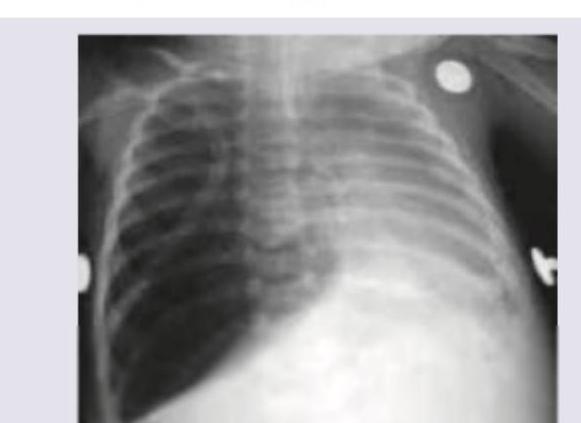
The image shows presence of:
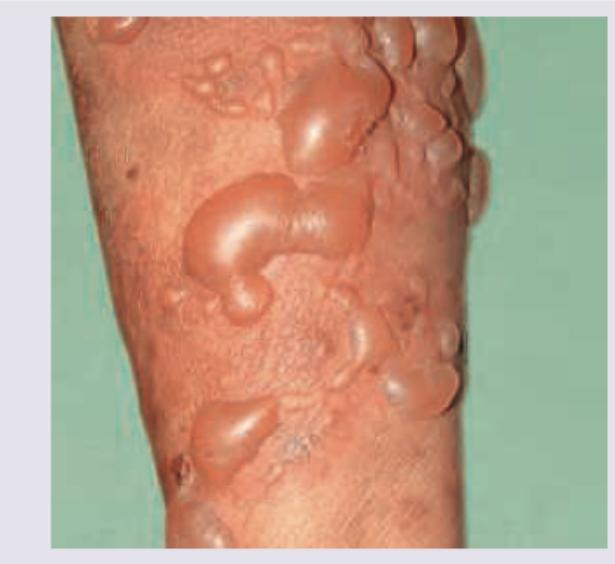
An elderly patient presents with itchy tense blisters on normal looking skin as well as on urticarial plaques as shown below. The most probable diagnosis is: (AIIMS Nov 2015)
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
The image shows presence of:

An elderly patient presents with itchy tense blisters on normal looking skin as well as on urticarial plaques as shown below. The most probable diagnosis is: (AIIMS Nov 2015)

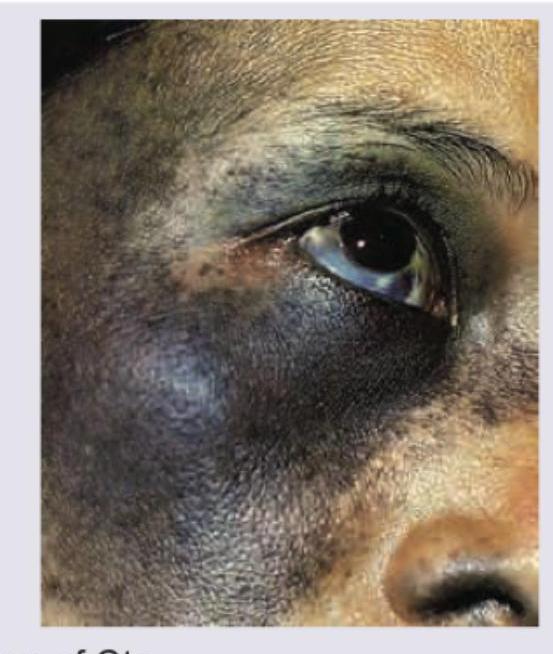
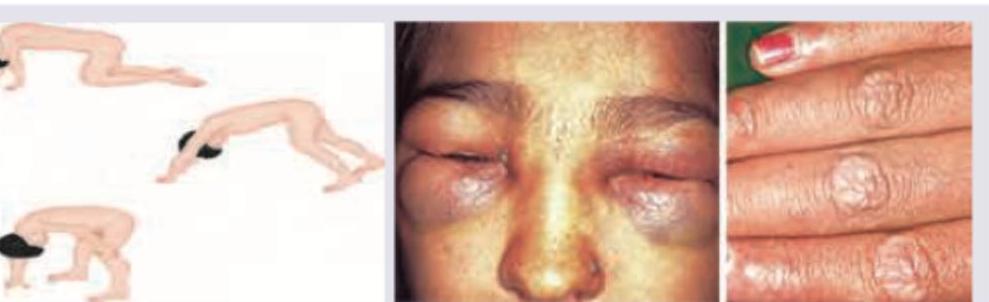
A 9-year-old girl presents with pigmentation over forehead and redness over upper eyelids. On physical examination following clinical sign was elicited. What is the next best step for diagnosis?
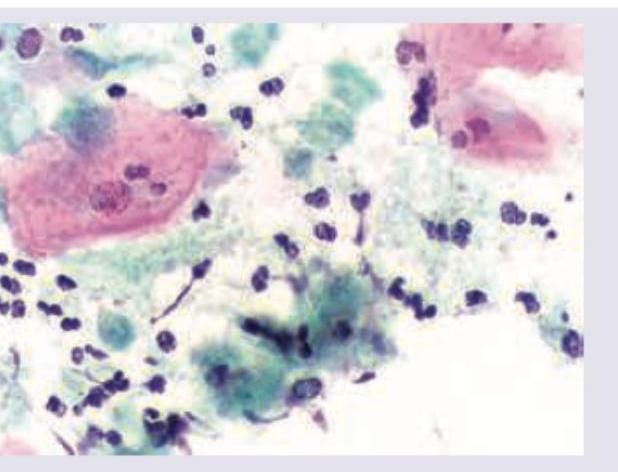
A wet mount preparation of vaginal discharge shows the following. Identify the organism responsible.
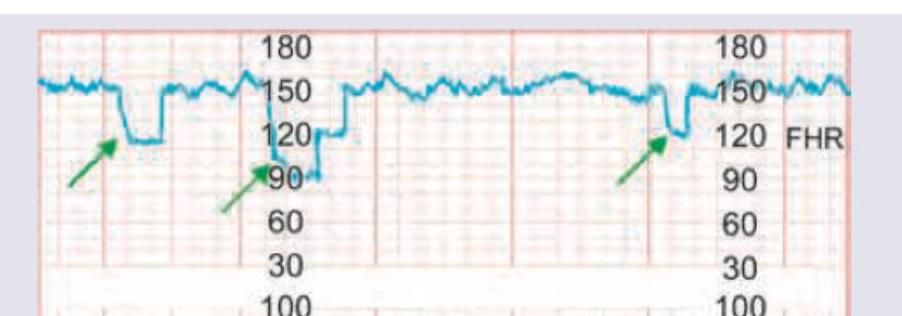
The following CTG indicates:
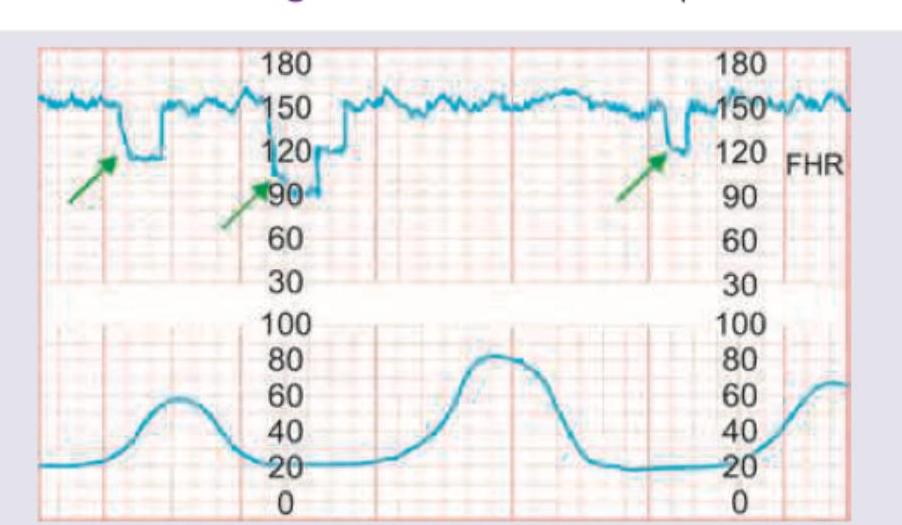
The following CTG indicates:
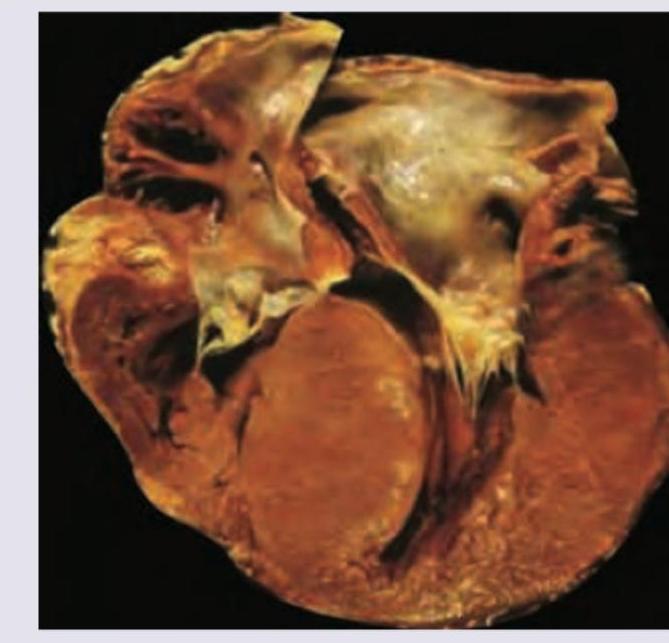
An athlete collapsed suddenly during exercise and died on the field. Postmortem heart is shown in the figure. There is family history of heart disease. What is the diagnosis?
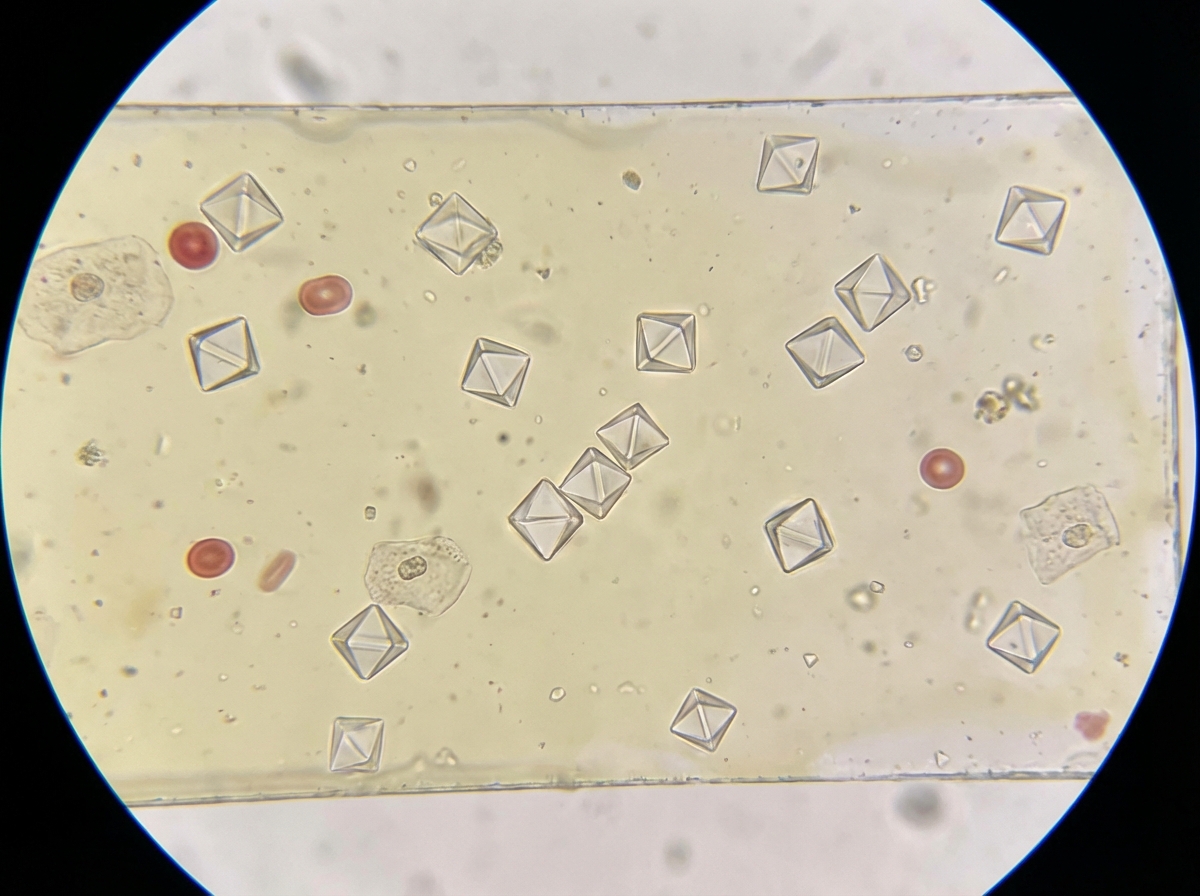
Which urine crystals are shown in the figure below?
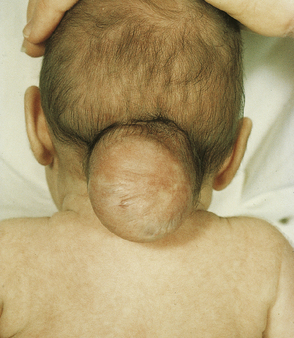
Identify the congenital defect seen in this baby.
A 4-year-old admitted in ward with pneumonia. He develops sudden onset of breathlessness. What is the next step in management?