🌪️ Core concept - Twist and Shout
- Urologic Emergency: Twisting of the spermatic cord obstructs testicular blood flow, leading to ischemia and infarction.
- Diagnosis: Primarily clinical (sudden severe pain, high-riding testis, absent cremasteric reflex).
- Imaging: STAT color Doppler ultrasound confirms ↓ or absent blood flow.
⭐ "Time is testis": Salvage rate is >90% if detorsion occurs within 6 hours of symptom onset.
- Management: Immediate surgical exploration, detorsion, and bilateral orchiopexy.
- 💡 Manual detorsion ("open the book" motion) can be attempted as a temporizing measure.
🏃♂️ The Sudden Scrotal Saga
- Onset: Acute, severe, unilateral testicular pain, often with nausea & vomiting.
- Patient: Typically adolescents; may awaken patient from sleep.
- Physical Exam:
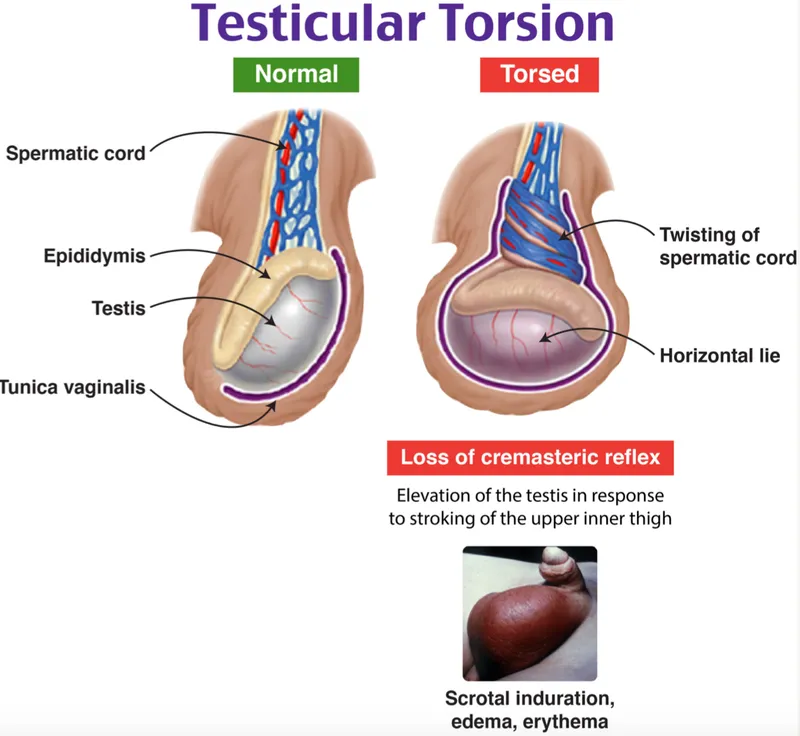
- Swollen, erythematous, and exquisitely tender hemiscrotum.
- High-riding testis with a horizontal lie.
- ⚠️ Absent cremasteric reflex on the affected side.
- Negative Prehn's sign (scrotal elevation does NOT relieve pain).
⭐ The underlying "bell clapper" deformity allows the testis to rotate freely on the spermatic cord, as the tunica vaginalis attaches abnormally high.
⏱️ Diagnosis - Racing the Clock
- Diagnosis is clinical and extremely time-sensitive.
- Physical Exam:
- Absent cremasteric reflex (highly sensitive).
- High-riding, transversely oriented testis.
- Negative Prehn's sign (no pain relief with scrotal elevation).
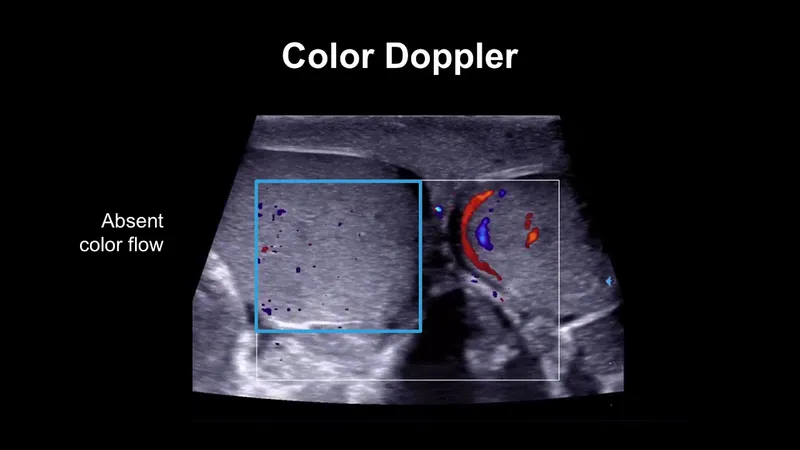
- Imaging: STAT Color Doppler Ultrasound is the test of choice.
- Key Finding: Absent or significantly ↓ arterial flow.
- Helps differentiate from epididymitis (hyperemia/↑ flow).
- Urinalysis is usually normal.
⭐ A high index of suspicion warrants immediate urologic consultation and potential surgical exploration, even before imaging. Do not delay surgery for ultrasound if the diagnosis is clear.
⚕️ Management - The Untangling Act
This is a true urological emergency. Time is testis.
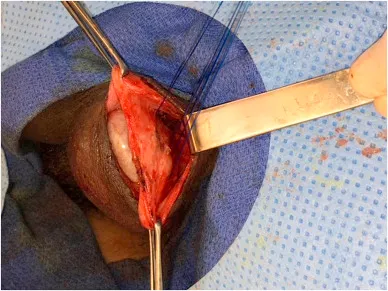
- Immediate surgical consultation is mandatory.
- ⚠️ Salvage Rates: >90% if corrected <6 hours; <10% after 24 hours.
- Manual Detorsion:
- Temporary measure while awaiting OR.
- 📌 Mnemonic: "Open the book" → rotate testis outwards (medial to lateral).
⭐ Bilateral Orchiopexy: The contralateral (unaffected) testis must also be fixed. The underlying anatomical cause (bell-clapper deformity) is frequently bilateral, and fixation prevents future torsion on the other side.
📉 Complications - Aftermath & Outlook
- Testicular Infarction/Necrosis: Primary risk with delayed reperfusion (>6 hrs).
- Requires orchiectomy (surgical removal of non-viable testis).
- Subfertility/Infertility:
- Due to loss of testicular mass.
- Potential for anti-sperm antibodies post-torsion.
- Testicular Atrophy: Affected testis may shrink even if salvaged.
- Contralateral Orchiopexy: Standard procedure to fix the unaffected testis, preventing future torsion.
⭐ Salvage rates are highly time-dependent: ~90% if surgery is within 6 hours, but drops to <10% after 24 hours.
⚡ Biggest Takeaways
- Testicular torsion is a urologic emergency requiring immediate intervention to preserve testicular viability.
- Suspect in any male with sudden, severe testicular pain, often with nausea and vomiting.
- Key exam findings: high-riding testis, horizontal lie, and an absent cremasteric reflex.
- Color Doppler ultrasound is the diagnostic test of choice, showing absent or decreased blood flow.
- Immediate surgical exploration is the definitive management.
- Testicular salvage rates drop sharply after 6 hours of ischemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

