🗺️ Anatomy - Location, Location, Adrenal!
- Location: Retroperitoneal, superomedial to kidneys.
- Key Relations:
- Right Gland (Pyramidal): Posterior to the IVC and liver.
- Left Gland (Crescentic): Medial to the spleen; posterior to the pancreas tail; lateral to the aorta.
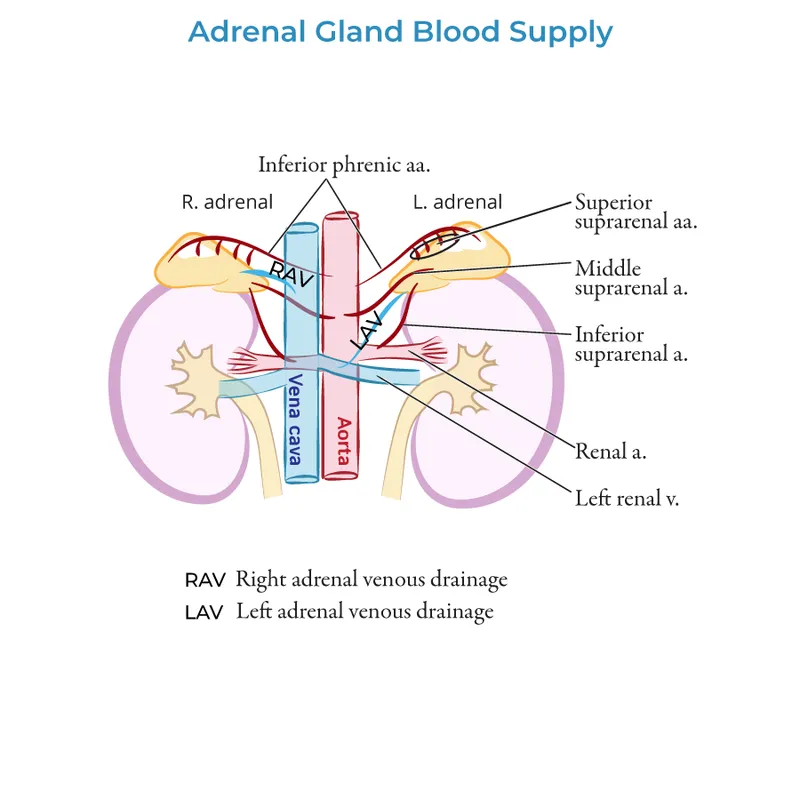
-
Arterial Supply (x3):
- Superior Adrenal A. (from Inferior Phrenic A.)
- Middle Adrenal A. (from Aorta)
- Inferior Adrenal A. (from Renal A.)
-
Venous Drainage (Asymmetric):
- Right Adrenal V. $\rightarrow$ IVC (short, direct)
- Left Adrenal V. $\rightarrow$ Left Renal V. (longer)
⭐ The short Right Adrenal Vein draining directly into the IVC increases the risk of hemorrhage and IVC injury during right adrenalectomy.
🔪 Management - The Surgical Game Plan
The choice of adrenalectomy approach hinges on tumor size, suspicion of malignancy, and patient factors.
| Approach | Indications | Patient Factors | Advantages | Disadvantages |
|---|---|---|---|---|
| Lap Transabdominal | Benign tumors <6-8 cm | Standard anatomy | Familiar view, large space | Bowel handling, visceral risk |
| Lap Retroperitoneal | Small tumors <5 cm, bilateral | Obesity, prior abd. surgery | Direct access, avoids bowel | Small space, technically hard |
| Open | ACC, tumors >10 cm, invasion | Driven by tumor | En bloc resection, controls large vessels | ↑ morbidity, long recovery |

⚠️ Complications - When Things Go South
-
Intra-operative
- Hemorrhage: High risk from the short, friable central adrenal vein, especially on the right (direct IVC entry).
- Organ Injury:
- Left-sided: Spleen (most common), pancreas tail, kidney.
- Right-sided: Liver, duodenum, IVC.
- Hypertensive Crisis: Due to catecholamine release from pheochromocytoma manipulation.
-
Post-operative
- Adrenal Insufficiency: Critical risk after removing a cortisol-producing adenoma (suppressed contralateral gland) or bilateral adrenalectomy. Requires stress-dose steroids.
- Thromboembolism (DVT/PE): Increased risk in Cushing's syndrome.
- General: Atelectasis, wound infection.
⭐ Pheochromocytoma: Intra-op catecholamine surge from tumor handling can cause life-threatening hypertension & tachycardia. Pre-op alpha-blockade (e.g., phenoxybenzamine) is crucial to prevent this.
⚡ Biggest Takeaways
- Laparoscopic adrenalectomy is the gold standard for most benign tumors (<6 cm).
- Transperitoneal (TLA) is the most common approach, offering a larger working space.
- Posterior retroperitoneal (PRA) is ideal for bilateral tumors, obesity, or prior abdominal surgery.
- Open adrenalectomy is mandatory for large (>10 cm) or suspected malignant tumors (ACC) to ensure complete resection.
- Major risks include spleen/pancreas injury (left) and liver/IVC injury (right).
- For pheochromocytoma, preoperative alpha-blockade is crucial to prevent hypertensive crisis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

