Indications & Workup - The Kidney Waitlist
- Indication: End-Stage Renal Disease (ESRD) with GFR < 15 mL/min/1.73m² or patient on dialysis.
- Core Workup:
- ABO & HLA typing (A, B, DR loci)
- Panel Reactive Antibody (PRA) to assess sensitization
- Infection screen (HIV, HBV, HCV, CMV)
- Cardiovascular & psychosocial evaluation
- Key Contraindications:
- Absolute: Active malignancy, uncontrolled infection, severe end-organ damage.
- Relative: Morbid obesity (BMI > 40), active substance abuse, nonadherence.
⭐ High Panel Reactive Antibody (PRA) signifies broad sensitization to donor HLAs, prolonging wait times and increasing rejection risk.
Immunosuppression - Taming the Defenses
- Goal: Prevent rejection (hyperacute, acute, chronic) while minimizing drug toxicity & infection risk.
- Phases: Induction (at transplant), Maintenance (lifelong), Rejection treatment.
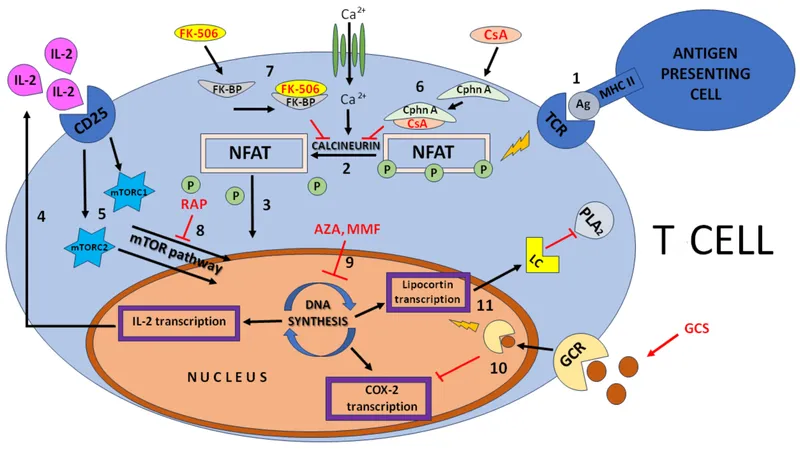
| Drug Class | Examples & MOA | Key Side Effects |
|---|---|---|
| Calcineurin Inhibitors | Tacrolimus, Cyclosporine - Inhibit IL-2 transcription | Nephrotoxicity, neurotoxicity, hypertension, hyperkalemia. |
| Antimetabolites | Mycophenolate Mofetil - Inhibits purine synthesis | GI distress (diarrhea), bone marrow suppression, ↑ CMV risk. |
| mTOR Inhibitors | Sirolimus - Blocks IL-2 signal transduction | Hyperlipidemia, poor wound healing, proteinuria, pneumonitis. |
| Corticosteroids | Prednisone - Broad anti-inflammatory | Hyperglycemia, osteoporosis, weight gain, mood changes. |
Surgical Technique - The Retroperitoneal Tuck
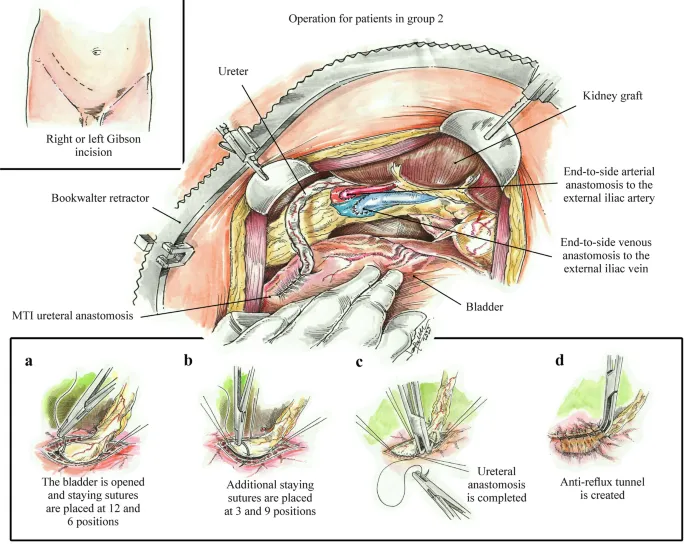
- Placement: The donor kidney is placed in the iliac fossa, remaining outside the peritoneal cavity (extraperitoneal). This protects the graft from potential peritonitis and allows for easier access for biopsy.
- Anastomosis Sequence:
- Vascular: Donor renal vein and artery are connected to the recipient's external iliac vein and internal/external iliac artery, respectively.
- Urinary: The donor ureter is implanted into the bladder (ureteroneocystostomy).
⭐ High-Yield: The most common urologic complication is ureteral obstruction, often at the vesicoureteric anastomosis site, leading to hydronephrosis and graft dysfunction.
Post-Op Complications - Rejection & Other Woes
-
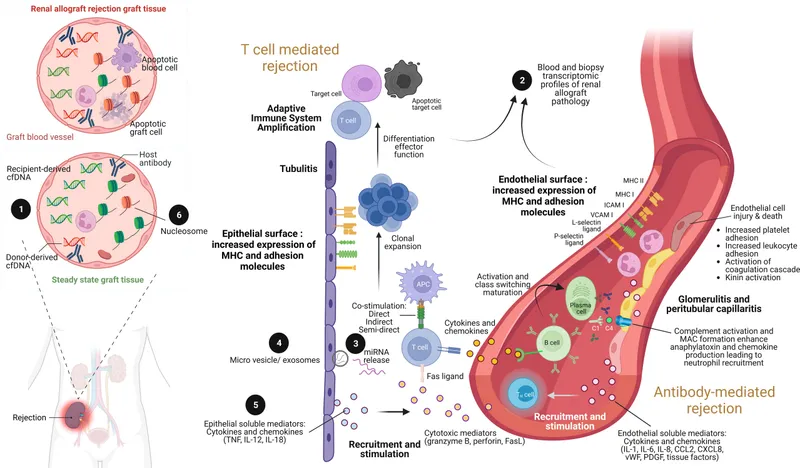
Rejection Types & Timeline
- Hyperacute: Pre-existing recipient antibodies against donor antigens. Gross mottling & cyanosis.
- Acute: Cellular (T-cell) or humoral (antibody) response. Most common type, usually reversible. Presents with ↑ creatinine, fever, graft tenderness.
- Chronic: Slow, progressive graft dysfunction. Dominated by interstitial fibrosis & tubular atrophy.
-
Other Major Complications
- Thrombosis: Renal artery or vein. Early post-op emergency.
- Urine Leak: Breakdown of ureter-bladder anastomosis.
- Infection: High risk due to immunosuppression. 📌 CMV, BK virus.
- Drug Toxicity: Calcineurin inhibitors (Tacrolimus, Cyclosporine) are nephrotoxic.
⭐ BK virus nephropathy can mimic acute cellular rejection. Both present with a rising creatinine. Diagnosis requires graft biopsy to look for viral inclusions vs. lymphocytic infiltrates.
High‑Yield Points - ⚡ Biggest Takeaways
- Living donor kidneys offer superior graft survival compared to deceased donor organs.
- Hyperacute rejection is a type II hypersensitivity due to pre-formed antibodies, causing immediate graft failure.
- Acute rejection is most commonly T-cell mediated within the first few months and responds to steroids.
- Calcineurin inhibitors (Tacrolimus) are cornerstone immunosuppressants but are nephrotoxic.
- Watch for renal artery stenosis as a cause of new-onset hypertension post-transplant.
- Prophylaxis for CMV and PCP is crucial in the immediate post-transplant period.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

