Indications & Contraindications - The Transplant Gates
-
Indications (Who gets a new liver?)
- Acute Liver Failure (e.g., fulminant hepatitis).
- Chronic Liver Disease/Cirrhosis with decompensation (ascites, encephalopathy, variceal bleeds).
- Hepatocellular Carcinoma (HCC) meeting specific criteria.
- Certain metabolic diseases (e.g., Wilson's disease).
-
Contraindications (Who doesn't?)
- Absolute: Severe cardiopulmonary disease, active extrahepatic malignancy, uncontrolled sepsis, active substance abuse.
- Relative: Morbid obesity, poor psychosocial support, non-adherence.
⭐ Milan Criteria for HCC: Solitary tumor ≤ 5 cm, or up to 3 tumors each ≤ 3 cm, with no extrahepatic spread or major vascular invasion.
Pre-transplant Evaluation - The MELD Meter
- MELD Score (Model for End-Stage Liver Disease): Objectively predicts 3-month mortality risk in patients with cirrhosis to guide organ allocation.
- Core Components:
- Total Bilirubin
- International Normalized Ratio (INR)
- Creatinine
- Serum Sodium (in MELD-Na variant)
- 📌 Mnemonic: I Crush Beer Smoothly (INR, Creatinine, Bilirubin, Sodium).
- Scoring: Ranges from 6 (less ill) to 40 (gravely ill). A higher score indicates a greater urgency for transplantation.
⭐ MELD Exceptions: Patients with conditions like Hepatocellular Carcinoma (HCC) receive standardized MELD "exception points" to ensure equitable access to transplant, as their lab-based MELD score may not fully reflect their mortality risk.
Surgery & Donors - The Great Liver Swap
- Donors: Deceased (DDLT) or living-donor (LDLT). Split-liver technique can create two grafts from one donor liver.
- Surgical Technique:
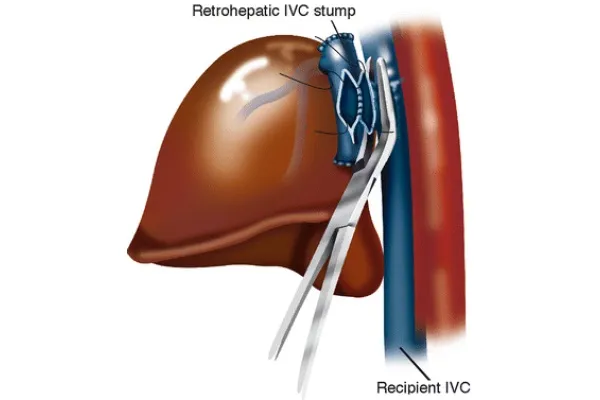
- Classical: Total hepatectomy with IVC resection.
- Piggyback: Preserves recipient IVC, reducing hemodynamic instability.
- Anastomosis Order: Suprahepatic IVC, infrahepatic IVC, portal vein, hepatic artery, then biliary duct.
⭐ High-Yield: The hepatic artery is the most common site of post-transplant thrombosis, often leading to graft failure.
Post-Op Management - Bugs, Drugs & Rejection
-
Infection Timeline:
- <1 Month: Bacterial (nosocomial, line-related), Candida, HSV.
- 1-6 Months: Opportunistic pathogens. Key threats are Cytomegalovirus (CMV), Pneumocystis jirovecii (PJP), and Aspergillus.
- >6 Months: Standard community-acquired pathogens.
-
Core Immunosuppression:
- Calcineurin Inhibitor (CNI): Tacrolimus (mainstay).
- Antimetabolite: Mycophenolate Mofetil (MMF).
- Corticosteroids: Prednisone (tapered).
-
Rejection:
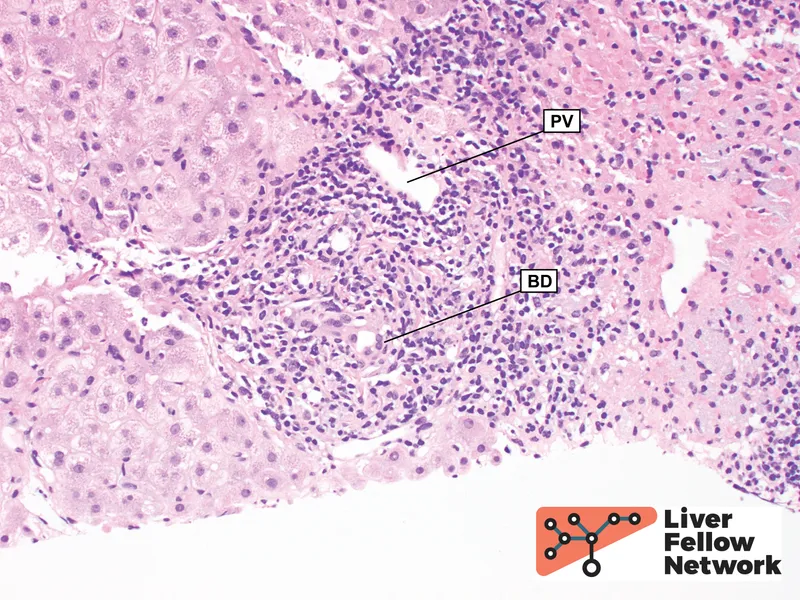
- Acute Cellular (ACR): T-cell mediated, common in first few months. Presents with ↑LFTs. Dx: Biopsy. Tx: Steroid bolus.
- Chronic: Late (>1 yr), ductopenic rejection (vanishing bile duct syndrome). Leads to graft failure.
⭐ CMV is a major cause of allograft dysfunction and morbidity in the 1-6 month window. Prophylaxis (e.g., Valganciclovir) is standard for at-risk patients.
- The MELD score (Bilirubin, INR, Creatinine) is paramount for organ allocation, predicting 3-month mortality.
- Primary indications include decompensated cirrhosis (ascites, encephalopathy, variceal bleeding) and hepatocellular carcinoma within Milan criteria.
- Key absolute contraindications are severe cardiopulmonary disease, extrahepatic malignancy, and active substance abuse.
- Post-transplant immunosuppression typically involves tacrolimus, mycophenolate, and corticosteroids.
- Hepatic artery thrombosis is the most devastating early vascular complication.
- Acute cellular rejection is T-cell mediated; treat with high-dose steroids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

