SSI Classification - Bugs on the Prowl
-
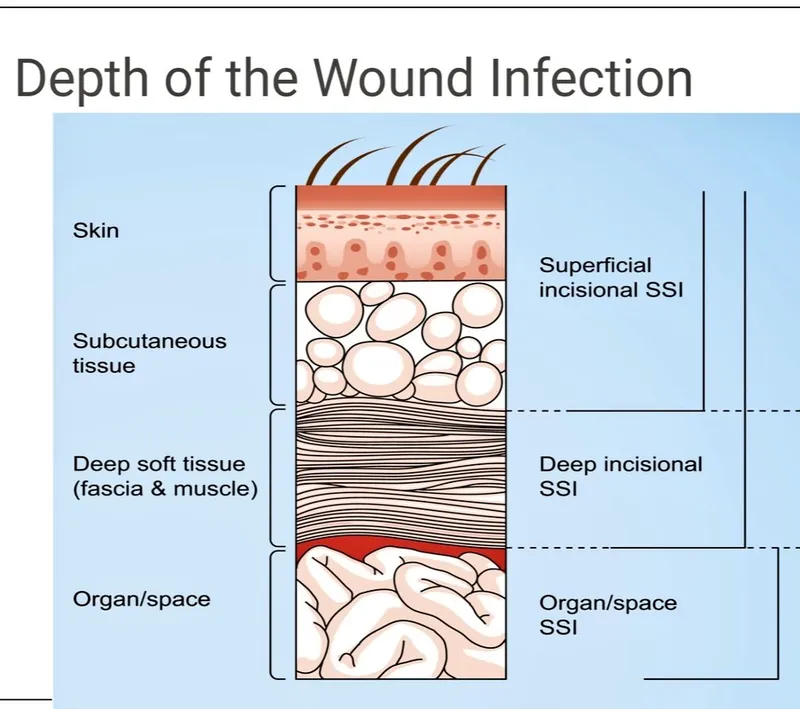
Superficial Incisional SSI:
- Involves skin & subcutaneous tissue.
- Occurs within 30 days of surgery.
- Bugs: S. aureus, Coag-neg Staph, Streptococcus.
-
Deep Incisional SSI:
- Involves deep soft tissues (fascia & muscle).
- Occurs within 30-90 days (if implant present).
- Bugs: As above + gram-negatives (e.g., E. coli).
-
Organ/Space SSI:
- Involves any organ/space opened during surgery.
- Occurs within 30-90 days (if implant present).
- Bugs: Specific to the organ (e.g., anaerobes like Bacteroides fragilis in abdominal surgery).
⭐ Most SSIs are caused by the patient's own endogenous flora. Staphylococcus aureus is the #1 culprit overall.
Risk & Prevention - Fortress Against Infection
- Patient Factors: Smoking, obesity (BMI > 30), malnutrition (albumin < 3.5), uncontrolled diabetes (HbA1c > 7%), immunosuppression, and nasal S. aureus carriage.
- Procedural Factors: Higher wound contamination class, prolonged surgery duration, poor hemostasis (hematoma), and emergency procedures.
- Prevention Bundle:
- Pre-op: Glucose control (<180 mg/dL), chlorhexidine showers, hair clipping (no razors), and prophylactic antibiotics within 60 minutes before incision.
- Intra-op: Maintain normothermia, use aseptic technique.
- Post-op: Sterile dressing for 24-48 hours.
⭐ For prophylaxis, Cefazolin is the workhorse. Use Vancomycin or Clindamycin for severe β-lactam allergies. Redose for surgeries >4 hours or with major blood loss (>1500 mL).
Diagnosis & Workup - The Infection Detective
-
Clinical Picture: Based on signs appearing 5-7 days post-op.
- Local: New pain, erythema, swelling, warmth, or purulent drainage.
- Systemic: Fever (>38°C / 100.4°F), tachycardia, leukocytosis (↑ WBC).
-
Diagnostic Steps:
- Wound Assessment: Gently probe incision with a sterile swab.
- Microbiology: Obtain wound culture & Gram stain before antibiotics. Blood cultures if systemic signs are present.
- Imaging: Use Ultrasound or CT to detect deep collections or abscesses.
⭐ Infections within 24-48 hours are rare but aggressive; suspect Group A Strep or Clostridium perfringens.

Management Strategy - The Clean-Up Crew
- Source Control is Paramount: Open the wound, drain purulence, and remove sutures/staples.
- Obtain Cultures: Always collect wound cultures before starting antibiotics to guide therapy.
- Healing by Secondary Intention: Most opened wounds are packed and allowed to heal from the base up.
- 📌 Mnemonic (I-C-A): Incise & Drain → Culture → Antibiotics.
⭐ Exam Favorite: Failure of a post-op fever to resolve after 48-72 hours despite empiric antibiotics strongly suggests a collection (abscess) requiring urgent source control, typically surgical drainage.
High‑Yield Points - ⚡ Biggest Takeaways
- Most SSIs manifest 5-7 days post-op; suspect Group A Strep or Clostridium if within 48 hours.
- Key signs include localized pain, erythema, warmth, and purulent drainage from the incision.
- Diagnosis is primarily clinical; wound cultures are for guiding, not delaying, therapy.
- Management cornerstone is source control: open the wound, drain abscesses, and debride nonviable tissue.
- Use systemic antibiotics only for significant cellulitis (>5 cm) or systemic signs of infection.
- Staphylococcus aureus is the most common pathogen responsible for SSIs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

