🗺️ Anatomy - Mediastinal Geography
- Definition: Central compartment of the thoracic cavity, located between the two pleural sacs.
- Boundaries:
- Superior: Thoracic inlet
- Inferior: Diaphragm
- Anterior: Sternum
- Posterior: Vertebral column
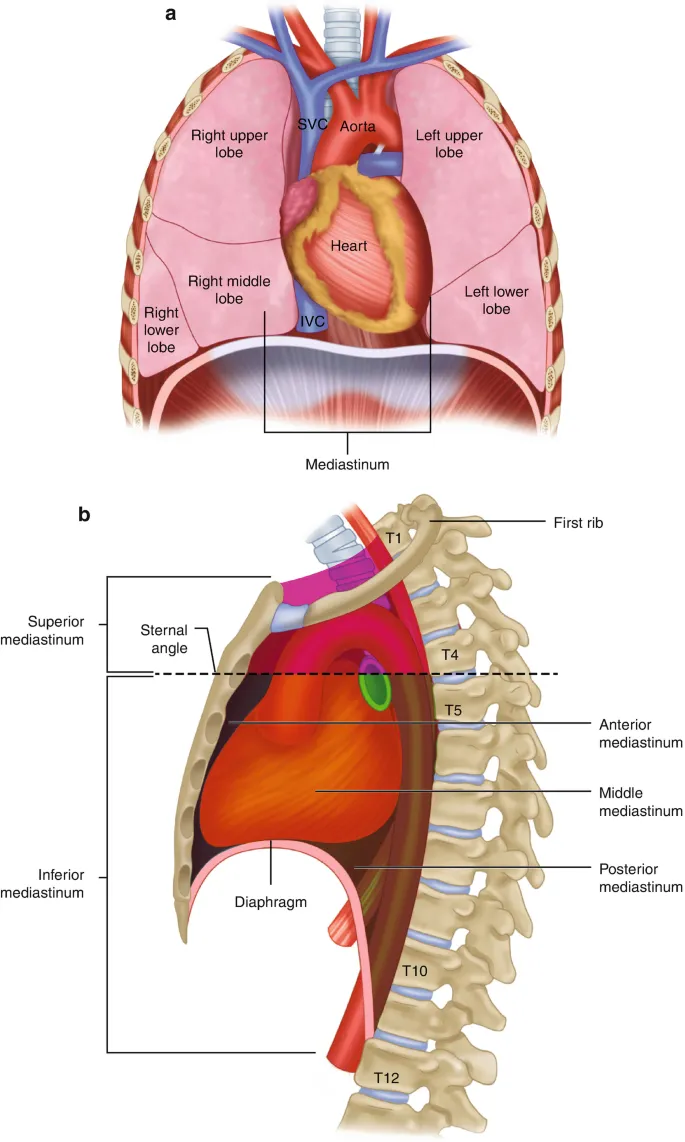
- Clinical Divisions (Felson Method):
- Anterior: From sternum to anterior border of heart/trachea.
- Contents: Thymus, lymph nodes, internal mammary vessels.
- 📌 Mnemonic (Masses): The 4 T's - Thymoma, Terrible lymphoma, Teratoma, Thyroid (ectopic).
- Middle: Contains heart, pericardium, great vessels, trachea, main bronchi, phrenic nerves.
- Posterior: Behind the heart/trachea, before the vertebral column.
- Contents: Esophagus, descending aorta, vagus nerves, thoracic duct.
- Anterior: From sternum to anterior border of heart/trachea.
⭐ High-Yield: The phrenic nerve runs anterior to the lung hilum, while the vagus nerve runs posterior to it. (Mnemonic: AP = Anterior Phrenic).
🩺 Clinical Manifestations - Compressive Syndromes
- Superior Vena Cava (SVC) Syndrome: Facial/neck swelling (plethora), jugular venous distention (JVD), headache, dilated chest wall veins.
- 💡 Pemberton's sign: Facial flushing/JVD on raising arms.
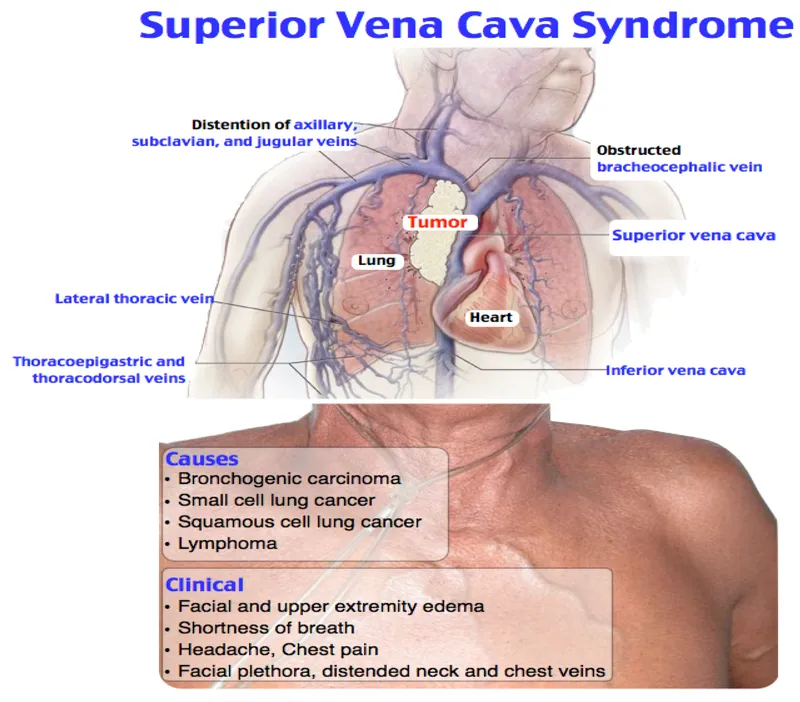
- Airway Compression: Dyspnea, cough, stridor, wheezing. Symptoms may worsen when supine.
- Esophageal Compression: Dysphagia (solids > liquids).
- Nerve Compression:
- Recurrent Laryngeal: Hoarseness.
- Phrenic: Diaphragmatic paralysis (elevated hemidiaphragm on CXR), dyspnea.
- Sympathetic Chain: Horner's Syndrome (ptosis, miosis, anhidrosis).
⭐ Malignancy (e.g., lung cancer, lymphoma) is the cause of SVC syndrome in >80% of cases.
🩺 Diagnosis - The Workup Algorithm
- Initial Imaging: Chest X-ray (often incidental finding) → CT chest with IV contrast is the gold standard to delineate mass location, size, and characteristics (e.g., cystic, solid, vascularity, invasion).
- Biochemical Markers: Guided by CT location.
- Anterior: Serum AFP and β-hCG for suspected germ cell tumors.
- Posterior: Urine/plasma metanephrines for suspected neurogenic tumors (paraganglioma).
- Thymoma suspicion: Acetylcholine receptor (AChR) antibodies for myasthenia gravis.
⭐ Pure seminomas may have an elevated β-hCG, but NEVER an elevated AFP. If AFP is elevated, it signifies a non-seminomatous germ cell tumor (NSGCT) component.
🔪 Management - Treatment Blueprints
-
General Principle: Treatment is histology-dependent. Biopsy is key before definitive therapy, unless resection is both diagnostic and therapeutic (e.g., suspected benign cyst).
-
Anterior Mediastinum:
- Thymoma: Complete surgical resection. Pre-op optimization for Myasthenia Gravis (if present).
- Germ Cell Tumors (GCTs):
- Seminoma: Primarily radiation/chemotherapy.
- Non-seminoma: Chemotherapy (e.g., BEP) followed by surgical resection of any residual mass.
- Lymphoma: Chemotherapy +/- Radiation. ⚠️ Surgery is for biopsy ONLY.
-
Middle & Posterior Mediastinum:
- Symptomatic Cysts (Bronchogenic, Pericardial): Surgical resection.
- Neurogenic Tumors: Complete surgical resection.
⭐ For suspected lymphoma, an excisional biopsy (e.g., via mediastinoscopy) is preferred over fine-needle aspiration (FNA) to preserve lymph node architecture for accurate subtyping.
⚡ Biggest Takeaways
- The anterior mediastinum is home to the "4 T's": Thymoma, Teratoma (GCTs), ectopic Thyroid, and "Terrible" Lymphoma.
- Always associate thymoma with Myasthenia Gravis; check for AChR antibodies.
- Evaluate suspected germ cell tumors with serum AFP and β-hCG.
- Posterior mediastinal masses are overwhelmingly neurogenic tumors (e.g., schwannoma).
- The middle mediastinum contains lymphadenopathy (lymphoma, sarcoidosis) and congenital cysts.
- CT with contrast is the primary imaging modality; definitive management is often surgical resection, except for lymphoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

