Burn Classification - Degrees of Damage
| Degree | Layers Involved | Appearance | Sensation | Healing |
|---|---|---|---|---|
| 1st | Epidermis | Red, dry, blanches | Painful | 3-6 days |
| 2nd (Partial) | Epidermis + Dermis | Blisters, moist, red/pink, blanches | Very painful | 7-21 days |
| 3rd (Full) | Through Dermis | Waxy, white, leathery, charred | Painless | Months, requires graft |
| 4th | Into fat, muscle, bone | Black, charred, dry | Painless | Requires excision |
TBSA Estimation - The Rule of Nines
A rapid method for estimating Total Body Surface Area (TBSA) for 2nd & 3rd-degree burns in adults. Not used for 1st-degree burns (e.g., sunburn).
- Head & Neck: 9%
- Anterior Torso: 18%
- Posterior Torso: 18%
- Each Arm: 9%
- Each Leg: 18%
- Genitalia/Perineum: 1%
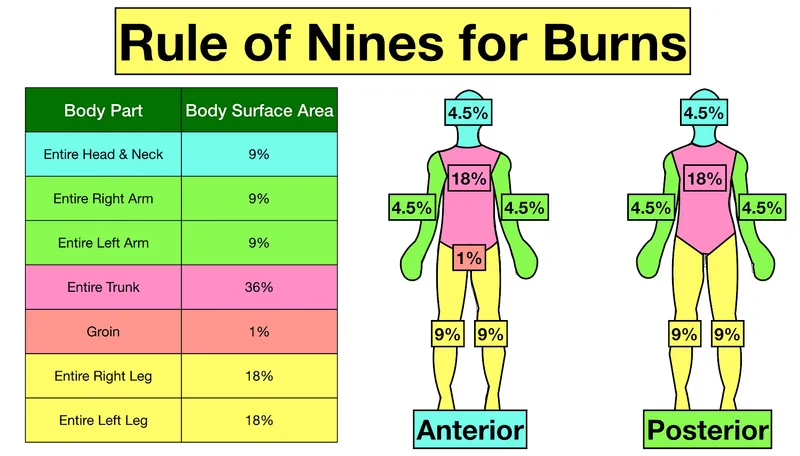
⭐ The TBSA estimate is a critical variable used in the Parkland formula to calculate IV fluid resuscitation volume for the first 24 hours.
For children, the Lund-Browder chart is more accurate due to different body proportions.
Fluid Resuscitation - The Parkland Plan
- Purpose: Guides IV fluid resuscitation for 2nd/3rd-degree burns, typically for TBSA >20%.
- Formula: Total fluid in 24h = $4 \text{ mL LR} \times % \text{TBSA} \times \text{Body Wt (kg)}$
- Administration Schedule:
- First 8 hours: Infuse 1/2 of the total calculated volume.
- Next 16 hours: Infuse the remaining 1/2 of the volume.
- Fluid of Choice: Lactated Ringer's (LR) is preferred over normal saline to prevent hyperchloremic metabolic acidosis.
⭐ The "first 8 hours" starts from the time of the burn injury, not from the time of hospital arrival.
Complications & Special Burns - Beyond the Basics
-
Systemic Complications:
- Infection: Pseudomonas (most common), S. aureus. High risk of sepsis.
- Metabolic: Hypermetabolic state (↑cortisol, ↑catecholamines) leading to hyperglycemia & muscle wasting.
- GI: Curling's ulcer (stress-related gastric ulcer).
- MSK: Joint contractures, heterotopic ossification.
-
Special Burn Types:
- Electrical: Deep tissue injury often hidden. Risk of rhabdomyolysis (check CK), arrhythmias (monitor ECG for 24h), and posterior shoulder dislocation.
- Chemical: Irrigate copiously. Alkali is worse (liquefaction necrosis) than acid. Brush off dry powders first.
- Inhalation: Suspect with facial burns/singed nares. Treat with 100% O₂; early intubation is key. Diagnose with bronchoscopy.
⭐ Marjolin's Ulcer: An aggressive squamous cell carcinoma that arises in chronic wounds or old burn scars, often years later.
High‑Yield Points - ⚡ Biggest Takeaways
- The Parkland formula (4 mL/kg/%TBSA) is paramount for guiding IV fluid resuscitation over the first 24 hours.
- Suspect inhalation injury with facial burns, soot, or hoarseness; prioritize early intubation to secure the airway.
- Circumferential burns of limbs or the chest may require urgent escharotomy to prevent compartment syndrome.
- Use the Rule of Nines for rapid estimation of Total Body Surface Area (TBSA) in adults.
- Prevent infection, especially from Pseudomonas, with topical antibiotics.
- Burns induce a hypermetabolic state, necessitating aggressive nutritional support.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

