Initial Assessment - Gut Check Time
The primary survey (ABCDEs) is the mandatory first step. Before any imaging, the clinician must determine if immediate surgical intervention is required based on "hard signs." This assessment is a rapid, hands-on evaluation to catch critical injuries that cannot wait.
- A: Airway, B: Breathing, C: Circulation: Is the patient hemodynamically stable? A systolic blood pressure of < 90 mmHg is a critical threshold indicating severe hemorrhage and the need for immediate action.
- D: Disability & E: Exposure: A full-body examination is crucial. Look for signs of peritonitis (involuntary guarding, rebound tenderness) or evisceration, which are absolute indications for surgery.
⭐ Peritonitis in a patient with blunt abdominal trauma is a hard sign that mandates immediate exploratory laparotomy.
Diagnostic Workup - Picture This Trauma
- FAST Exam (Focused Assessment with Sonography for Trauma): Initial test for unstable patients to rapidly detect hemoperitoneum (free fluid).
- Indications: Blunt or penetrating abdominal trauma, hypotension.
- 📌 Views: 'RUQ (Morison's pouch), LUQ (splenorenal), Pelvic (pouch of Douglas), Subxiphoid (pericardial)'.
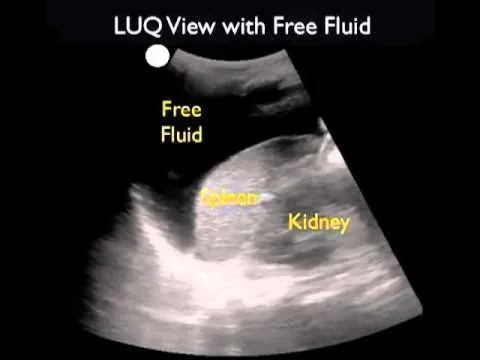
-
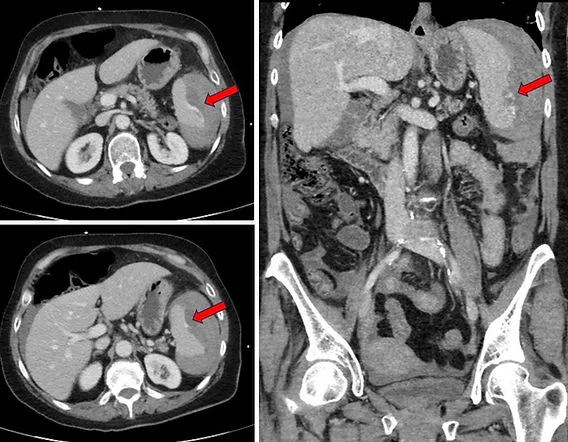
CT Scan with IV Contrast: Gold standard for hemodynamically stable patients. Accurately identifies specific organ injury, retroperitoneal hemorrhage, and quantifies bleeding.
-
Diagnostic Peritoneal Lavage (DPL): Invasive and largely historical. Considered only if FAST/CT are unavailable in an unstable patient.
⭐ The FAST exam is excellent for detecting hemoperitoneum but poor for retroperitoneal, diaphragmatic, or hollow viscus injuries.
Organ-Specific Injuries - The Damage Report
- Spleen: Most commonly injured organ in blunt abdominal trauma.
- Liver: Second most common.
- Injury Grading: Standardized scales (AAST Grade I-V for spleen, I-VI for liver) assess severity and guide management.
Management Approach
- Non-Operative Management (NOM): Preferred for many solid organ injuries. Key criteria include:
- Hemodynamic stability.
- No signs of peritonitis.
- Absence of other injuries requiring surgery.
- Angioembolization: A key adjunct to NOM for patients with active arterial extravasation on CT scan but who are otherwise stable.
- Surgery (Exploratory Laparotomy): Indicated for:
- Hemodynamic instability.
- Peritonitis.
- Failure of NOM/angioembolization.
⭐ Kehr's sign: Referred pain to the left shoulder due to phrenic nerve irritation from a splenic rupture. A classic exam finding.
High‑Yield Points - ⚡ Biggest Takeaways
- The spleen is the most commonly injured organ in blunt abdominal trauma, followed by the liver.
- In unstable patients, the eFAST exam is the primary diagnostic tool to assess for hemoperitoneum.
- Hemodynamically stable patients should undergo a CT scan with IV contrast for accurate injury grading.
- Non-operative management is the standard for most solid organ injuries in stable patients.
- A "seatbelt sign" strongly suggests underlying hollow viscus or mesenteric injury.
- Retroperitoneal injuries (e.g., pancreas, duodenum) can be occult on initial FAST scan.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

