🗺️ Anatomy - The Surgical Landscape
- Zonal Anatomy:
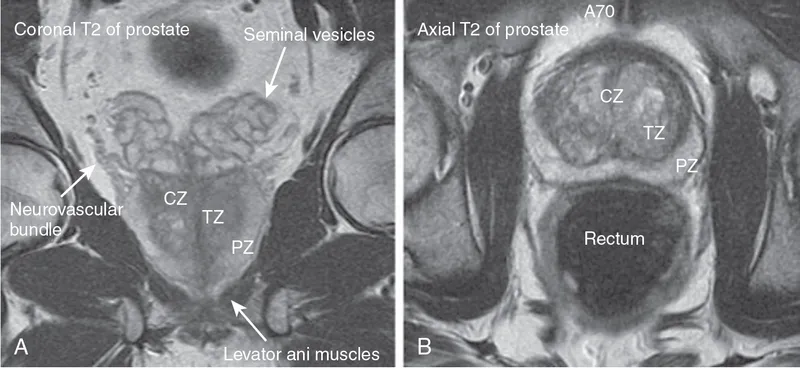
- Peripheral Zone (PZ): ~70% of gland; site of most prostate cancers. Palpable on Digital Rectal Exam (DRE).
- Transitional Zone (TZ): ~5% of gland; surrounds the urethra. Origin of Benign Prostatic Hyperplasia (BPH).
- Central Zone (CZ): ~25%; surrounds the ejaculatory ducts.
- Neurovascular Bundles (NVB):
- Run posterolaterally to the prostate.
- Contain cavernous nerves (from pelvic plexus) crucial for erectile function.
- Critical Relations:
- Posterior: Denonvilliers' fascia separates prostate from the rectum.
- Apex: Near external urethral sphincter (key for continence).
⭐ Injury to the cavernous nerves within the posterolateral neurovascular bundles during radical prostatectomy is the primary cause of post-operative erectile dysfunction.
🔪 Management - The Surgeon's Toolkit
-
Transurethral Resection of the Prostate (TURP):
- Indication: Gold standard for moderate-to-severe BPH.
- Procedure: Resects tissue from the transitional zone.
- ⚠️ Complications: Retrograde ejaculation (most common), TURP syndrome.
-
Laser Enucleation (HoLEP/ThuLEP):
- Indication: BPH, especially large glands (>80g).
- Advantage: ↓ bleeding risk vs. TURP.
-
Radical Prostatectomy (RP):
- Indication: Curative intent for localized prostate cancer.
- ⚠️ Complications: Erectile dysfunction (cavernous nerve injury), urinary incontinence (sphincter damage).
⭐ TURP Syndrome: Life-threatening dilutional hyponatremia from absorption of hypotonic irrigation fluid (glycine, sorbitol). Presents with nausea, confusion, hypertension, bradycardia, and visual changes.
⚠️ Complications - Navigating the Risks
-
Immediate:
- Bleeding: Most common early issue; monitor for clot retention.
- TURP Syndrome: Hyponatremia from absorption of hypotonic irrigation fluid (glycine, sorbitol). Presents with confusion, nausea, HTN, bradycardia.
- Infection: UTI, prostatitis.
-
Long-Term:
- Erectile Dysfunction (ED): Damage to cavernous nerves in posterolateral neurovascular bundles. Nerve-sparing techniques are key.
- Urinary Incontinence: Stress incontinence from external urethral sphincter injury.
- Retrograde Ejaculation: Common after TURP; semen enters the bladder.
- Bladder Neck Contracture / Urethral Stricture: Late fibrotic scarring causing obstruction.
⭐ TURP Syndrome is a medical emergency. The combination of hyponatremia, fluid overload, and potential glycine toxicity can lead to seizures and coma.
📋 Clinical - Post-Op Playbook
- Catheter & Irrigation:
- Indwelling Foley catheter is standard post-op.
- Continuous Bladder Irrigation (CBI) post-TURP prevents clot retention. Titrate to keep urine pink.
- Medications:
- Analgesics for pain.
- Anticholinergics (e.g., oxybutynin) for bladder spasms.
- Stool softeners (e.g., docusate) to prevent straining.
- Activity & Monitoring:
- Avoid heavy lifting (>10 lbs) for 4-6 weeks.
- ⚠️ Expect initial hematuria; report bright red blood or large clots.
- Follow-up for catheter removal, pathology review, and PSA monitoring.
⭐ Retrograde ejaculation is the most common long-term complication following TURP.
⚡ High-Yield Points - Biggest Takeaways
- Transurethral Resection of the Prostate (TURP) for BPH risks TURP syndrome (hyponatremia, fluid overload) and retrograde ejaculation.
- Radical Prostatectomy for localized cancer risks erectile dysfunction (cavernous nerve injury) and stress urinary incontinence.
- Nerve-sparing techniques during prostatectomy are critical for preserving post-operative erectile function.
- Post-prostatectomy PSA should become undetectable; a rising PSA signals biochemical recurrence.
- Stress incontinence after surgery is often due to internal urethral sphincter damage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

