⚠️ The Risky Trio
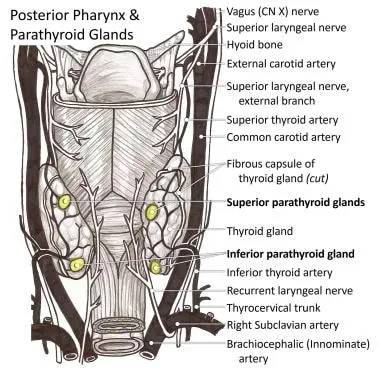
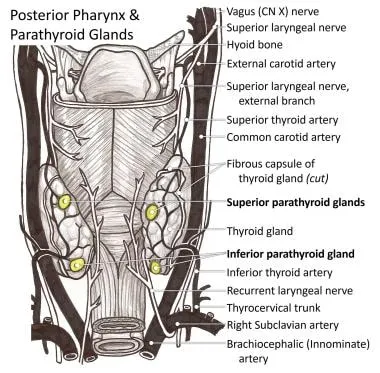
- Nerve Injury:
- Recurrent Laryngeal (RLN): Unilateral injury → hoarseness. Bilateral → inspiratory stridor, airway emergency.
- Superior Laryngeal (SLN): External branch injury → loss of high-pitched voice, vocal fatigue.
- Hypoparathyroidism:
- Inadvertent removal/devascularization of parathyroid glands → ↓PTH → Hypocalcemia.
⭐ Hypocalcemia: Presents with perioral numbness and tingling (paresthesias). Elicit Chvostek (facial twitch) and Trousseau (carpal spasm) signs. Severe cases can cause tetany and seizures.
🤕 Complications - Gland-Specific Grief
Thyroidectomy
- Hypocalcemia: Most common complication. Due to parathyroid devascularization or inadvertent removal.
- Symptoms: Perioral numbness, paresthesias, muscle cramps.
- Signs: Chvostek (facial twitch), Trousseau (carpal spasm with BP cuff).
- Nerve Injury:
Nerve Injury Manifestation Recurrent Laryngeal (RLN) Unilateral: Hoarseness, breathy voice. Bilateral: Acute airway obstruction (stridor). Superior Laryngeal (SLN) Loss of high-pitched voice; vocal fatigue. Often subtle. - Hematoma: Expanding neck mass can cause rapid airway compromise. A surgical emergency.
Parathyroidectomy
- Hypocalcemia: Can be severe and prolonged ("Hungry Bone Syndrome") in patients with severe pre-op bone disease (e.g., osteitis fibrosa cystica).
- Persistent/Recurrent Hyperparathyroidism: Due to missed adenoma, ectopic gland, or parathyroid hyperplasia.
Adrenalectomy
- Adrenal Insufficiency/Crisis: Requires vigilant post-op steroid replacement, especially after bilateral removal or for Cushing's syndrome.
- Hypertensive Crisis: During manipulation of a pheochromocytoma; requires pre-op alpha-blockade.
⭐ Pearl: Transient hypocalcemia is the most common complication following total thyroidectomy, occurring more frequently than permanent nerve injury.
Post-Thyroidectomy Hypocalcemia Management
🩺 Diagnosis - Finding the Fault
-
Hypocalcemia:
- Labs: ↓ Ionized Calcium, ↓ PTH, ↑ Phosphate.
- Signs: Positive Chvostek's (facial twitch) & Trousseau's (carpal spasm).
- ECG: Prolonged QT interval.
-
Nerve Injury:
- Recurrent Laryngeal (RLN): Laryngoscopy shows vocal cord paralysis. Unilateral → hoarseness. Bilateral → stridor, airway emergency.
- Superior Laryngeal (SLN): Laryngoscopy/stroboscopy reveals vocal cord bowing/asymmetry. Patient reports loss of high pitch.
-
Neck Hematoma:
- Primarily a clinical diagnosis: rapid neck swelling, dyspnea, stridor.
- Ultrasound can confirm fluid collection.
⭐ Post-thyroidectomy, a precipitous drop in PTH within 1-6 hours of surgery is highly predictive of symptomatic hypocalcemia.
- Hypothyroidism:
- Labs: ↑ TSH, ↓ Free T4.
🚑 Management - The Rescue Mission
- Post-Op Stridor/Airway Compromise: Immediate action required.
-
Hypocalcemia ($Ca^{2+} < 8.5$ mg/dL):
- Symptomatic (tetany, seizures, QT prolongation): IV Calcium Gluconate.
- Asymptomatic/Mild: Oral Calcium Carbonate + Calcitriol (active Vit D).
-
Thyroid Storm:
- 📌 4 P's: Propranolol (β-blocker), Propylthiouracil (PTU), Prednisone (corticosteroids), Potassium Iodide (SSKI).
⭐ High-Yield: For a tense, expanding neck hematoma, the immediate life-saving step is opening the surgical incision at the bedside to decompress the airway. Do not delay for OR transport.
⚡ Biggest Takeaways
- Thyroidectomy: Hypocalcemia (parathyroid injury) is most common. Recurrent laryngeal nerve injury causes hoarseness; bilateral is an airway emergency.
- Superior laryngeal nerve injury causes loss of high-pitched voice.
- Parathyroidectomy: Watch for hungry bone syndrome (severe hypocalcemia) and persistent hyperparathyroidism (missed adenoma).
- Pheochromocytoma resection: Risk of intraoperative hypertensive crisis; requires pre-op alpha-blockade.
- Adrenalectomy for Cushing's: Post-op adrenal insufficiency is common; requires steroid replacement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

