🧬 Pathophysiology - The Wall Weakens
The aortic wall weakens from degradation of structural proteins (elastin, collagen), leading to dilation. Governed by Laplace's Law, wall tension increases with radius ($T = P \times r$), promoting further expansion.
- Degenerative (Most Common):
- Atherosclerosis: Chronic inflammation damages intima and media.
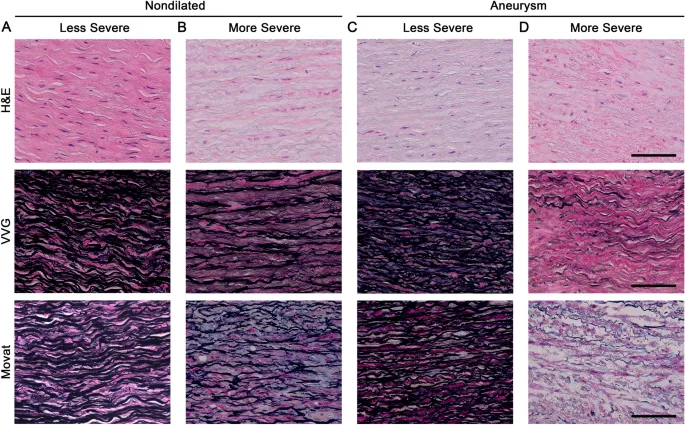
- Cystic Medial Necrosis: Fragmentation of elastic fibers in the media; common with aging.
- Genetic/Connective Tissue Disorders:
- Marfan Syndrome: Defective fibrillin-1 (FBN1).
- Ehlers-Danlos Syndrome (Vascular): Defective type III collagen.
- Other:
- Infections: Syphilitic aortitis, mycotic aneurysms (Staph, Salmonella).
- Trauma: Deceleration injury.
⭐ Marfan syndrome is classically associated with cystic medial necrosis, predisposing to aortic root aneurysm and dissection.
🤫 Clinical Manifestations - The Silent Threat
Most are asymptomatic and discovered incidentally. When symptoms occur, they are due to expansion, compression, or rupture.
- Pain: Most common symptom. Typically a deep, steady, severe pain in the chest or back.
- Compression of adjacent structures:
- Hoarseness: Left recurrent laryngeal nerve palsy.
- Dysphagia: Esophageal compression.
- Stridor/Cough: Tracheal or mainstem bronchus compression.
- SVC Syndrome: Edema of the face/neck/arms, JVD.
⭐ Hoarseness from a TAA is a classic sign of left recurrent laryngeal nerve compression (Ortner's syndrome), a frequently tested association.
🩺 Diagnosis - Seeing the Bulge
- Initial Test: Chest X-ray (CXR) is often the first clue, showing a widened mediastinum or an enlarged aortic knob.
- Gold Standard: CT Angiography (CTA) is the definitive diagnostic tool.
- Details aneurysm size, location, and branch vessel involvement.
- Essential for pre-operative planning (Open vs. TEVAR).
- Alternatives:
- MRA: For stable patients with contraindications to CTA (e.g., severe contrast allergy, renal failure).
- TEE: Useful for unstable patients or intra-operative assessment.
⭐ CTA is not just for diagnosis; it's the essential roadmap for planning repair, determining suitability for endovascular (TEVAR) vs. open surgery.
🔪 Management - Cut or Watch?
- Medical Management (Watch): Goal is to ↓ aortic wall stress & slow expansion.
- BP Control: Target SBP 100-120 mmHg.
- Agents: β-blockers (first-line); ARBs (especially for Marfan syndrome).
- Surveillance: Serial imaging (CT/MRI) every 6-12 months.
⭐ Beta-blockers are key as they decrease the rate of change of blood pressure ($dP/dt$), reducing aortic shear stress beyond just lowering the absolute BP.
- Surgical Intervention (Cut): Decision based on size, growth rate, or symptoms.
💥 Complications - When the Wall Breaks
- Rupture: Catastrophic hemorrhage (hemothorax, hemopericardium).
- Presents with sudden pain, profound hypotension, and shock.
- Dissection: Intimal tear creates a false lumen.
- Presents with new, severe, "tearing" chest or back pain.
- Leads to malperfusion syndromes (stroke, MI, limb ischemia).
⭐ Rupture is a surgical catastrophe with pre-hospital mortality >80%. Immediate intervention is the only chance for survival.
⚡ Biggest Takeaways
- Ascending TAA is linked to Marfan syndrome and cystic medial necrosis; descending TAA to atherosclerosis.
- Often asymptomatic; symptoms from compression (hoarseness, dysphagia) or chest/back pain.
- CT angiography (CTA) is the diagnostic gold standard for planning repair.
- Repair ascending TAA at >5.5 cm (or >4.5 cm in Marfan).
- Repair descending TAA at >6.0 cm, often with endovascular repair (TEVAR).
- Medical therapy: strict blood pressure control with beta-blockers to slow growth.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

