INI-CET 2017 — Ophthalmology
7 Previous Year Questions with Answers & Explanations
Identify the instrument used: (AIIMS Nov 2017)

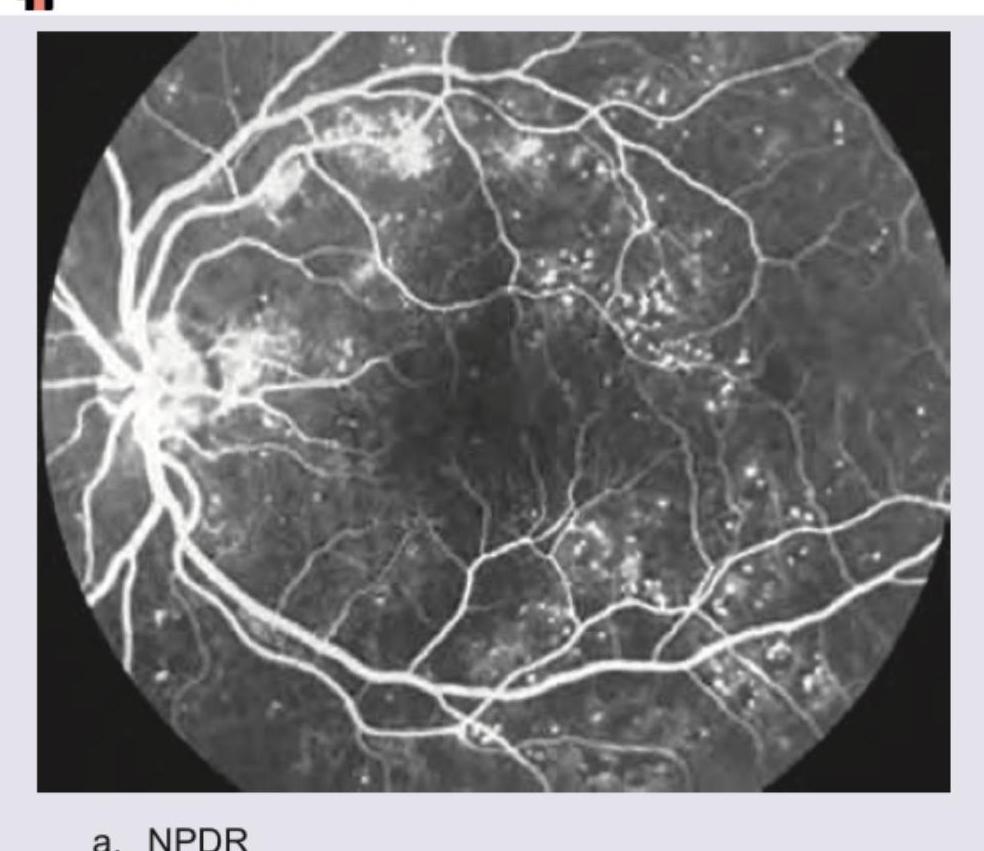
Identify the FFA picture:
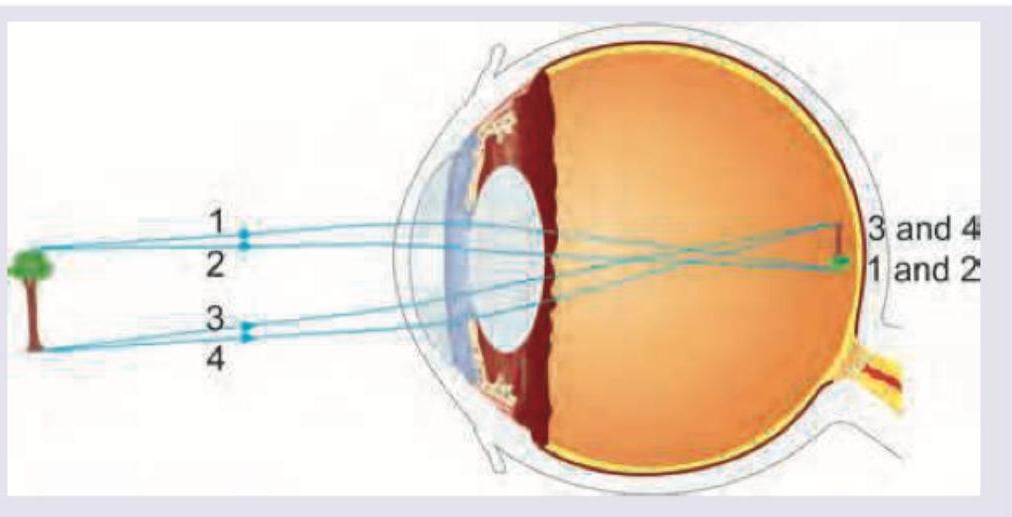
Identify the refractive error shown in the image:
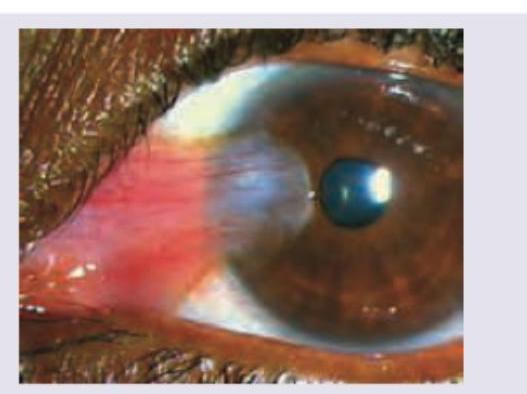
A patient has the following presentation. After administration of an intravenous drug to the patient, in 6 minutes his symptoms have resolved. The diagnosis of the patient is:
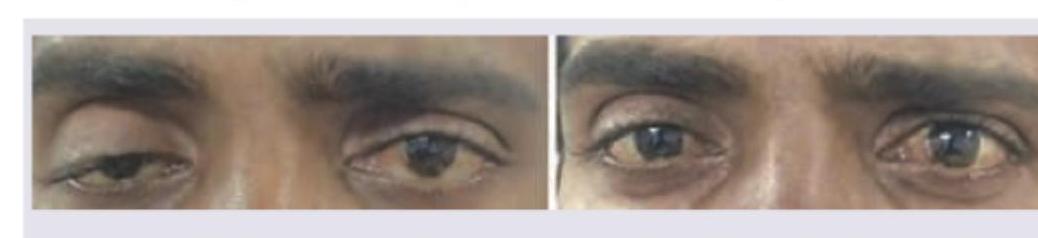
What is the diagnosis?
A 60-year-old male underwent a cataract surgery. After 1 year he came with complaints of diminished vision and the finding shown in the image. Diagnosis is?
A 60-year-old male underwent a cataract surgery. After 1 year he came with complaints of diminished vision and the finding shown in the image. Diagnosis is?
INI-CET 2017 - Ophthalmology INI-CET Practice Questions and MCQs
Question 1: Identify the instrument used: (AIIMS Nov 2017)
- A. Episiotomy scissors (Correct Answer)
- B. Dissection scissors
- C. Mayo scissors
- D. Metzenbaum scissors
Explanation: ***Episiotomy scissors*** - These scissors are characterized by their **blunt, angled tip** on one blade, which is designed to protect the fetal head during an episiotomy. - The image clearly shows this specific design, making them ideal for cutting soft tissues in a controlled manner without puncturing underlying structures. *Dissection scissors* - Dissection scissors typically have **sharp tips**, either straight or curved, and are used for cutting and separating tissues with precision. - They lack the blunt, angled tip characteristic of episiotomy scissors. *Mayo scissors* - **Mayo scissors** are heavy-duty scissors, typically used for cutting **fascia, sutures, and dense tissues**. - They often have straight or slightly curved blades without the protective blunt tip seen in episiotomy scissors. *Metzenbaum scissors* - **Metzenbaum scissors** are known for their **long handles and relatively short, delicate blades**, designed for cutting and dissecting fine, delicate tissues. - Their blades are typically slender and do not feature the angled, blunt tip of episiotomy scissors.
Question 2: Identify the FFA picture:
- A. NPDR (Correct Answer)
- B. PDR
- C. Familial dominant drusen
- D. Birdshot choroidopathy
Explanation: ***NPDR*** - The image shows areas of **capillary non-perfusion** (dark areas without visible blood flow) and **microaneurysms** (small bright dots due to damaged capillaries). These are characteristic findings of **Non-Proliferative Diabetic Retinopathy (NPDR)** on fluorescein angiography. - There is no evidence of neovascularization, which is the hallmark of proliferative diabetic retinopathy. *PDR* - **Proliferative Diabetic Retinopathy (PDR)** is characterized by the presence of **neovascularization** (new, abnormal blood vessel growth) on the retina or optic disc. - This image does not show any signs of neovascularization, which would appear as brightly fluorescing, tangled vessels. *Familial dominant drusen* - **Familial dominant drusen** are typically seen as yellow-white deposits under the retinal pigment epithelium and would manifest on FFA as **hyperfluorescent spots**, but usually with a different distribution and appearance than the microaneurysms seen here. - This image reflects widespread microvascular damage consistent with a retinal vascular disease, not primarily drusen. *Birdshot choroidopathy* - **Birdshot choroidopathy** is a chronic, bilateral posterior uveitis characterized by multiple, depigmented choroidal lesions (birdshot lesions). - On FFA, these lesions would typically show **hypofluorescence** in the early phases due to blocked choroidal fluorescence and possible late staining, which is not depicted in this image.
Question 3: Identify the refractive error shown in the image:
- A. Myopia
- B. Hypermetropia
- C. Astigmatism (Correct Answer)
- D. Presbyopia
Explanation: ***Astigmatism*** - The image shows that light rays from a single point source are **not focused at a single point** on the retina, but rather spread across multiple focal points or a line. This pattern is characteristic of **astigmatism**, where the eye's cornea or lens has an irregular curvature. - Specifically, rays 1 and 2 converge at one point, while rays 3 and 4 converge at a different point, indicating that the eye has different refractive powers along different meridians, which defines **astigmatism**. *Myopia* - In **myopia (nearsightedness)**, light rays from a distant object focus **in front of the retina**, not at multiple planes or lines as depicted. - Myopia would show all rays converging to a single point before reaching the retina, resulting in a blurry image. *Hypermetropia* - In **hypermetropia (farsightedness)**, light rays from a distant object focus **behind the retina**, assuming the eye is unaccommodated. - This condition would show the rays converging to a single point beyond the retinal plane, not divergent focal points within the eye. *Presbyopia* - **Presbyopia** is an age-related condition where the eye's **lens loses its flexibility**, making it difficult to focus on nearby objects. - It primarily affects near vision and does not typically involve the multiple focal points for distant vision as shown in the image.
Question 4: A patient has the following presentation. After administration of an intravenous drug to the patient, in 6 minutes his symptoms have resolved. The diagnosis of the patient is:
- A. Myasthenia gravis (Correct Answer)
- B. Sixth nerve palsy
- C. Third nerve palsy
- D. Tolosa-Hunt syndrome
Explanation: The question refers to an accompanying image (not provided in the text, but essential for context) showing a patient with **ptosis** (drooping eyelid) and possibly other ocular muscle weakness. The key information is that symptoms resolve within 6 minutes after administration of an intravenous drug. This rapid and complete resolution of symptoms following drug administration is highly characteristic of a specific condition and a specific diagnostic test. ***Myasthenia gravis*** - The rapid resolution of symptoms (ptosis and possibly other ocular muscle weakness) within 6 minutes after intravenous drug administration is the hallmark of a positive **Tensilon test**. - The **Tensilon test** involves injecting **edrophonium**, a short-acting acetylcholinesterase inhibitor, which temporarily increases acetylcholine at the neuromuscular junction, improving muscle strength in patients with **myasthenia gravis**. *Sixth nerve palsy* - Sixth nerve palsy (abducens nerve palsy) causes **diplopia** (double vision) and an inability to abduct the affected eye. - While symptoms may fluctuate or improve with treatment, they would not resolve completely in 6 minutes with a diagnostic agent like edrophonium. *Third nerve palsy* - Third nerve palsy (oculomotor nerve palsy) can cause **ptosis**, **diplopia**, and impairment of eye movements (inability to adduct, elevate, or depress the eye). - Nerve palsies are structural or neurological deficits that do not rapidly reverse with a cholinergic agonist like edrophonium. *Tolosa-Hunt syndrome* - Tolosa-Hunt syndrome is a rare inflammatory disorder characterized by **painful ophthalmoplegia** (paralysis of eye muscles), often affecting the third, fourth, and/or sixth cranial nerves. - It typically responds to corticosteroids, but symptoms would not resolve in 6 minutes with an intravenous drug, and the diagnostic approach is different.
Question 5: What is the diagnosis?
- A. Sixth nerve palsy
- B. Myasthenia gravis
- C. Third nerve palsy (Correct Answer)
- D. Tolosa-Hunt syndrome
Explanation: ***Third nerve palsy*** - The image shows **ptosis** (drooping of the eyelid) and **pupil dilation** with the eye deviated **down and out**, which are classic signs of a complete third nerve palsy. - The **oculomotor nerve (CN III)** innervates most extraocular muscles (**superior, medial, inferior recti, and inferior oblique**), the **levator palpebrae superioris**, and the **parasympathetic fibers to the pupillary constrictor muscle**. *Sixth nerve palsy* - A sixth nerve palsy (**abducens nerve**) would cause an inability to **abduct the eye** (move it outwards) leading to an **esotropia** (eye turned inward at rest) and **horizontal diplopia**, which is not depicted. - Symptoms primarily affect the **lateral rectus muscle**. *Myasthenia gravis* - Myasthenia gravis can cause **ptosis** and **diplopia**, but typically presents with **variable and fluctuating weakness** that worsens with fatigue. - It does not usually cause the fixed, specific pattern of strabismus and pupillary involvement seen in a severe third nerve palsy. *Tolosa-Hunt syndrome* - Tolosa-Hunt syndrome is a **painful ophthalmoplegia** caused by **non-specific inflammation** in the cavernous sinus or orbital apex. - While it can affect cranial nerves III, IV, V1, and VI, leading to **ophthalmoplegia** and **ptosis**, the defining feature is often **severe orbital pain**, which cannot be assessed from the image alone, and the specific constellation of symptoms in the image points more directly to a third nerve lesion rather than an inflammatory syndrome.
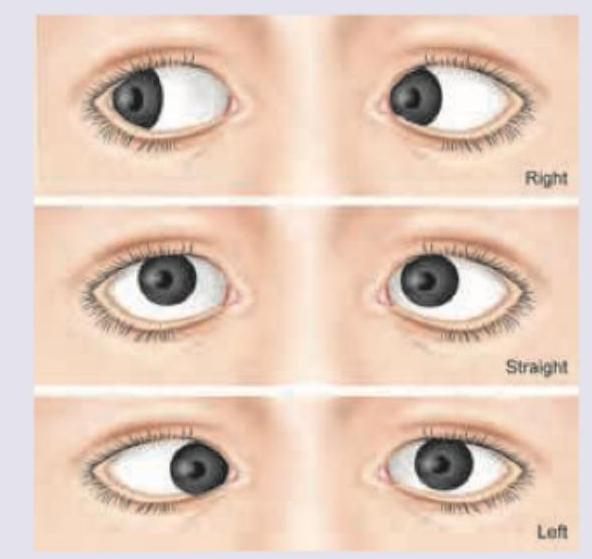
Question 6: A 60-year-old male underwent a cataract surgery. After 1 year he came with complaints of diminished vision and the finding shown in the image. Diagnosis is?
- A. 2nd nerve palsy
- B. 3rd nerve palsy
- C. 4th nerve palsy
- D. 6th nerve palsy (Correct Answer)
Explanation: ***6th nerve palsy*** - The image shows the **right eye** is unable to **abduct** (move outwards) when looking to the right, and is **adducted** (turned inwards) when looking straight ahead, which is characteristic of a **sixth cranial nerve (abducens) palsy**. - The abducens nerve innervates the **lateral rectus muscle**, which is responsible for abduction of the eye. Its paralysis causes the affected eye to deviate medially due to the unopposed action of the medial rectus muscle. *2nd nerve palsy* - **Second nerve (optic nerve) palsy** would primarily present with **vision loss** or field defects, not with abnormal eye movements. - The optic nerve transmits visual information from the eye to the brain and does not control ocular motility. *3rd nerve palsy* - **Third nerve (oculomotor) palsy** typically presents with **ptosis**, **dilated pupil**, and the eye positioned **down and out**. - This is because the oculomotor nerve innervates most extraocular muscles (medial, superior, inferior rectus, inferior oblique) and the levator palpebrae superioris, as well as pupillary constrictors. *4th nerve palsy* - **Fourth nerve (trochlear) palsy** affects the **superior oblique muscle**, leading to **vertical diplopia** and the eye being unable to move down and in. - Patients often compensate by **tilting their head** to the opposite shoulder.
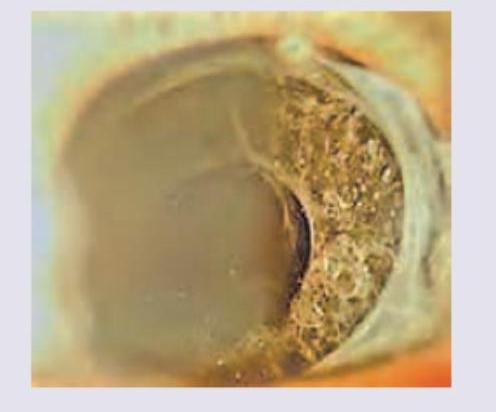
Question 7: A 60-year-old male underwent a cataract surgery. After 1 year he came with complaints of diminished vision and the finding shown in the image. Diagnosis is?
- A. Irvine-Gass syndrome
- B. After cataract (Correct Answer)
- C. UGH syndrome
- D. Endophthalmitis
Explanation: ***After cataract*** - The image depicts a **thickening and opacification of the posterior capsule** behind an intraocular lens, which is characteristic of after cataract (also known as **posterior capsular opacification** or PCO). - PCO is a common complication following cataract surgery, leading to **diminished vision** months to years after the initial procedure, consistent with the patient's presentation. *Irvine-Gass syndrome* - Irvine-Gass syndrome refers to **pseudophakic cystoid macular edema**, which causes diminished vision after cataract surgery due to fluid accumulation in the macula. - While it can cause vision loss post-cataract surgery, it is a retinal condition and does not present with the **posterior capsule opacification** seen in the image. *UGH syndrome* - UGH (Uveitis-Glaucoma-Hyphema) syndrome is a complication typically associated with poorly designed or positioned **intraocular lenses (IOLs)** that rub against uveal tissue. - It presents with **intraocular inflammation, elevated intraocular pressure, and recurrent hyphema**, none of which are directly suggested by the provided image or clinical details. *Endophthalmitis* - Endophthalmitis is a severe **intraocular infection** that typically occurs days to weeks after cataract surgery, presenting acutely with significant **pain, redness, and severe vision loss**. - The patient's presentation of diminished vision one year after surgery and the image showing a **fibrotic posterior capsule** are not consistent with the acute, infectious nature of endophthalmitis.