🧬 Core principles - The Heart's Blueprint
- Shunt Physiology:
- Left-to-Right (L→R): Acyanotic. ↑ Pulmonary blood flow. Examples: VSD, ASD, PDA.
- Right-to-Left (R→L): Cyanotic. Deoxygenated blood bypasses lungs.
- 📌 5 T's of Cyanotic CHD: Tetralogy of Fallot, Transposition, Tricuspid atresia, Truncus arteriosus, TAPVR.
- Surgical Goals:
- Palliative: Temporizing procedures to optimize physiology (e.g., Blalock-Taussig shunt).
- Corrective: Definitive anatomical repair (e.g., VSD patch closure).
- Key Metric: Pulmonary-to-Systemic Flow Ratio ($Q_p/Q_s$). Ideal is 1:1.
⭐ Eisenmenger Syndrome: A severe form of pulmonary hypertension from a chronic, large L→R shunt. The shunt reverses to R→L, causing late-onset cyanosis and making corrective surgery contraindicated.
💨 Pathophysiology - Shunts & Swirls
- Shunt: Abnormal blood flow between cardiac chambers/vessels, driven by pressure gradients.
- Left-to-Right (L→R) Shunt (Acyanotic)
- Pathophysiology: Oxygenated blood from high-pressure left heart shunts to low-pressure right heart.
- Result: ↑ Pulmonary Blood Flow (PBF) → Pulmonary HTN → RV Hypertrophy → heart failure.
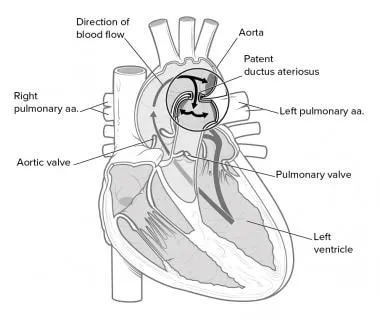
- Examples: VSD, ASD, PDA. Acyanotic at birth.
- Right-to-Left (R→L) Shunt (Cyanotic)
- Pathophysiology: Deoxygenated blood bypasses lungs into systemic circulation.
- Result: Systemic hypoxemia, causing early cyanosis ("blue babies").
- Examples: Tetralogy of Fallot (TOF), Transposition of Great Arteries (TGA).
- 📌 5 T's: TOF, TGA, Truncus arteriosus, Tricuspid atresia, TAPVR.
⭐ Eisenmenger Syndrome: Chronic L→R shunt causes severe pulmonary HTN, reversing flow to R→L. Results in late-onset cyanosis, making the defect inoperable.
- Quantifying Shunts (Qp:Qs Ratio):
- Normal: Qp:Qs ≈ 1:1
- L→R Shunt: Qp:Qs > 1.5 (significant)
- R→L Shunt: Qp:Qs < 1
🩺 The Surgical Toolkit
-
Palliative Procedures: Temporize until definitive repair.
- Systemic-to-Pulmonary Shunt: ↑ Pulmonary Blood Flow (PBF) in cyanotic defects (e.g., ToF, Tricuspid Atresia).
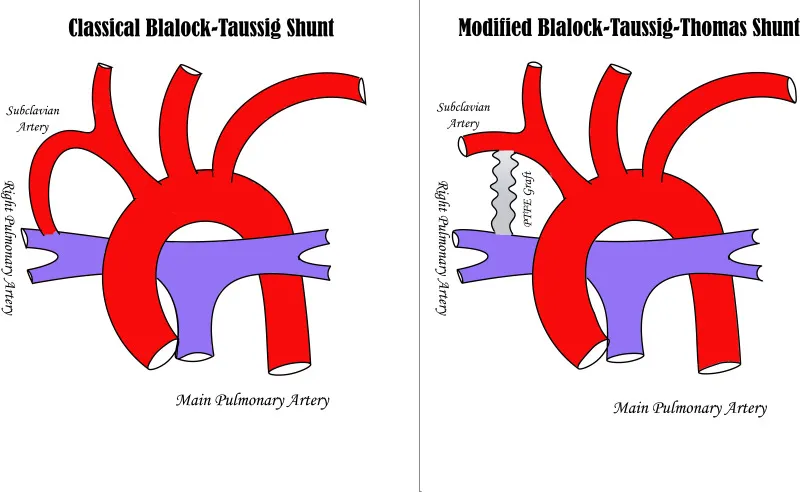
- 📌 Blalock-Taussig-Thomas (BTT): Subclavian artery to pulmonary artery.
- Pulmonary Artery (PA) Banding: ↓ PBF to protect lungs from pulmonary HTN in large L→R shunts (e.g., VSD).
- Systemic-to-Pulmonary Shunt: ↑ Pulmonary Blood Flow (PBF) in cyanotic defects (e.g., ToF, Tricuspid Atresia).
-
Corrective Procedures: Definitive anatomical repair.
- Patch Closure: For ASD, VSD.
- Arterial Switch (Jatene): For D-TGA.
- Rastelli Procedure: For TGA with VSD & LVOTO.
⭐ The Fontan circulation is a passive system where systemic venous return bypasses the ventricle, flowing directly to the pulmonary arteries. Success is critically dependent on low pulmonary vascular resistance (PVR).
⚠️ Complications - Post-Op Perils
- Low Cardiac Output Syndrome (LCOS): Most common cause of early mortality. Features: hypotension, oliguria, ↑lactate. Treat with inotropes (e.g., milrinone).
- Cardiac Tamponade: Sudden ↓ chest tube output with ↑CVP & hypotension (Beck's triad). Requires emergent sternotomy.
- Pulmonary: Atelectasis, pleural effusions, chylothorax (thoracic duct injury → milky fluid, ↑triglycerides).
- Neurologic/Renal: Stroke from cardiopulmonary bypass (CPB) emboli; Acute Kidney Injury (AKI) from hypoperfusion.
⭐ Junctional Ectopic Tachycardia (JET) is a high-risk, narrow-complex tachycardia, especially after VSD repair. Key sign: AV dissociation.
⚡ Biggest Takeaways
- L→R shunts (VSD, ASD, PDA) are acyanotic but risk Eisenmenger syndrome (shunt reversal, late cyanosis) from chronic pulmonary overcirculation.
- R→L shunts (e.g., Tetralogy of Fallot, TGA) cause early cyanosis by shunting deoxygenated blood systemically.
- Prostaglandin E1 (PGE1) is a critical pre-op bridge to maintain a patent ductus arteriosus (PDA) in ductal-dependent lesions.
- Palliative shunts (e.g., Blalock-Taussig) temporarily increase pulmonary blood flow in cyanotic defects.
- Cardiopulmonary bypass (CPB) is required for most definitive intracardiac repairs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

