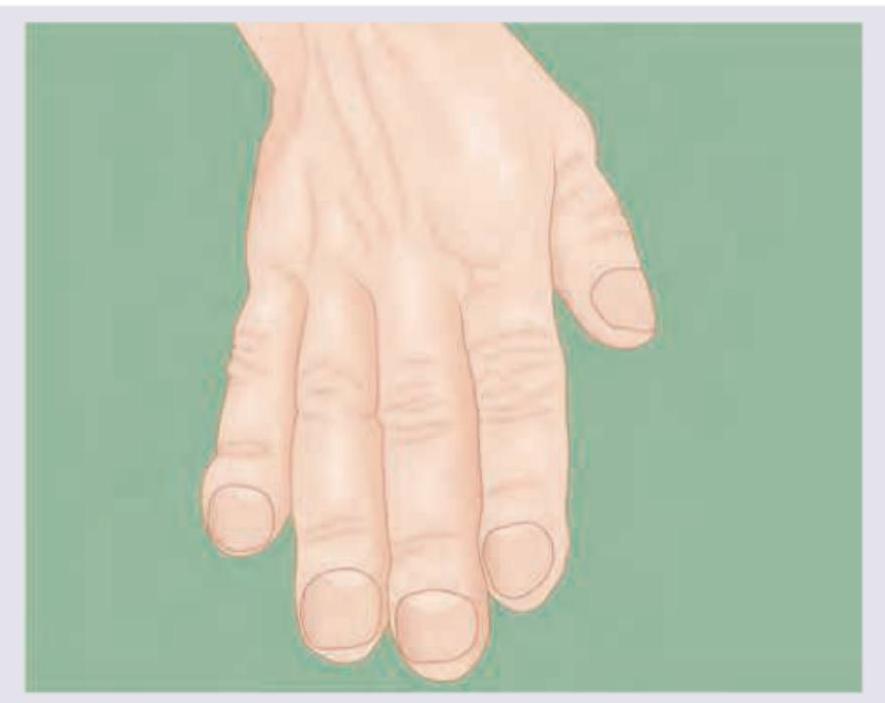
A 50-year-old man presents with frontal bossing, enlarged tongue and following appearance of hand. Which of the following tests should be done in this patient?
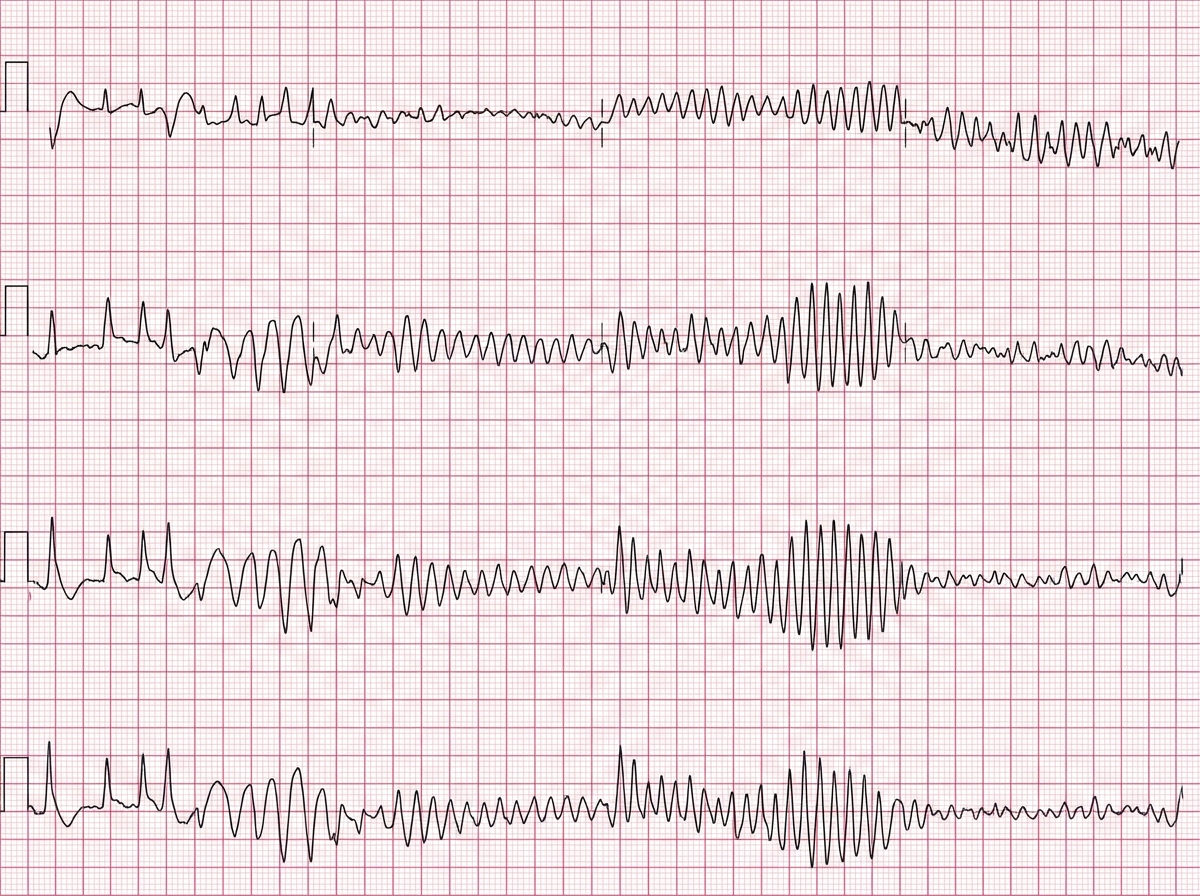
This 50-year-old patient developed syncope after having a coffee. ECG was done .Which is the most appropriate therapy for a patient suffering from the condition shown below?
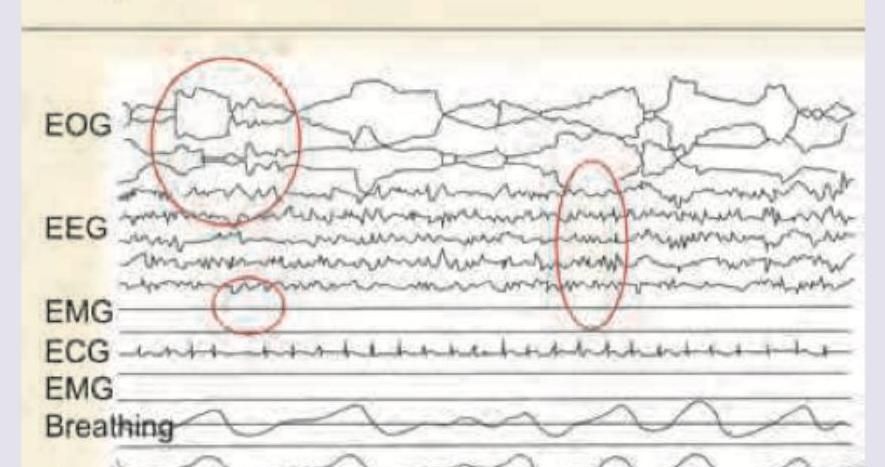
Identify the sleep stage in the following Polysomnograph.
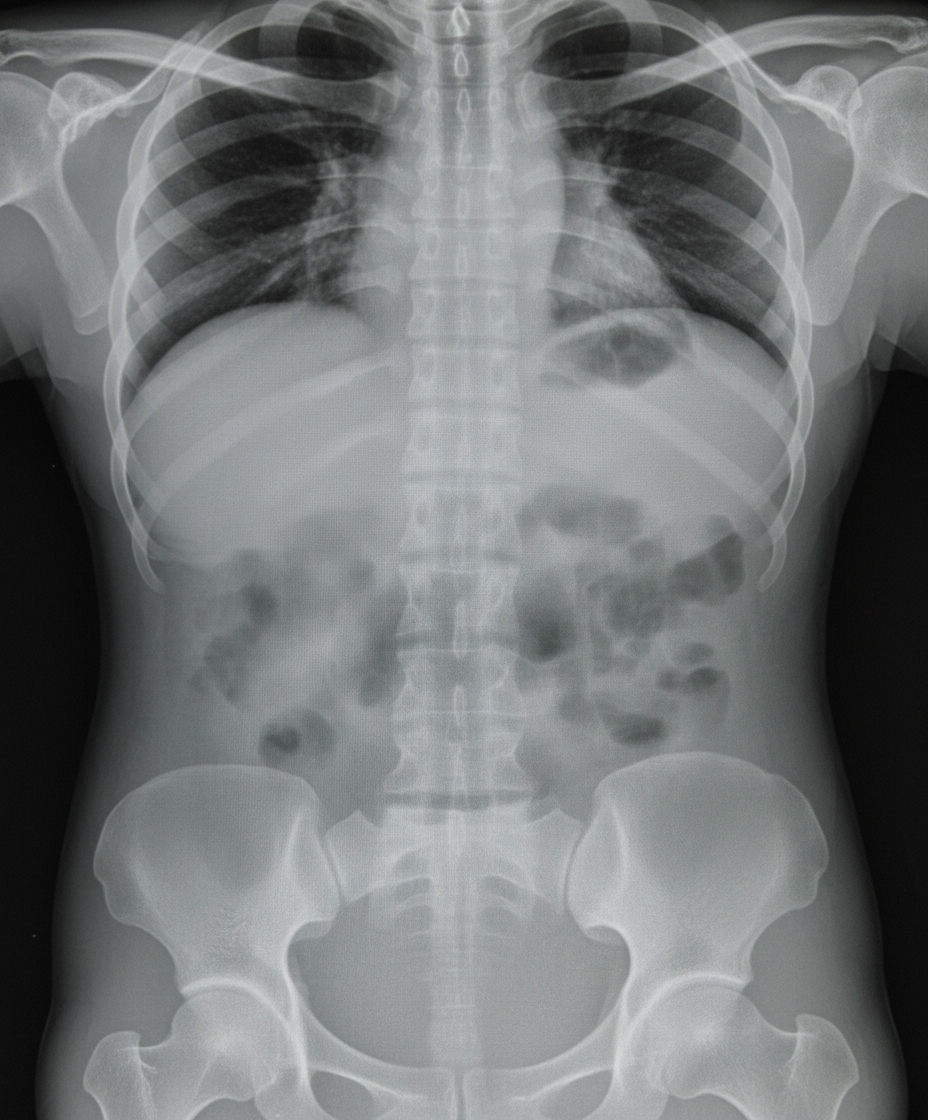
A patient presents with complaints of fever and abdominal distention. He is having history of bloody diarrhea off and on for previous 6 months. X-ray abdomen is shown below. What is the diagnosis?
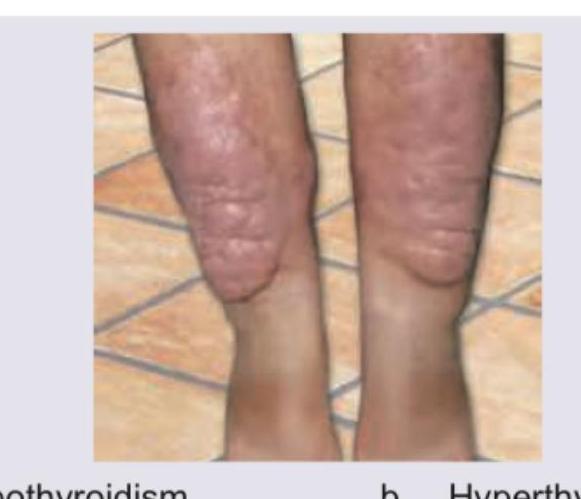
Comment on the diagnosis of the image shown below. (AIIMS Nov 2017)
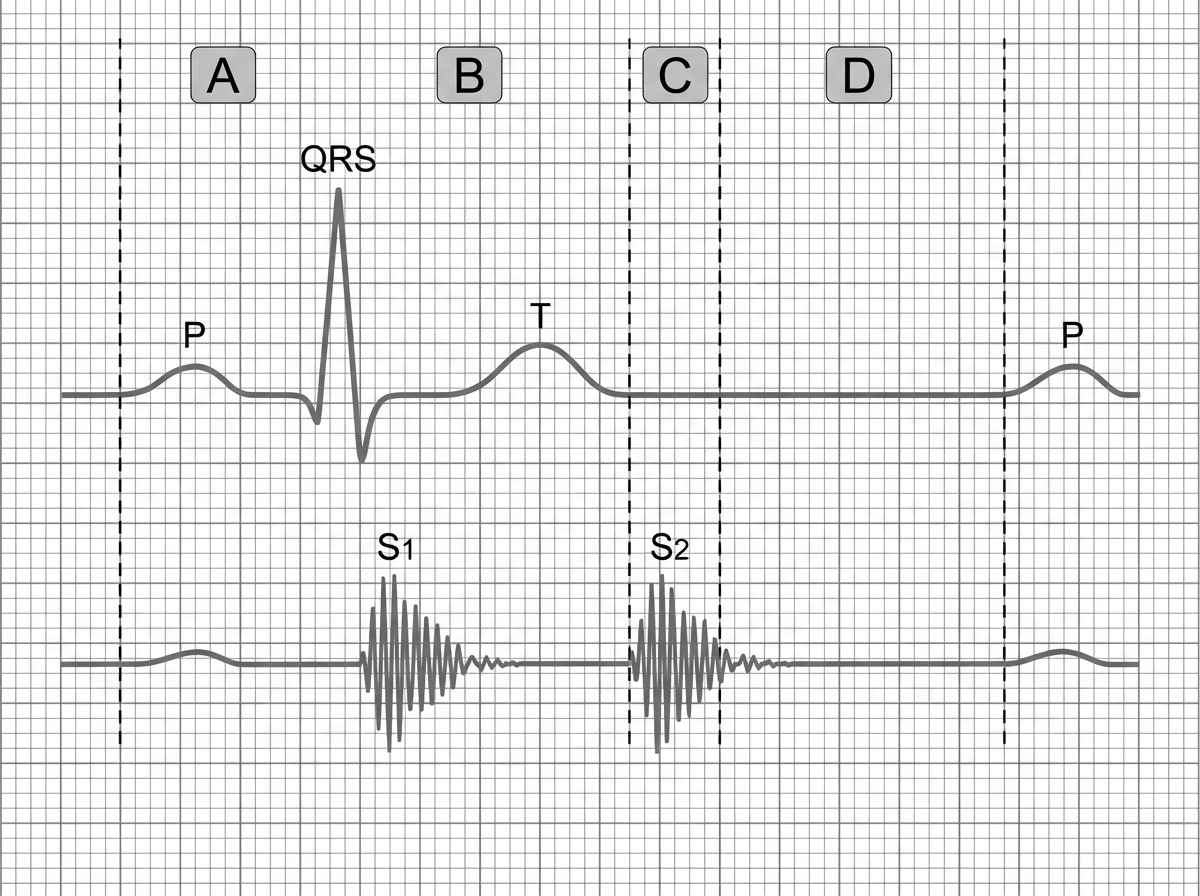
Phonocardiogram tracing is shown below with corresponding ECG. Identify the phase corresponding with $S_{2}$ in phonocardiogram.
A patient presented with sudden onset difficulty in breathing with RR 28/min, normal blood pressure. X-ray was taken which is given below. What is the diagnosis?
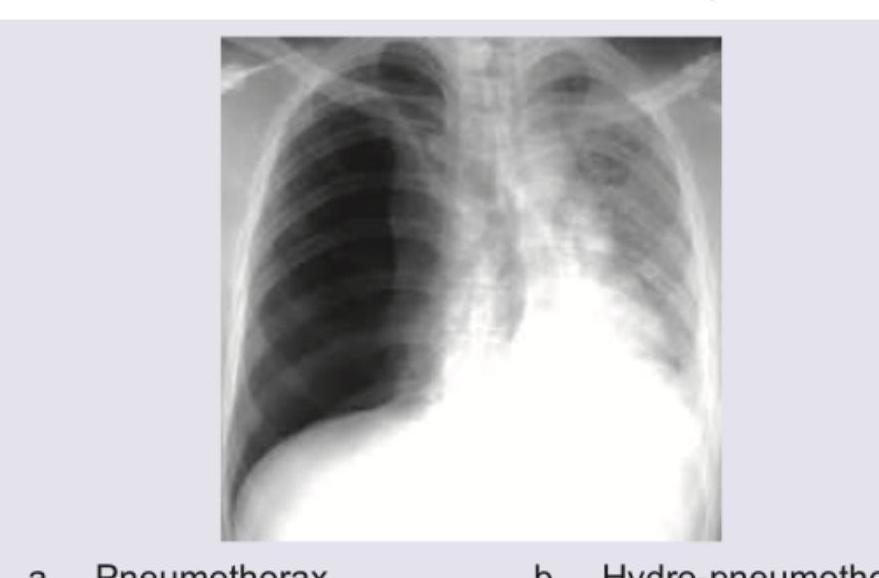
A car accident patient complains of breathlessness. On examination BP is $110 / 70 \mathrm{mmHg}$ with GCS of 15/15. On examination, trachea is deviated to the right side, with reduced breath sounds in left infra-axillary area and inframammary areas. $S_{1}$ and $S_{2}$ are normal in intensity and splitting. CXR is shown below. What is the best step in management of the patient?