🔪 Pathophysiology - Why Surgery?
Surgery is indicated when medical therapy fails or when complications of chronic inflammation arise. The goal is to manage structural damage, control sepsis, or prevent malignancy.
Common Indications:
- Failure of Medical Therapy: Disease refractory to biologics/immunomodulators.
- Complications (Crohn's): 📌 F-SOAP
- Fistula, Stricture/Obstruction, Abscess, Perforation.
- Complications (UC):
- Toxic megacolon (colonic diameter >6 cm)
- Fulminant colitis unresponsive to therapy.
- Uncontrolled hemorrhage.
- Dysplasia or colorectal cancer (CRC).
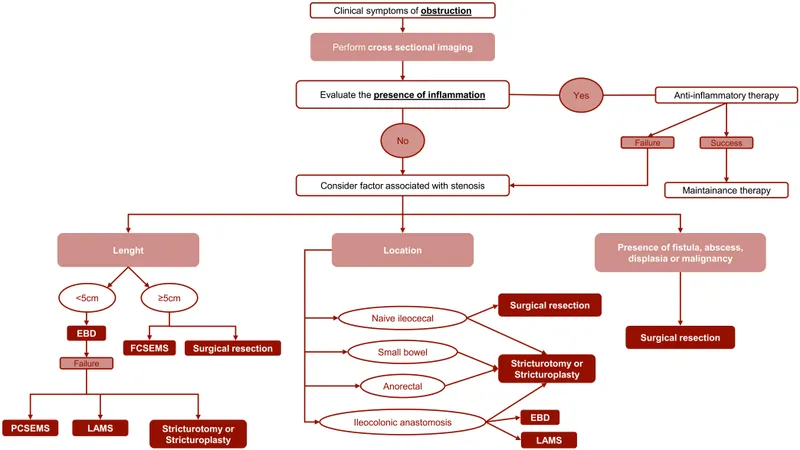
⭐ Surgery is curative for Ulcerative Colitis (total proctocolectomy), but only palliative for Crohn's Disease due to high recurrence rates.
🔪 Surgical Indications
⭐ UC: Total proctocolectomy is curative. Crohn's: Surgery is palliative for complications; recurrence is common, often at the anastomosis.
Emergent/Urgent:
- Toxic megacolon (transverse colon >6 cm + toxicity)
- Bowel perforation
- Massive, uncontrolled hemorrhage
- Fulminant colitis refractory to 72 hrs of IV steroids
Elective:
- Medically refractory disease (steroid dependence, growth failure)
- Dysplasia or carcinoma on surveillance colonoscopy
- Crohn's-specific: Symptomatic strictures, non-healing fistulas, intra-abdominal abscesses
🛠️ Management - The Surgeon's Toolkit
Crohn's Disease (CD): Bowel Conservation is Key
- Strictureplasty: Widens fibrotic strictures (e.g., Heineke-Mikulicz) without resection, preserving bowel length.
- Limited Resection: For complications like fistula, abscess, perforation, or obstruction. Remove only grossly affected bowel with clear margins.
- Anastomosis: Side-to-side (e.g., Kono-S) may ↓ recurrence vs. end-to-end.
Ulcerative Colitis (UC): Resection is Curative
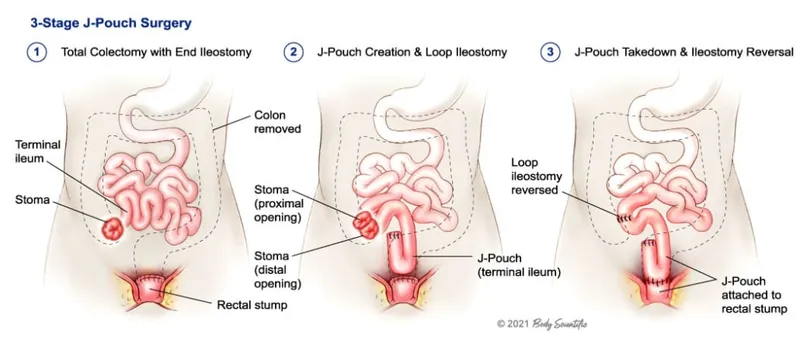
- Total Proctocolectomy (TPC) with Ileal Pouch-Anal Anastomosis (IPAA / J-Pouch):
- Gold standard for elective cases (dysplasia, refractory disease).
- Restores fecal continence. ⚠️ Risk of pouchitis.
- TPC with End Ileostomy (Brooke Ileostomy): For patients not candidates for IPAA (poor sphincter function, distal rectal cancer).
- Emergent Subtotal Colectomy: For toxic megacolon/perforation. Leaves rectal stump (Hartmann's pouch); IPAA can be done later (staged procedure).
⭐ Surgical Philosophy: Surgery for UC is curative (removes all diseased mucosa), while for CD it is palliative for complications, as disease often recurs proximal to the anastomosis.
⚠️ Complications - Post-Op Perils
- Anastomotic Leak:
- Most feared early complication.
- Presents with fever, tachycardia, peritonitis.
- Dx: CT with oral/rectal contrast.
- Small Bowel Obstruction (SBO):
- Commonly due to adhesions.
- Pouch-Specific (IPAA for UC):
- Pouchitis: Most common long-term issue; inflammation of the ileal pouch.
- Cuffitis: Inflammation of the rectal cuff remnant.
- Crohn's Disease Specific:
- High rate of disease recurrence at the anastomotic site.
⭐ Pouchitis after IPAA presents with ↑ stool frequency, urgency, and cramps. First-line treatment is antibiotics (Metronidazole or Ciprofloxacin).
⚡ Biggest Takeaways
- Ulcerative Colitis (UC) surgery is curative; Crohn's Disease (CD) surgery is palliative for complications.
- The standard procedure for UC is total proctocolectomy with ileal pouch-anal anastomosis (IPAA).
- Pouchitis is the most common long-term complication of an IPAA; treat with metronidazole/ciprofloxacin.
- For CD, the goal is bowel preservation; strictureplasty is preferred over resection for fibrotic strictures.
- Key indications for UC surgery: dysplasia/cancer, toxic megacolon, or medically refractory disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

