Relapse Prevention - The Ground Rules
- Goal: Move from acute stabilization to stable remission by equipping patients to handle high-risk situations.
- Core Models:
- Cenaps Model (Gorski): Views relapse as a progression of warning signs.
- Cognitive-Behavioral Model (Marlatt): Focuses on coping skills in high-risk situations.
- Abstinence Violation Effect (AVE): A minor slip (lapse) leads to guilt & perceived loss of control, escalating to a full-blown relapse. This is often driven by "all-or-nothing" thinking.
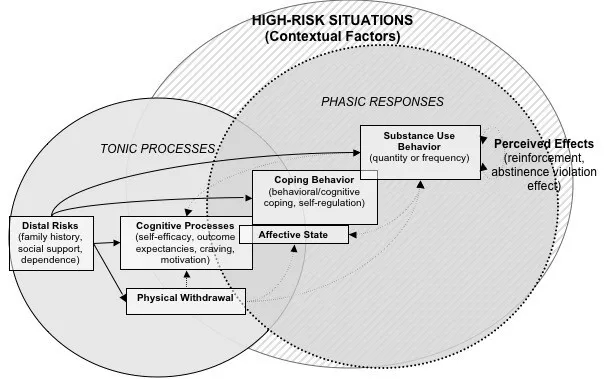
⭐ High-Yield Fact: The most common triggers for relapse are negative emotional states (e.g., frustration, anger, depression), interpersonal conflict, and social pressure.
Psychosocial Strategies - Talk It Through
-
Cognitive Behavioral Therapy (CBT): The cornerstone of relapse prevention.
- Goal: Identify and modify maladaptive thoughts, feelings, and behaviors linked to substance use.
- Core Technique: Functional analysis of substance use (triggers, thoughts, consequences).
- Develops coping skills for high-risk situations and cravings.
-
Motivational Interviewing (MI): A collaborative conversation style for strengthening a person’s own motivation and commitment to change.
- 📌 OARS Core Skills: Open-ended questions, Affirmations, Reflective listening, Summaries.
-
Support Groups (AA/NA): Peer-led, 12-step programs providing fellowship and accountability.
-
Contingency Management: Uses positive reinforcement (e.g., vouchers) for objective evidence of abstinence.
⭐ Exam Favorite: Contingency management is highly effective, especially for stimulant (cocaine, amphetamine) use disorders, by providing tangible rewards for maintaining abstinence.
Pharmacotherapy - The Chemical Shield
-
Alcohol Use Disorder
- Naltrexone: Reduces cravings & the rewarding "buzz" (μ-opioid antagonist).
- Acamprosate (Campral): Restores GABA/glutamate balance. Ideal for post-detoxification maintenance.
- Disulfiram (Antabuse): Aversive therapy. Inhibits aldehyde dehydrogenase → acetaldehyde buildup. ⚠️ Requires high motivation.
-
Opioid Use Disorder
- Naltrexone: Blocks euphoric effects. Must be opioid-free for 7-10 days.
- Buprenorphine (+ Naloxone): Partial μ-agonist with a ceiling effect on respiratory depression.
- Methadone: Long-acting full μ-agonist. Dispensed via licensed programs. ⚠️ Monitor for QTc prolongation.
-
Nicotine Use Disorder
- Varenicline (Chantix): Partial nicotinic receptor agonist. Most effective monotherapy.
- Bupropion (Zyban): NDRI antidepressant.
- 📌 Mnemonic: "He CAN't smoke": Campral, Antabuse, Naltrexone for alcohol.
⭐ Exam Favorite: Always ensure a patient is opioid-free for at least 7-10 days before starting naltrexone to avoid severe, precipitated withdrawal symptoms. This is a critical safety step.
High‑Yield Points - ⚡ Biggest Takeaways
- Relapse is an expected part of recovery, not a failure; the goal is to re-engage with treatment and learn from the event.
- Use the HALT mnemonic to identify high-risk situations: Hungry, Angry, Lonely, and Tired.
- Cognitive Behavioral Therapy (CBT) is key to developing coping skills and changing maladaptive behaviors.
- Contingency management uses positive reinforcement to maintain abstinence.
- Support groups like AA/NA provide essential peer support.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

