INI-CET 2015 — Microbiology
5 Previous Year Questions with Answers & Explanations
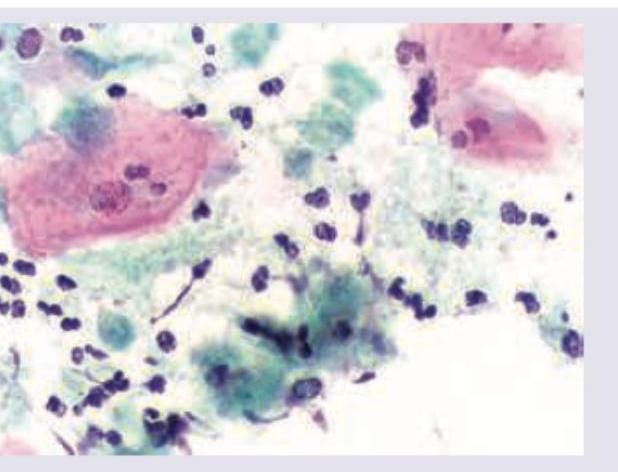
A wet mount preparation of vaginal discharge shows the following. Identify the organism responsible.
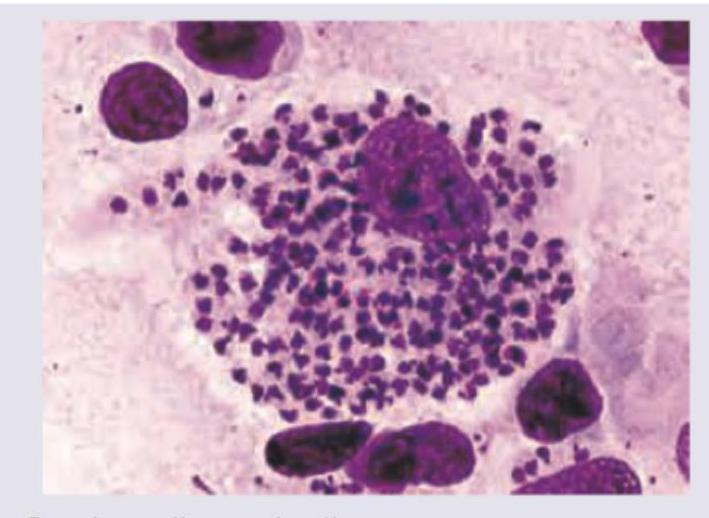
A 24-year-old female presented with an ulcer in the genital area. A giemsa stained cervical smear was prepared. Identify the causative agent: (AIIMS Nov 2015)
A 35-year-old male farmer presents with multiple discharging cervical sinuses. Which of these stains will be useful for the diagnosis and where does this organism normally colonize in the body? (AIIMS Nov 2015)
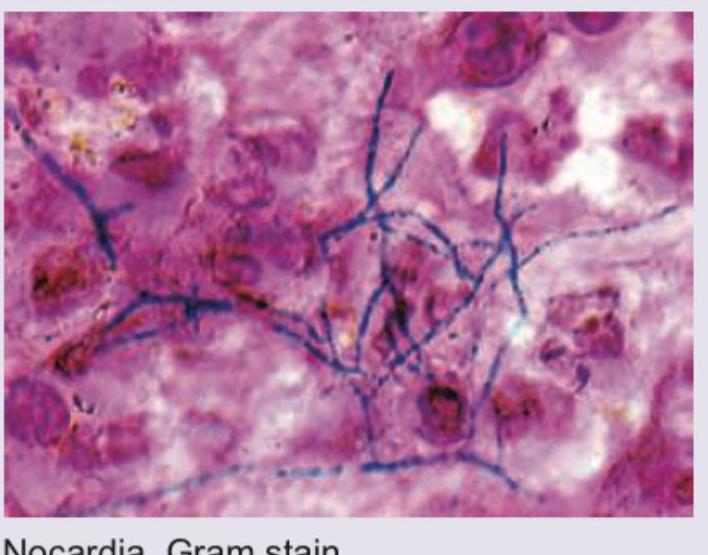
Stereotactic CT based aspiration from a patient with brain abscess was performed. Identify the organism seen and the stain used.
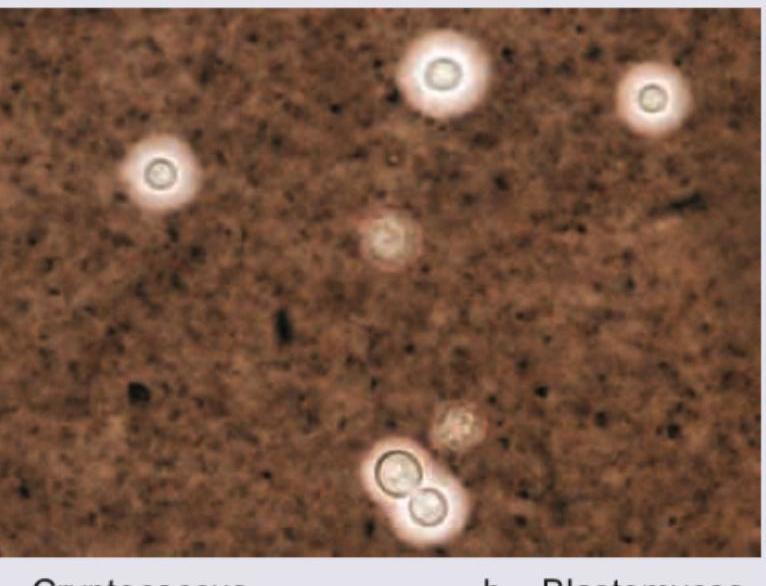
A patient presented with headache and projectile vomiting and altered sensorium. The following organism was demonstrated on India ink staining. What is the likely diagnosis?
INI-CET 2015 - Microbiology INI-CET Practice Questions and MCQs
Question 1: A wet mount preparation of vaginal discharge shows the following. Identify the organism responsible.
- A. Trichomonas vaginalis (Correct Answer)
- B. Neisseria gonorrhoeae
- C. Chlamydia
- D. Treponema pallidum
Explanation: ***Trichomonas vaginalis*** - The image shows numerous flagellated protozoa, characterized by their **pear-shaped appearance** with **jerky motility** on wet mount examination. - **Trichomonas vaginalis** is a flagellated protozoan parasite causing vaginitis, typically presenting with frothy, yellow-green vaginal discharge and strawberry cervix. - Wet mount microscopy showing motile trophozoites is the classic diagnostic method for trichomoniasis. *Neisseria gonorrhoeae* - This bacterium is a **gram-negative diplococcus**, typically seen intracellularly within neutrophils on Gram stain. - It does not present as flagellated protozoa on microscopy. *Chlamydia* - **Chlamydia trachomatis** is an obligate intracellular bacterium, not visible on routine wet mount microscopy. - Diagnosis requires specialized staining (Giemsa), immunofluorescence, or molecular tests (NAAT). *Treponema pallidum* - This is a **spirochete** responsible for syphilis, typically identified using dark-field microscopy from ulcer exudate or serological tests. - It does not present as the large, flagellated protozoa characteristic of Trichomonas.
Question 2: A 24-year-old female presented with an ulcer in the genital area. A giemsa stained cervical smear was prepared. Identify the causative agent: (AIIMS Nov 2015)
- A. Gardnerella vaginalis
- B. Chlamydia
- C. Calymmatobacterium granulomatosis
- D. Haemophilus ducreyi (Correct Answer)
Explanation: ***Hemophilus ducreyi*** - The image shows numerous small, pleomorphic, gram-negative coccobacilli arranged in **'school of fish'** or parallel chains, characteristic of **_Haemophilus ducreyi_** on a Giemsa-stained smear. - This morphology, especially from a genital ulcer, is highly indicative of **chancroid**, caused by _H. ducreyi_. *Gardnerella vaginalis* - _Gardnerella vaginalis_ is associated with **bacterial vaginosis** and is characterized by the presence of **"clue cells"** (vaginal epithelial cells covered with coccobacilli) on microscopy. - It does not form the "school of fish" arrangement seen in the image, nor does it typically cause ulcerative lesions. *Chlamydia* - **_Chlamydia trachomatis_** causes various infections, including genital ulcers in cases of **lymphogranuloma venereum (LGV)**, but it is an obligate intracellular bacterium. - It would appear as **intracellular inclusions** on a Giemsa stain and would not show extracellular coccobacillary forms arranged in clusters as depicted. *Calymmatobacterium granulomatosis* - Previously known as _Calymmatobacterium granulomatosis_, now designated as **_Klebsiella granulomatis_**, this bacterium causes **granuloma inguinale (donovanosis)**, characterized by large, beefy-red ulcers. - Diagnostic features on Giemsa stain include **Donovan bodies** (intracellular bacilli within macrophages), which are not a prominent feature in the provided image.
Question 3: A 35-year-old male farmer presents with multiple discharging cervical sinuses. Which of these stains will be useful for the diagnosis and where does this organism normally colonize in the body? (AIIMS Nov 2015)
- A. Gram stain, hypopharynx
- B. PAS, intestine
- C. Modified kinyoun acid fast stain, mouth (Correct Answer)
- D. Grocott methenamine silver stain, vagina
Explanation: ***Modified Kinyoun acid-fast stain, mouth*** - This clinical presentation of **multiple discharging cervical sinuses** in a farmer is highly suggestive of **actinomycosis**, caused by *Actinomyces israelii*. - *Actinomyces israelii* is a **Gram-positive, non-spore-forming, anaerobic to microaerophilic rod** that is **partially acid-fast (modified Kinyoun acid-fast stain)** and a normal inhabitant of the **oral cavity, gastrointestinal tract, and female genital tract**. *Gram stain, hypopharynx* - While *Actinomyces israelii* would stain Gram-positive, the **Gram stain** alone is not specific enough to confirm actinomycosis, especially given the characteristic partially acid-fast nature. - The **hypopharynx** is not the primary or most common normal colonization site for *Actinomyces israelii*; the mouth is more accurate. *PAS, intestine* - The **Periodic Acid-Schiff (PAS) stain** is typically used to identify fungi, carbohydrates, and glycogen, not primarily *Actinomyces*. - While *Actinomyces* can be found in the intestine, it's not the most common colonization site associated with cervicofacial actinomycosis. *Grocott methenamine silver stain, vagina* - **Grocott Methenamine Silver (GMS) stain** is primarily used for the detection of fungi and some encapsulated bacteria, but not specifically *Actinomyces*. - Though *Actinomyces* can colonize the vagina, it's more commonly associated with pelvic actinomycosis, not the cervical presentation described.
Question 4: Stereotactic CT based aspiration from a patient with brain abscess was performed. Identify the organism seen and the stain used.
- A. Nocardia, Gram stain (Correct Answer)
- B. Cryptococcus, India ink
- C. Streptococcus, Gram stain
- D. Staphylococcus, Gram stain
Explanation: ***Correct: Nocardia, Gram stain*** - The image displays **Gram-positive, branching filamentous bacteria**, which are characteristic morphological features of *Nocardia* species. These organisms are known to cause brain abscesses, especially in immunocompromised individuals. - The stain used is clearly a **Gram stain**, as evidenced by the purple/blue coloring of the bacterial cells (Gram-positive) against a pink/red background (counterstain). - *Nocardia* species are **weakly acid-fast** and show characteristic **branching, beaded filaments** that can be visualized with Gram staining. *Incorrect: Cryptococcus, India ink* - *Cryptococcus* is a **yeast** and would appear as round or oval budding cells, often with a prominent capsule, rather than branching filaments. - An **India ink stain** highlights the polysaccharide capsule of *Cryptococcus* as a clear halo against a black background, which is not what is seen in the image. *Incorrect: Streptococcus, Gram stain* - *Streptococcus* species are **Gram-positive cocci** that typically arrange in chains. They would appear as spherical cells in linear arrangements, not as filamentous structures. - While *Streptococcus* species can cause brain abscesses, their morphology in a Gram stain would be distinctly different from the branching filaments shown. *Incorrect: Staphylococcus, Gram stain* - *Staphylococcus* species are **Gram-positive cocci** that typically arrange in grape-like clusters. They would appear as spherical cells in irregular clumps, not as filamentous structures. - Similar to *Streptococcus*, their characteristic coccal morphology on a Gram stain would not match the filamentous structures observed in the image.
Question 5: A patient presented with headache and projectile vomiting and altered sensorium. The following organism was demonstrated on India ink staining. What is the likely diagnosis?
- A. Cryptococcus (Correct Answer)
- B. Blastomyces
- C. Histoplasma
- D. Coccidioides
Explanation: ***Cryptococcus*** - The image displays encapsulated yeast cells, characteristic of **_Cryptococcus neoformans_** or **_Cryptococcus gattii_**, which are commonly highlighted by **India ink staining** due to their large polysaccharide capsule. - The clinical presentation of headache, projectile vomiting, and altered sensorium strongly suggests **cryptococcal meningitis**, especially in immunocompromised individuals. *Blastomyces* - **_Blastomyces dermatitidis_** appears as large, broad-based budding yeast, which is distinct from the encapsulated yeasts seen in the image. - While it can cause CNS infection, its morphological characteristics under microscopy are different, and India ink is not its primary diagnostic stain. *Histoplasma* - **_Histoplasma capsulatum_** is a small, intracellular yeast, often seen within macrophages, and does not possess a prominent capsule that would be stained by India ink. - Neurological involvement is less common than with _Cryptococcus_ and the microscopic appearance is different. *Coccidioides* - **_Coccidioides immitis_** forms **spherules** containing **endospores** in tissue samples, a distinct morphology not seen in the provided image. - Although it can cause meningitis, its microscopic identification relies on finding these spherules, not encapsulated yeasts with India ink.