💊 Drug class/MOA - The Analgesic Arsenal
- NSAIDs/Acetaminophen:
- NSAIDs: Inhibit COX-1/2 enzymes, reducing prostaglandin synthesis.
- Acetaminophen: Weak, reversible COX inhibitor, primarily in the CNS.
- Opioids (e.g., Morphine, Fentanyl):
- Agonists at μ-opioid receptors (GPCRs) in CNS and periphery.
- Local Anesthetics (e.g., Lidocaine):
- Block voltage-gated Na⁺ channels, preventing nerve impulse propagation.
- Adjuvants:
- Gabapentinoids: Block presynaptic voltage-gated Ca²⁺ channels (α2δ subunit).
- Ketamine: Non-competitive NMDA receptor antagonist.
⭐ Gabapentinoids (Gabapentin, Pregabalin) are first-line for neuropathic pain, like diabetic neuropathy or postherpetic neuralgia.
🎯 Clinical Uses - Targeting the Pain
- Multimodal approach is standard of care. Use agents with different mechanisms.
- Nociceptive Pain (Somatic/Visceral): Responds well to NSAIDs, acetaminophen, and opioids.
- Neuropathic Pain: First-line are adjuvants.
- Gabapentinoids (Gabapentin, Pregabalin).
- TCAs (Amitriptyline), SNRIs (Duloxetine).
- Regional Anesthesia: Nerve blocks & epidurals provide potent, localized pain control, reducing systemic opioid needs.
⭐ WHO Analgesic Ladder: A stepwise approach for cancer/chronic pain. Start with non-opioids, add weak opioids for moderate pain, then strong opioids for severe pain. Adjuvants can be used at any step.
💊 Adverse Effects - The Side Effect Slate
| Drug Class | Key Adverse Effects |
|---|---|
| Opioids | Respiratory depression, sedation, constipation, miosis, N/V, pruritus |
| NSAIDs | GI ulcers/bleeding, acute kidney injury (afferent constriction), platelet dysfunction |
| Acetaminophen | Hepatotoxicity (overdose; toxic metabolite NAPQI) |
| Local Anesthetics | CNS toxicity (seizures), cardiotoxicity (arrhythmias), methemoglobinemia |
| Gabapentinoids | Sedation, dizziness, ataxia, peripheral edema |
💉 Management - Blocks, Pumps, & More
- Regional/Nerve Blocks: Local anesthetic (e.g., bupivacaine) injected near a nerve/plexus (e.g., brachial, femoral) under ultrasound guidance. Provides targeted, opioid-sparing analgesia.
- Neuraxial Anesthesia:
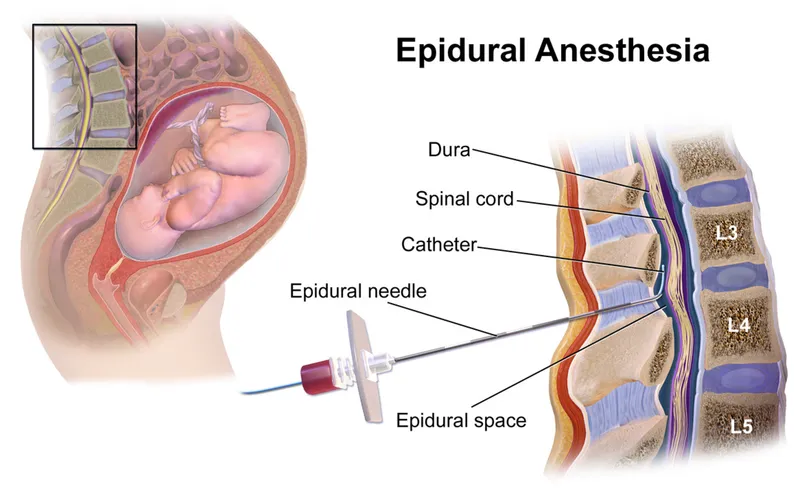
- Epidural: Catheter in epidural space for continuous infusion. Slower onset; ideal for labor or prolonged post-op pain.
- Spinal: Single injection into subarachnoid space. Rapid, dense block. ⚠️ Risk: Post-dural puncture headache (PDPH), hypotension.
- Patient-Controlled Analgesia (PCA): IV pump for patient-administered opioid boluses with a programmed lockout interval to prevent overdose.
⭐ PCA pumps require vigilant monitoring for respiratory depression, especially in opioid-naïve patients, the elderly, or those with obstructive sleep apnea (OSA).
⚠️ Complications - When Relief Goes Wrong
-
Opioids
- Acute: Respiratory depression (most feared), sedation, miosis, constipation, nausea/vomiting, pruritus, urinary retention.
- Drug Interaction: ⚠️ Serotonin syndrome risk with tramadol/meperidine + SSRIs/MAOIs.
- Chronic: Tolerance, dependence, opioid-induced hyperalgesia, Opioid Use Disorder (OUD).
-
NSAIDs & Acetaminophen
- NSAIDs: GI bleeding/ulcers, acute kidney injury (afferent constriction), ↑ cardiovascular risk (MI/stroke).
- Acetaminophen: Hepatotoxicity in overdose (toxic metabolite NAPQI).
-
Regional Anesthesia (Epidural/Spinal)
- Common: Hypotension (sympathectomy), post-dural puncture headache (PDPH).
- Rare but Severe: Epidural hematoma, epidural abscess, nerve damage, Local Anesthetic Systemic Toxicity (LAST).
⭐ Epidural Hematoma: A neurosurgical emergency. Suspect in patients on anticoagulants post-procedure with new motor/sensory deficits or bowel/bladder dysfunction. Requires urgent MRI and decompression.
⚡ Biggest Takeaways
- Opioids (morphine) are μ-agonists; key risks are respiratory depression and constipation. Antidote: naloxone.
- NSAIDs (ketorolac) inhibit COX, risking GI bleeds and renal injury. Contraindicated in CKD.
- Acetaminophen overdose causes hepatotoxicity (treat with N-acetylcysteine); a key part of multimodal analgesia.
- Local anesthetics (lidocaine) block Na+ channels. Bupivacaine has significant cardiotoxicity risk.
- Regional techniques (epidurals, nerve blocks) are opioid-sparing and offer superior analgesia.
- Ketamine (NMDA antagonist) is effective for opioid-tolerant patients and chronic pain syndromes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

