Pediatric Patients - Not Just Little Adults
- Higher metabolic rate & larger body surface area-to-mass ratio → ↑ insensible fluid losses.
- Maintenance fluid needs are calculated using the Holliday-Segar Method (the "4-2-1 Rule"):
- 4 mL/kg/hr for the first 10 kg of body weight.
- 2 mL/kg/hr for the next 10 kg (11-20 kg).
- 1 mL/kg/hr for each subsequent kg (>20 kg).

⭐ To reduce the risk of iatrogenic hyponatremia, isotonic fluids (e.g., D5 0.9% NaCl) are now preferred over traditional hypotonic maintenance fluids for most pediatric patients.
Geriatric Patients - Handle With Care
- Physiology: ↓ total body water, ↓ GFR, blunted thirst mechanism, and altered ADH response.
- High Risk: Prone to both dehydration and iatrogenic fluid overload due to narrow therapeutic window.
- Management Principle: "Start low and go slow."
- Maintenance fluids: Reduce to 20-25 mL/kg/day.
- For resuscitation, use smaller boluses (e.g., 250-500 mL) and reassess frequently.
- Crucial monitoring: Daily weights, strict I/Os, mental status.
⭐ Be vigilant for heart failure exacerbation. The presence of an S3 gallop, JVD, or new/worsening crackles indicates fluid overload and requires immediate cessation of IV fluids and potential diuresis.
Pregnancy & Burns - Bumps and Burns
Pregnancy:
- Physiologic ↑ in plasma volume by ~50% & ↑ GFR.
- ↓ colloid osmotic pressure increases risk of pulmonary edema with over-resuscitation.
- Generally, maintenance fluids are adequate; use crystalloids judiciously.
Burns:
- Massive fluid loss necessitates aggressive resuscitation to prevent hypovolemic shock.
- 📌 "Rule of 9s" used to estimate Total Body Surface Area (%TBSA) for burns.
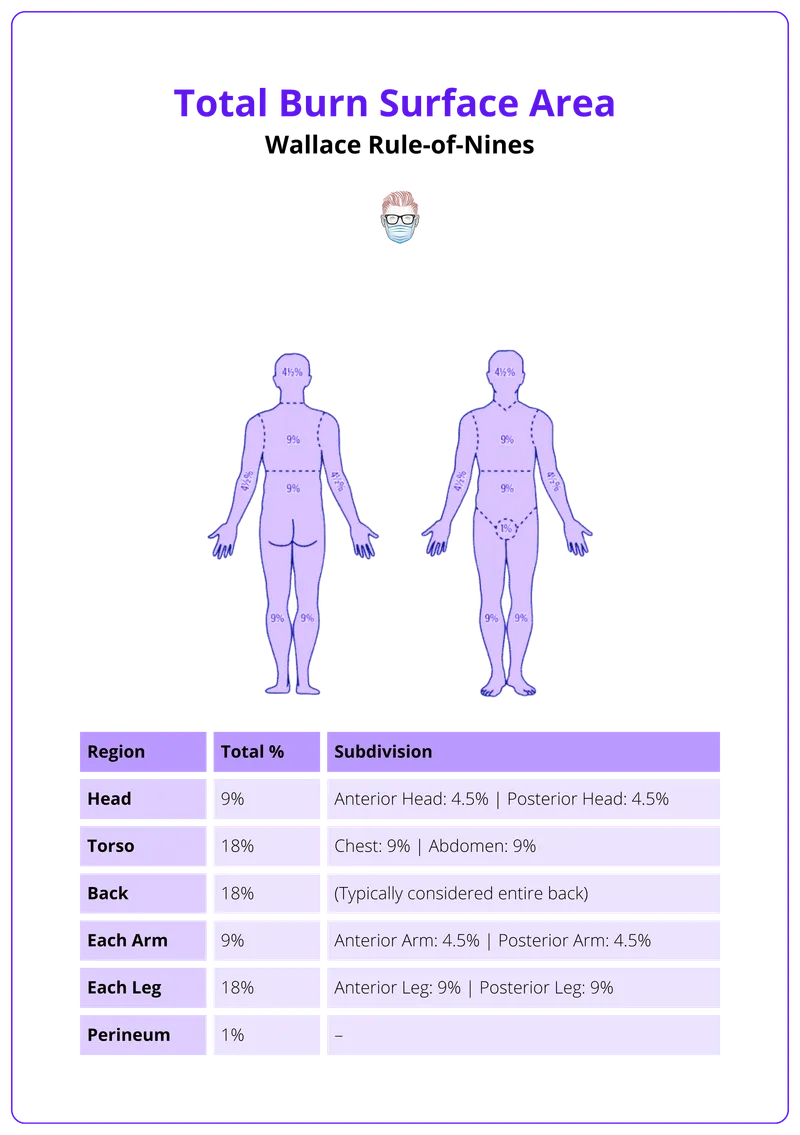
- Parkland Formula for 24-hr fluid requirement:
- $4 \text{ mL} \times \text{Body Wt (kg)} \times % \text{TBSA burn}$
- Fluid: Lactated Ringer's.
- Timing: Give 50% in first 8 hrs (from burn onset), 50% over next 16 hrs.
⭐ Urine output (0.5-1.0 mL/kg/hr) is the most critical indicator of adequate fluid resuscitation in burn patients.
Cardiac & Renal Failure - Walking a Tightrope
Fluid management in patients with significant cardiac (HF) or renal (CKD) dysfunction is a delicate balance aimed at maintaining euvolemia. The guiding principle is "start low, go slow" to prevent iatrogenic harm from fluid shifts.
- Primary Goal: Avoid both fluid overload (→ pulmonary edema, worsening HF) and hypovolemia (→ pre-renal azotemia, decreased cardiac output).
- Vigilant Monitoring:
- Daily weights are the most reliable single indicator of net fluid change.
- Closely track Intake/Output (I/Os), JVP, peripheral and pulmonary edema.
- Labs: Monitor serial BUN/Creatinine.
- Therapeutic Strategy:
- If hypovolemia is suspected, administer small, slow fluid challenges (e.g., 250 mL crystalloid bolus) followed by immediate clinical reassessment.
- For fluid overload, the mainstay is loop diuretics (e.g., IV furosemide) to achieve negative fluid balance.
⭐ High-Yield: In a hypotensive patient with decompensated heart failure, the cause is often cardiogenic shock (pump failure), not hypovolemia. Giving large fluid volumes can be lethal; inotropes are required.
High‑Yield Points - ⚡ Biggest Takeaways
- In Traumatic Brain Injury (TBI), avoid hypotonic fluids; use isotonic or hypertonic saline to prevent cerebral edema.
- For severe burns, use the Parkland formula (4 mL/kg/%TBSA) with Lactated Ringer's for resuscitation.
- In Congestive Heart Failure (CHF) and cirrhosis, prioritize sodium and water restriction and cautious diuresis.
- End-Stage Renal Disease (ESRD) requires careful volume management, often restricting fluids to match output.
- In malnutrition, correct electrolytes (phosphate, K⁺, Mg²⁺) before fluids to prevent refeeding syndrome.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

