🗺️ Pathology - Staging the Enemy
-
TNM Staging (AJCC 8th Ed.) is the cornerstone for prognosis and treatment planning.
-
T (Tumor Size):
- T1: ≤ 2 cm
- T2: > 2 cm to ≤ 5 cm
- T3: > 5 cm
- T4: Any size with direct extension to chest wall/skin (e.g., ulceration, edema/peau d'orange), or inflammatory breast cancer.
-
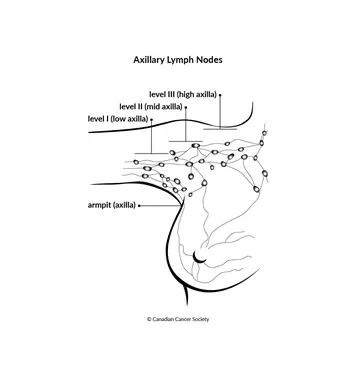
N (Nodal Status):
- Clinically node-negative: Sentinel Lymph Node Biopsy (SLNB) is standard.
- Clinically node-positive: Axillary Lymph Node Dissection (ALND).
⭐ Axillary lymph node status is the single most important prognostic factor in early-stage breast cancer.
-
M (Metastasis):
- M0: No distant spread.
- M1: Distant spread (bone, lung, liver, brain).
🎀 Breast Cancer Staging & Surgical Management
-
Staging (TNM):
- T (Tumor): T1 (≤2cm), T2 (>2-5cm), T3 (>5cm), T4 (chest wall/skin, inflammatory).
- N (Nodes): Sentinel Lymph Node Biopsy (SLNB) for clinically node-negative axilla. Axillary Lymph Node Dissection (ALND) for positive SLNB or clinically positive nodes.
- M (Metastasis): M1 indicates distant disease (Stage IV), typically managed non-surgically first.
-
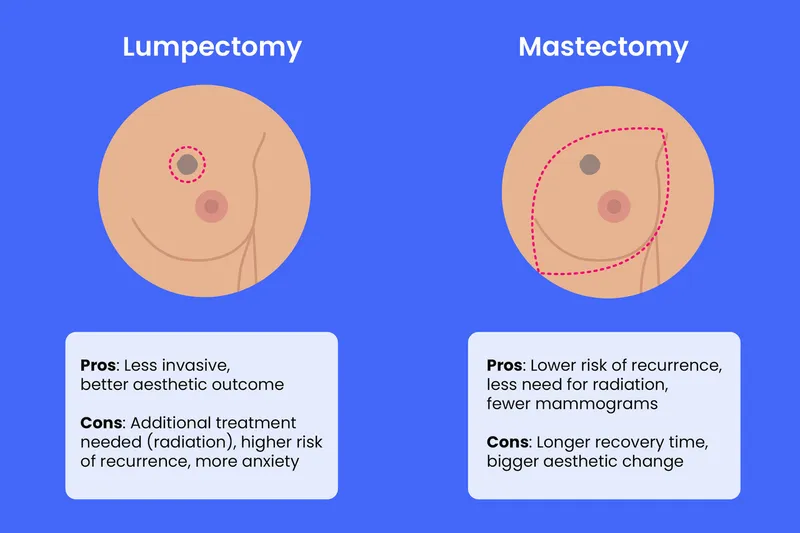
Surgical Decision-Making:
- Breast Conserving Surgery (BCS): Lumpectomy + SLNB. Requires adjuvant radiation to reduce local recurrence.
- Mastectomy: Removal of breast tissue ± SLNB/ALND. Radiation may still be needed for large tumors or positive nodes.
⭐ For early-stage breast cancer (Stage I/II), BCS followed by radiation therapy offers equivalent survival rates to mastectomy.
🔪 Axillary Dissection Details
-
Axillary Lymph Node Levels: Defined by relation to pectoralis minor muscle.
- Level I: Lateral to the muscle's lateral border.
- Level II: Posterior/deep to the muscle.
- Level III: Medial to the muscle's medial border.
-
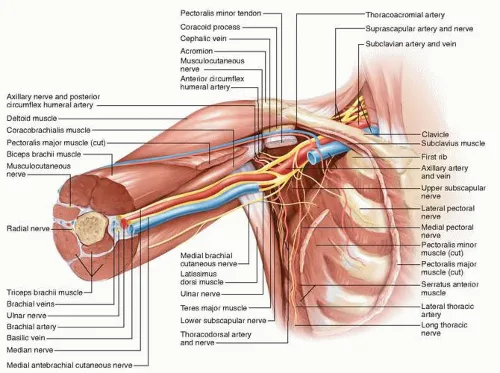
Nerves at Risk & Deficits:
- Long Thoracic N.: Runs on serratus anterior. Injury → winged scapula (impaired arm abduction >90°).
- Thoracodorsal N.: Travels with thoracodorsal artery. Injury → weak arm adduction, extension, internal rotation.
- Intercostobrachial N.: Sensory nerve. Injury → numbness/paresthesia of medial arm/axilla.
⭐ The intercostobrachial nerve is the most frequently injured nerve during axillary dissection, leading to sensory loss, not motor deficit.
⚠️ Complications - Post-Op Pitfalls
- Lymphedema: Chronic, non-pitting edema of the ipsilateral arm. Major risk with Axillary Lymph Node Dissection (ALND); significantly lower with SLNB. Management: compression, physical therapy.
- Nerve Injury (during ALND):
- Long Thoracic n.: Serratus anterior palsy → "winged scapula".
- Thoracodorsal n.: Latissimus dorsi weakness → weak arm adduction/internal rotation.
- Other: Seroma, hematoma, surgical site infection, chronic pain (post-mastectomy pain syndrome).
⭐ The intercostobrachial nerve is most commonly injured during axillary dissection, causing sensory loss to the medial arm and axilla.
⚡ Biggest Takeaways
- TNM staging dictates prognosis; metastasis (M) is the most critical factor.
- Sentinel lymph node biopsy (SLNB) is the standard for axillary staging in clinically node-negative patients.
- Axillary lymph node dissection (ALND) is reserved for positive SLNB or clinically positive nodes.
- Breast-conserving therapy (BCT)-lumpectomy + radiation-offers equivalent survival to mastectomy for early-stage disease.
- Mastectomy is indicated for large tumors, multicentric disease, or contraindications to radiation.
- Stage IV disease management is primarily systemic therapy, not curative surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

