Overview & Classification - The 'Whoops' Factor
Iatrogenic: "Brought forth by the healer." Unintended harm resulting directly from medical or surgical intervention, not the underlying disease.
- Classification Methods:
- By System: Vascular, nerve, visceral (e.g., ureter in pelvic surgery).
- By Error Type: Technical (skill-based), judgmental (decision-making), system failure.
- By Severity (Clavien-Dindo): Grades I-V based on the therapy required to manage the complication.
⭐ While surgical 'slips' are classic, the most common iatrogenic injury across all of medicine is an adverse drug event (ADE).

Common Nerve Injuries - Shocking Mistakes
| Nerve | Procedure at Risk | Clinical Manifestation |
|---|---|---|
| Axillary (C5-C6) | Deltoid IM injection, humerus fracture repair | Deltoid paralysis (impaired abduction), loss of sensation over lateral shoulder. |
| Long Thoracic | Mastectomy, axillary node dissection | "Winging" of the scapula due to serratus anterior paralysis. |
| Recurrent Laryngeal | Thyroidectomy, parathyroidectomy | Hoarseness (unilateral); airway obstruction if bilateral injury occurs. |
| Spinal Accessory (CN XI) | Posterior triangle lymph node biopsy | Drooping shoulder, impaired arm abduction >90°, weakened shoulder shrug. |
| Common Peroneal | Fibular neck fracture, tight leg cast | Foot drop (loss of dorsiflexion & eversion), "steppage gait." |
📌 Mnemonic: Long Thoracic Nerve innervates Serratus Anterior. LTSA = "Let's Try Saving the Angel's wing".
Visceral & Vascular Injuries - Plumbing & Punctures
- Bowel Injury: Most common in laparoscopy. Suspect with post-op fever, peritonitis, or free air on CT. Delayed diagnosis ↑ mortality.
- Ureteral Injury: High risk in pelvic surgery (e.g., hysterectomy). Often presents late with flank pain, fever, or urinoma.
- 📌 Mnemonic: "Water under the bridge" - Uterine artery crosses over the ureter.
- Bladder Injury: Common in pelvic procedures. Suspect with gross hematuria or oliguria post-op. Diagnose with retrograde cystogram.
- Bile Duct Injury: Classic cholecystectomy complication. Leads to bile leak or stricture. ERCP/MRCP is diagnostic & therapeutic.
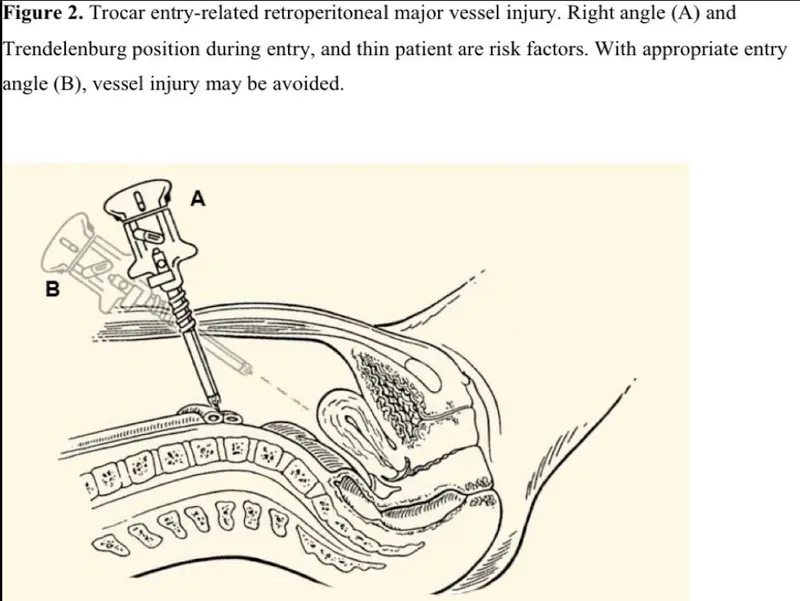
- Vascular Injury: Major vessels (aorta, IVC) at risk from deep dissection or laparoscopic entry. Can cause massive hemorrhage & shock.
⭐ During laparoscopic cholecystectomy, iatrogenic bile duct injury is a major risk. Prevention relies on achieving the "critical view of safety" before clipping or cutting any structures.
Prevention & Mitigation - The Safety Net
Proactive, systems-based strategies are key. Utilizes checklists, clear communication, and standardized protocols to create a safety net, minimizing human error. Key pillars include:
- Communication: Structured, closed-loop (e.g., SBAR).
- Team Training: Crew Resource Management (CRM).
- Standardization: Reduces ambiguity and reliance on memory.
⭐ The WHO Surgical Safety Checklist is a cornerstone of patient safety, demonstrated to significantly reduce both morbidity and mortality rates across diverse surgical settings.
High‑Yield Points - ⚡ Biggest Takeaways
- Common bile duct injury is a feared complication of laparoscopic cholecystectomy.
- Ureters are most vulnerable during hysterectomy and colorectal surgery.
- Recurrent laryngeal nerve injury during thyroidectomy causes hoarseness or airway obstruction.
- Axillary nerve injury during shoulder surgery leads to deltoid weakness and sensory loss.
- The spleen is the most commonly injured organ during other major abdominal operations.
- Bowel perforation is a key risk in laparoscopy and endoscopy, causing peritonitis.
- Suspect iatrogenic injury with any unexplained postoperative pain, fever, or organ dysfunction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

