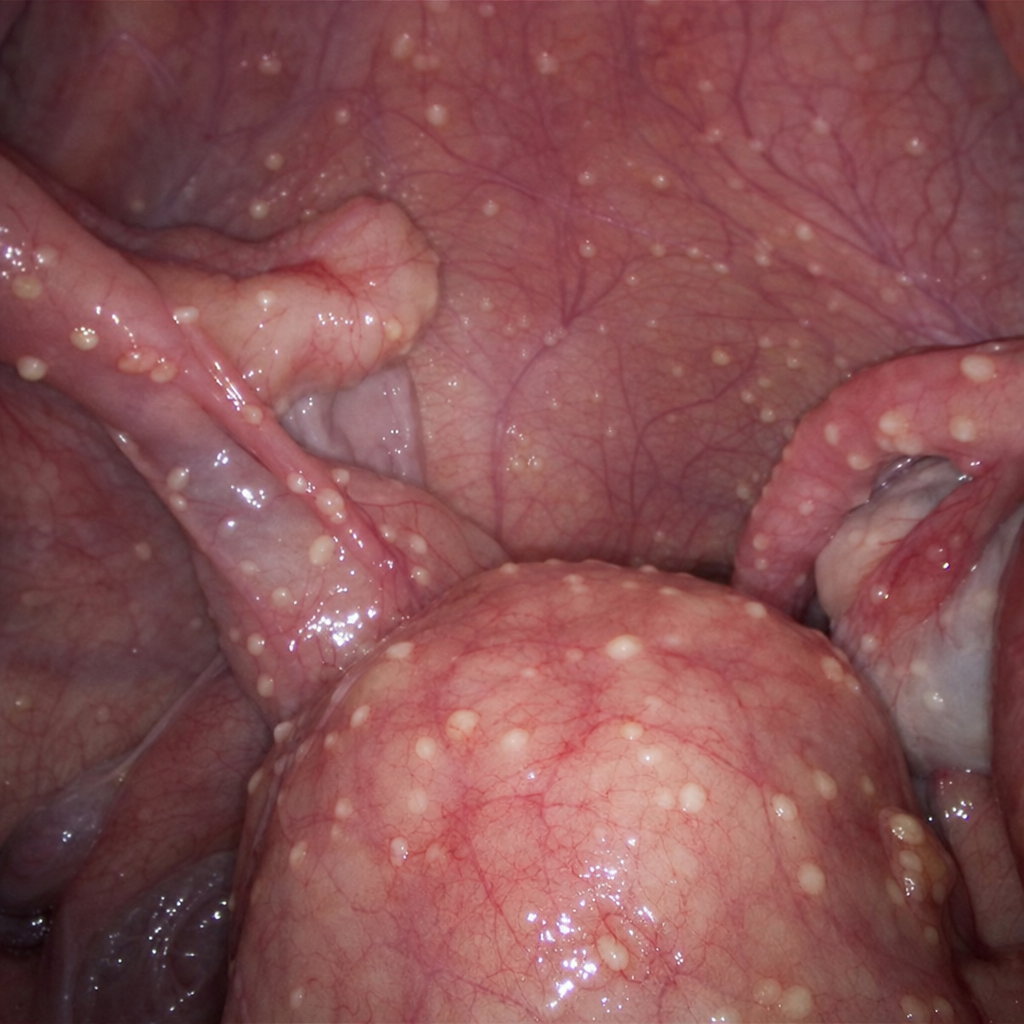
What is the likely diagnosis for the given image?
During laparoscopy, multiple small, yellowish-white tubercles are observed scattered over the pelvic peritoneum and adnexal surfaces. What is the most likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which of the following is the schedule of the OPV vaccine?
An image of the mascot is shown below. Identify the related national health programme.
A patient presents with a transverse fracture at the skull base, described as splitting it and creating a 'hinge' with a 'nodding face sign.' This fracture extends from one petrous ridge across the sella turcica to the other petrous ridge. Which type of fracture is this?
Which of the following is the culture medium used for tuberculosis?
What is the most common causative organism of prosthetic heart valve endocarditis?
What is the likely diagnosis for the given image?
During laparoscopy, multiple small, yellowish-white tubercles are observed scattered over the pelvic peritoneum and adnexal surfaces. What is the most likely diagnosis?

A 23 year old male epileptic patient presented with pain in right shoulder region. Examination revealed that right upper limb was abducted and externally rotated and the movements could not be performed. Which of the following is the most likely diagnosis?
A child diagnosed with von Willebrand disease requires an understanding of the role of von Willebrand factor (vWF). What does von Willebrand factor primarily combine with?
A fracture caused by falls landing on feet/buttocks (force transmitted through the spine), heavy blows to the top of the skull/vertex, twisting of the head on the spine, or blows to the occiput or chin. Which type of fracture is this?