All (272)Anatomy (12)Anesthesiology (7)Biochemistry (17)Community Medicine (19)Dental (2)Dermatology (2)ENT (7)Forensic Medicine (9)Internal Medicine (35)Microbiology (23)Obstetrics and Gynecology (28)Ophthalmology (13)Orthopaedics (6)Pathology (12)Pediatrics (9)Pharmacology (26)Physiology (11)Psychiatry (7)Radiology (7)Surgery (20)
Q241
In this normal menstrual cycle graph, the mark 'X' represents levels of which hormone?
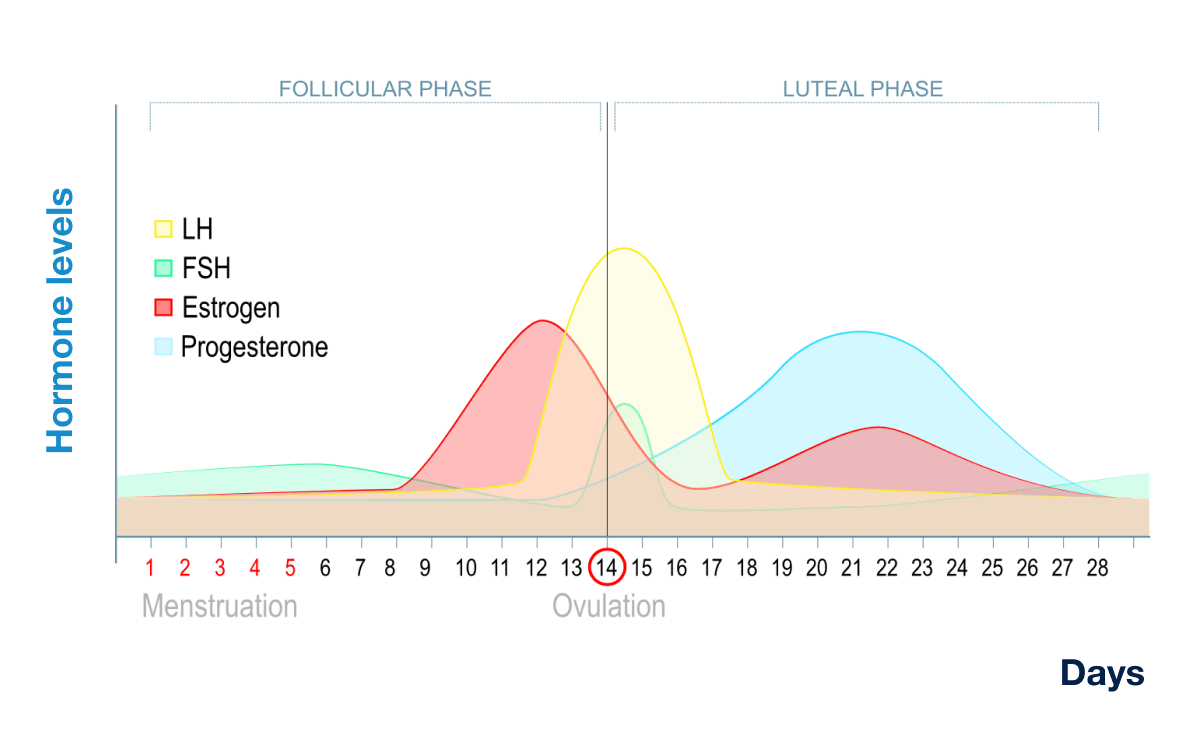
Q242
Normal anion gap is___ mmol/L?
