🦠 Pathophysiology - Infection's Upward Spiral
- Initiating Event: Ascending infection from the cervix/vagina, typically post-menses when the cervical mucus barrier is thin.
- Primary Pathogens: Neisseria gonorrhoeae & Chlamydia trachomatis disrupt the endocervical barrier, facilitating the ascent of polymicrobial vaginal flora.
- Inflammatory Cascade: Leads to mucosal damage, edema, and destruction of ciliated epithelial cells in the fallopian tubes, impairing ovum transport.
⭐ Fitz-Hugh-Curtis Syndrome: Perihepatic inflammation causing "violin-string" adhesions between the liver capsule and peritoneum. Presents with RUQ pain, often pleuritic, with normal LFTs.
⛓️ Complications - PID's Lasting Legacy
PID's inflammatory cascade leads to significant long-term sequelae, primarily from scarring and adhesions in the upper genital tract.
- Infertility: Tubal scarring, hydrosalpinx, and occlusion. Risk increases with each episode.
- Ectopic Pregnancy: Risk increases 6-10x due to damaged ciliary function and tubal obstruction.
- Chronic Pelvic Pain: Common sequela (>18% of cases) from pelvic adhesions.
- Tubo-ovarian Abscess (TOA): Acute, severe complication. Complex adnexal mass with fever/leukocytosis. Requires drainage & broad-spectrum IV antibiotics.
- Fitz-Hugh-Curtis Syndrome: Perihepatitis. "Violin-string" adhesions between liver capsule and peritoneum. Presents with RUQ pain.
⭐ The risk of infertility is ~15% after one episode of PID, ~35% after two, and ~75% after three or more episodes.

🔬 Diagnosis - Unmasking the Damage
- Primary Imaging Modality: Transvaginal Ultrasound (TVUS) is the first-line test for suspected PID complications.
- Specific Complication Findings:
- Tubo-ovarian Abscess (TOA):
- TVUS: Complex, multiloculated adnexal mass with thick walls; tube and ovary are indistinguishable.
- CT: Used for suspected rupture or to rule out GI pathology.
- Pyosalpinx/Hydrosalpinx:
- TVUS: Dilated, sausage-shaped, fluid-filled fallopian tube.
- 💡 "Cogwheel sign" indicates thickened endosalpingeal folds in pyosalpinx.
- Fitz-Hugh-Curtis Syndrome:
- Laparoscopy (gold standard): "Violin-string" adhesions between the liver capsule and peritoneum.
- Tubo-ovarian Abscess (TOA):

⭐ Laparoscopy is the ultimate gold standard for diagnosing PID complications, allowing direct visualization and simultaneous therapeutic intervention (e.g., abscess drainage, adhesiolysis).
🧹 Management - The Aftermath Cleanup
- Tubo-ovarian Abscess (TOA):
- Initial: Hospitalization + IV broad-spectrum antibiotics (e.g., Cefotetan/Cefoxitin + Doxycycline; or Clindamycin + Gentamicin).
- Failure to improve in 48-72 hrs or abscess >7-9 cm warrants drainage.
- Drainage options: Percutaneous (IR-guided) or surgical (laparoscopy).
- Fitz-Hugh-Curtis Syndrome (Perihepatitis):
- Inflammation of liver capsule → "violin-string" adhesions.
- Treat underlying PID. Laparoscopic lysis of adhesions for persistent pain.
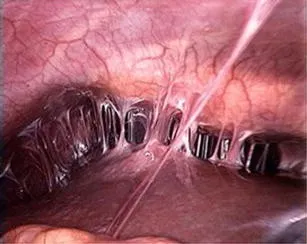
⭐ Fitz-Hugh-Curtis syndrome can present with acute RUQ pain, mimicking cholecystitis, but typically with normal LFTs and gallbladder ultrasound.
- Chronic Sequelae:
- ↑ Risk of infertility (tubal factor), ectopic pregnancy, and chronic pelvic pain.
⚡ Biggest Takeaways
- Tubo-ovarian abscess (TOA) is a severe complication presenting as a complex adnexal mass; requires IV antibiotics and possible drainage.
- Infertility and increased risk of ectopic pregnancy are major long-term sequelae from tubal scarring and adhesions.
- Fitz-Hugh-Curtis syndrome (perihepatitis) causes RUQ pain from "violin-string" adhesions on the liver capsule.
- Chronic pelvic pain is a common, debilitating outcome resulting from pelvic adhesions.
- Hydrosalpinx (fluid-filled, blocked fallopian tube) is another significant cause of infertility.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

