🗺️ Anatomy - Pelvic Floor Blueprint
- Muscular Diaphragm: Levator ani (puborectalis, pubococcygeus, iliococcygeus) & coccygeus muscle.
- Innervation: Pudendal nerve (S2-S4) & direct branches from sacral plexus.
- Connective Tissue: Endopelvic fascia (ligaments & fascia).
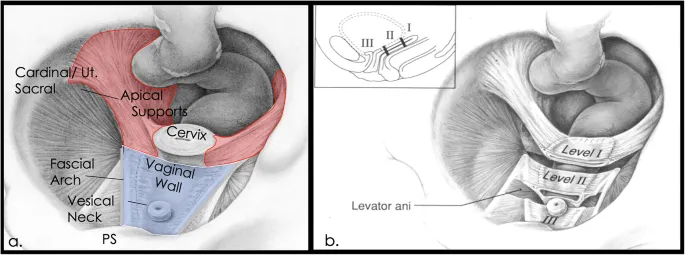
⭐ Defects in Level I support (apical) are critical, leading to uterine or vault prolapse. Repair targets re-suspension, often via uterosacral or sacrospinous ligament fixation.
📉 Clinical Manifestations - Downward Spiral Symptoms
- Primary Symptom: Pelvic pressure or a vaginal bulge ("sitting on a ball").
- Worsens with ↑ intra-abdominal pressure (coughing, straining, standing).
- Urinary:
- Stress incontinence (SUI) is common.
- Obstructive symptoms: hesitancy, incomplete emptying.
- Bowel:
- Constipation, incomplete evacuation.
- 📌 Splinting: Patient manually presses on the perineum or posterior vaginal wall to defecate.
- Sexual: Dyspareunia, decreased sensation.
⭐ Masked SUI: A severe prolapse (e.g., cystocele) can kink the urethra, hiding SUI. Correcting the prolapse can unmask incontinence.
📏 Grading the Drop
- Pelvic Organ Prolapse Quantification (POP-Q) System: The standardized, objective method for grading POP.
- Reference Point: The hymen is the fixed point of reference, designated as 0 cm.
- Points proximal (inside) are negative (e.g., $-1$ cm).
- Points distal (outside) are positive (e.g., $+1$ cm).
| Stage | Prolapse Extent (Relative to Hymen) |
|---|---|
| 0 | No prolapse detected. |
| 1 | Most distal point > 1 cm above. |
| 2 | Most distal point ≤ 1 cm proximal or distal. |
| 3 | Most distal point > 1 cm below. |
| 4 | Complete eversion (procidentia). |
🏗️ Management - The Up-Lifting Fix
Management depends on symptoms, severity, and patient goals (e.g., maintaining sexual function).
- Conservative:
- Vaginal pessary (supportive device).
- Pelvic floor muscle training (Kegels).
- Topical estrogen for atrophy.
- Surgical (Reconstructive):
- Apical: Sacrocolpopexy, Uterosacral Ligament Suspension.
- Anterior/Posterior: Colporrhaphy.
- Surgical (Obliterative):
- Colpocleisis: Closes the vagina. For frail, non-sexually active patients.
⭐ Sacrocolpopexy (attaching vaginal vault to sacrum, often with mesh) is the most durable repair for apical prolapse.
⚠️ Transvaginal mesh has a high risk of complications like erosion and pain.
⚠️ Post-Op Pitfalls
- Urinary Retention: Common, often transient; may require temporary catheterization.
- Mesh-Specific Complications:
- Erosion/Exposure: Presents with vaginal discharge, bleeding, dyspareunia.
- Chronic Pain: Pelvic pain, dyspareunia.
- Voiding Dysfunction: De novo urgency or stress urinary incontinence (SUI).
- Organ Injury (Intra-op): Rare; bladder, ureter, bowel.
- Recurrence: Long-term failure of the surgical repair.
⭐ Mesh erosion is a key complication of synthetic mesh, presenting months to years post-op. Suspect in patients with new vaginal bleeding, discharge, or dyspareunia.
⚡ Biggest Takeaways
- Conservative management (pessaries, pelvic floor exercises) is first-line, especially for poor surgical candidates.
- Sacrocolpopexy is the gold standard for apical prolapse (vault/uterus), offering the highest durability.
- Uterosacral ligament suspension, a native tissue repair, carries a significant risk of ureteral injury.
- Transvaginal mesh is associated with high rates of mesh erosion, pain, and dyspareunia.
- Colpocleisis (vaginal obliteration) is a definitive, low-morbidity option for elderly, non-sexually active women.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

