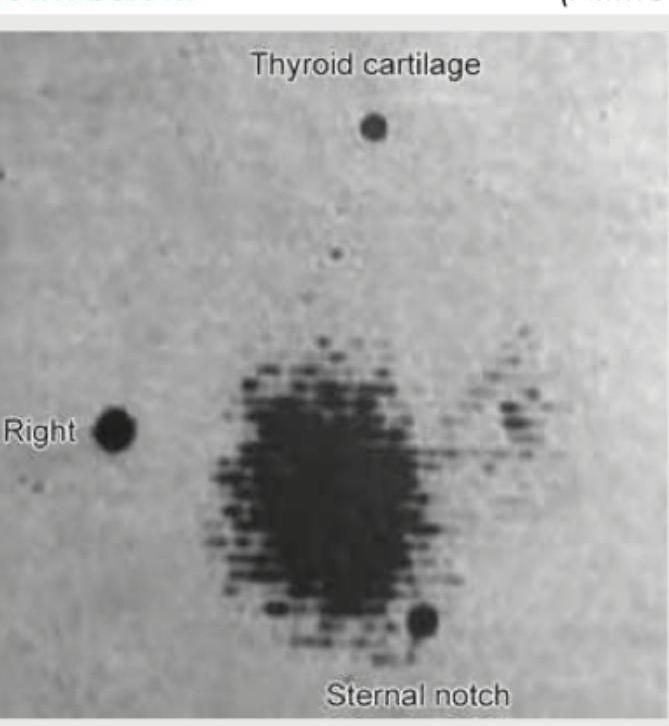
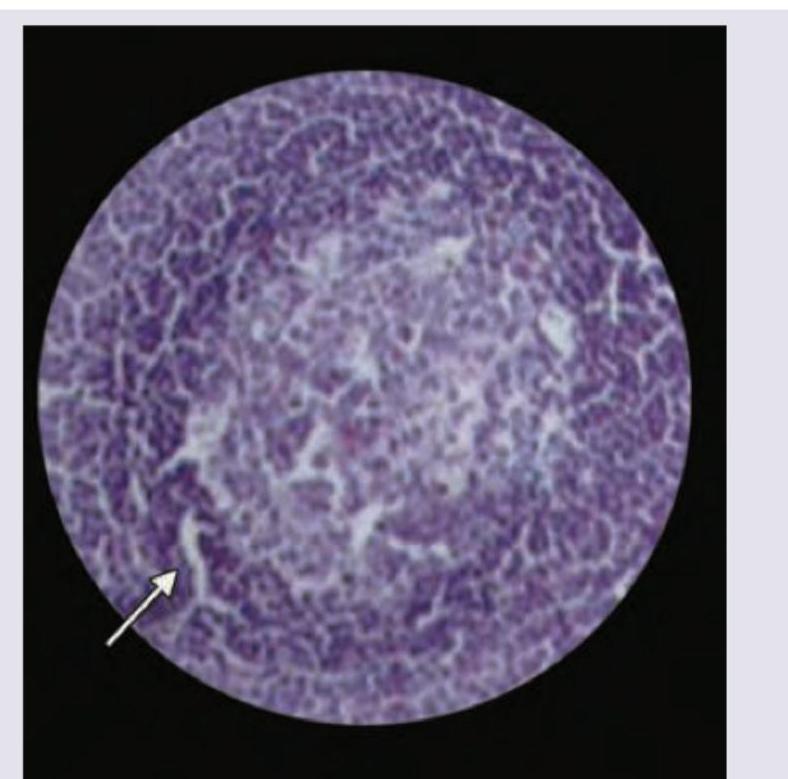
Which of the following area is marked in the histology of lymph node? (AIIMS May 2017)
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which of the following area is marked in the histology of lymph node? (AIIMS May 2017)

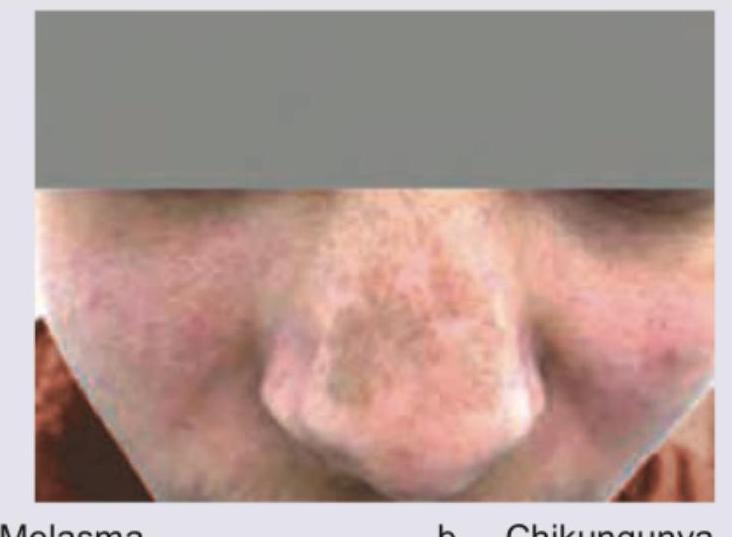
A 30-year-old male presents with joint pain and NSAIDs were prescribed. After one week, joint pain is persisting and he has developed brownish discoloration over nose as shown in the figure. This was due to: (AIIMS Nov 2017)
A patient with HIV develops fever weight loss and diarrhea. Fecal examination shows isospora belli. He was given treatment with TMP - SMX. Diarrhea subsided but fever persisted. Bone marrow examination showed the following picture with intracellular fungi. Which of the following statements is wrong? (AIIMS Nov 2017)
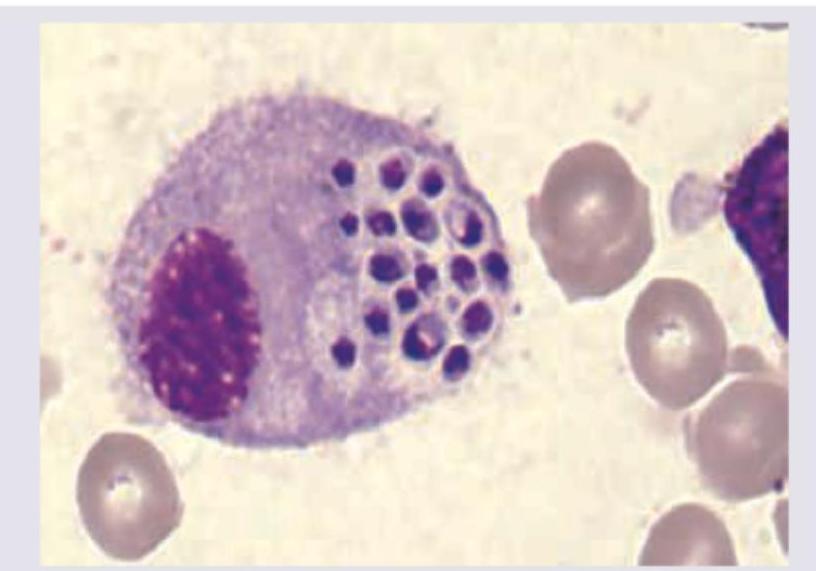
Which causative organism is responsible for this disease?
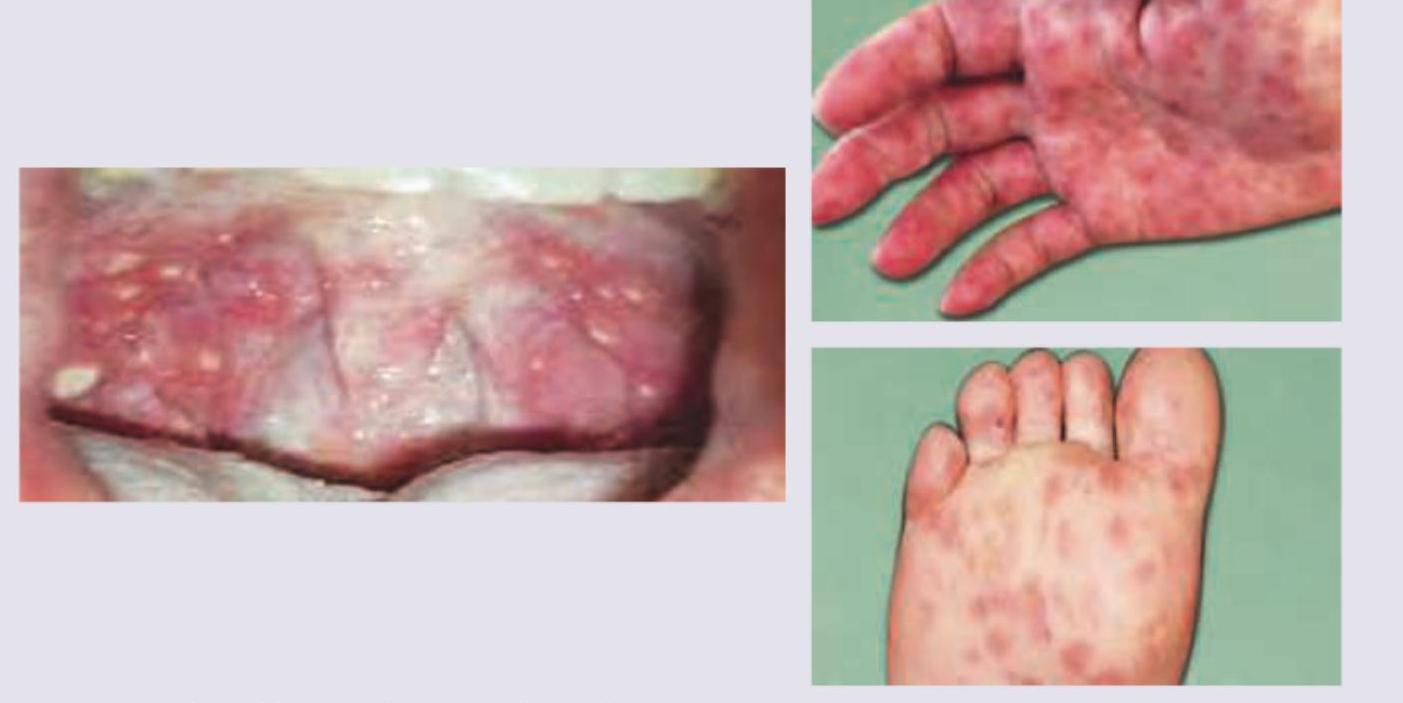
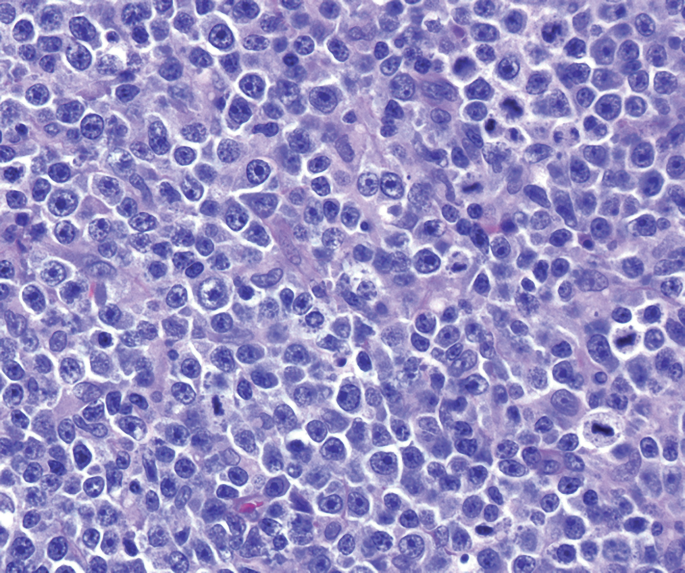
A 35-year-old presented with fever. On examination he had enlarged and ulcerated tonsils. Since peripheral smear shows lymphocytosis, monospot test was done which is negative. Tonsillectomy was done and stained section is shown below. Large cells mixed with lymphocytes are seen. The cells are positive for CD20, EBVLMP-1, MUM1, CD 79a and CD 15 negative. The background cells are positive for CD3. Diagnosis is: (AIIMS May 2017)
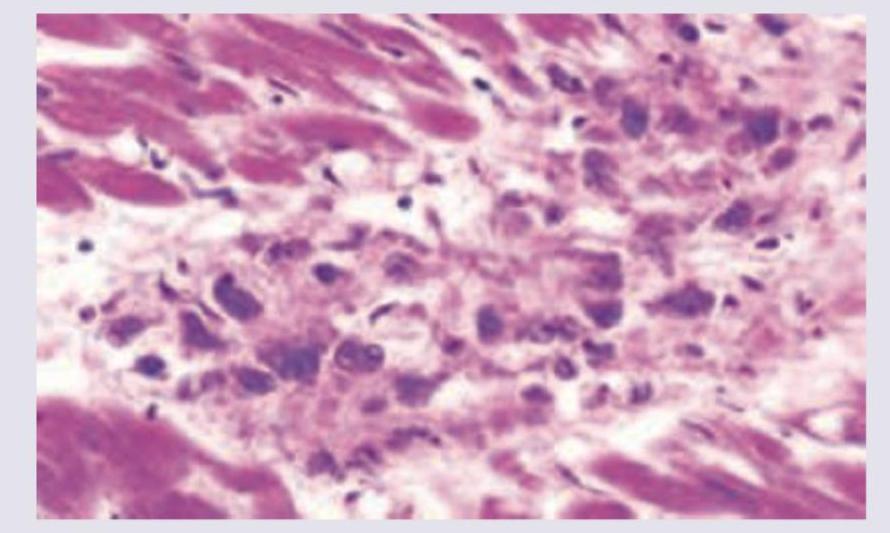
A patient presented with mitral valve stenosis, identify the diagnosis from the mitral valve histopathology depicted below. (AIIMS Nov 2017)
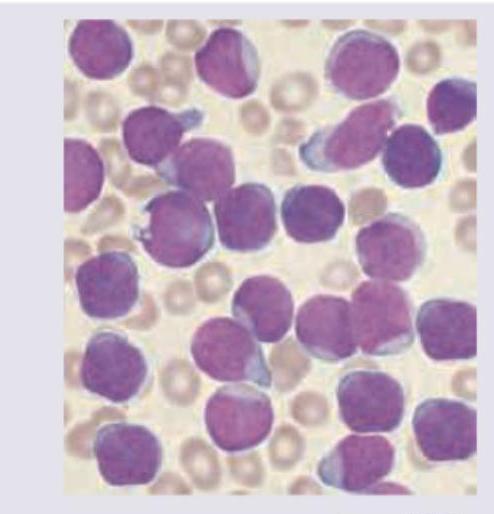
A 7-year-old boy presents with fever and weight loss. On examination he had pallor with lymphadenopathy. Peripheral smear is shown below. Diagnosis is: (AIIMS May 2017)
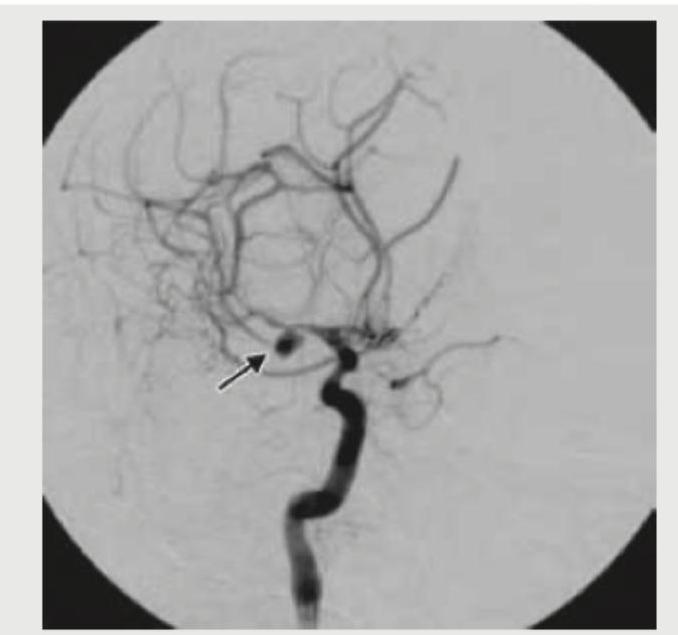
The digital subtraction angiography given below shows? (AIIMS Nov 2017)
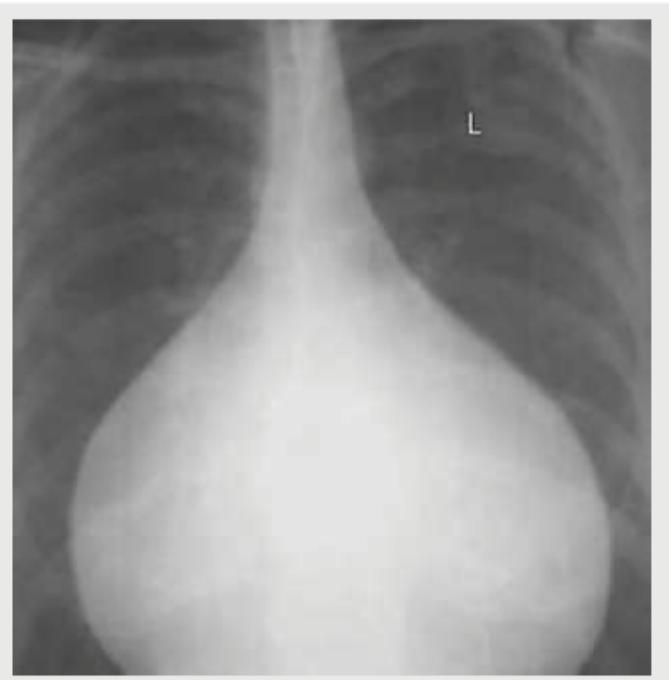
Which is not a finding of the Chest X-ray shown below? (AIIMS May 2017)
Comment on the diagnosis from the thyroid scan shown below. (AIIMS May 2017)