Extrapyramidal Symptoms - The Unwanted Moves
- Timeline: 📌 ADAP-Tive response: Acute Dystonia → Akathisia → Parkinsonism → Tardive Dyskinesia.
- Pathophysiology: Dopamine ($D_2$) blockade in the nigrostriatal pathway.
- Acute Dystonia (hours-days): Sudden, sustained muscle contractions. Torticollis, oculogyric crisis.
- Akathisia (days-weeks): Subjective restlessness; inability to stay still.
- Parkinsonism (weeks-months): Bradykinesia, cogwheel rigidity, resting tremor.
- Tardive Dyskinesia (months-years): Involuntary choreoathetoid movements, esp. orofacial.
⭐ Exam Favourite: While anticholinergics (e.g., benztropine) treat most EPS, they can worsen or unmask Tardive Dyskinesia. Always assess for TD before prescribing.
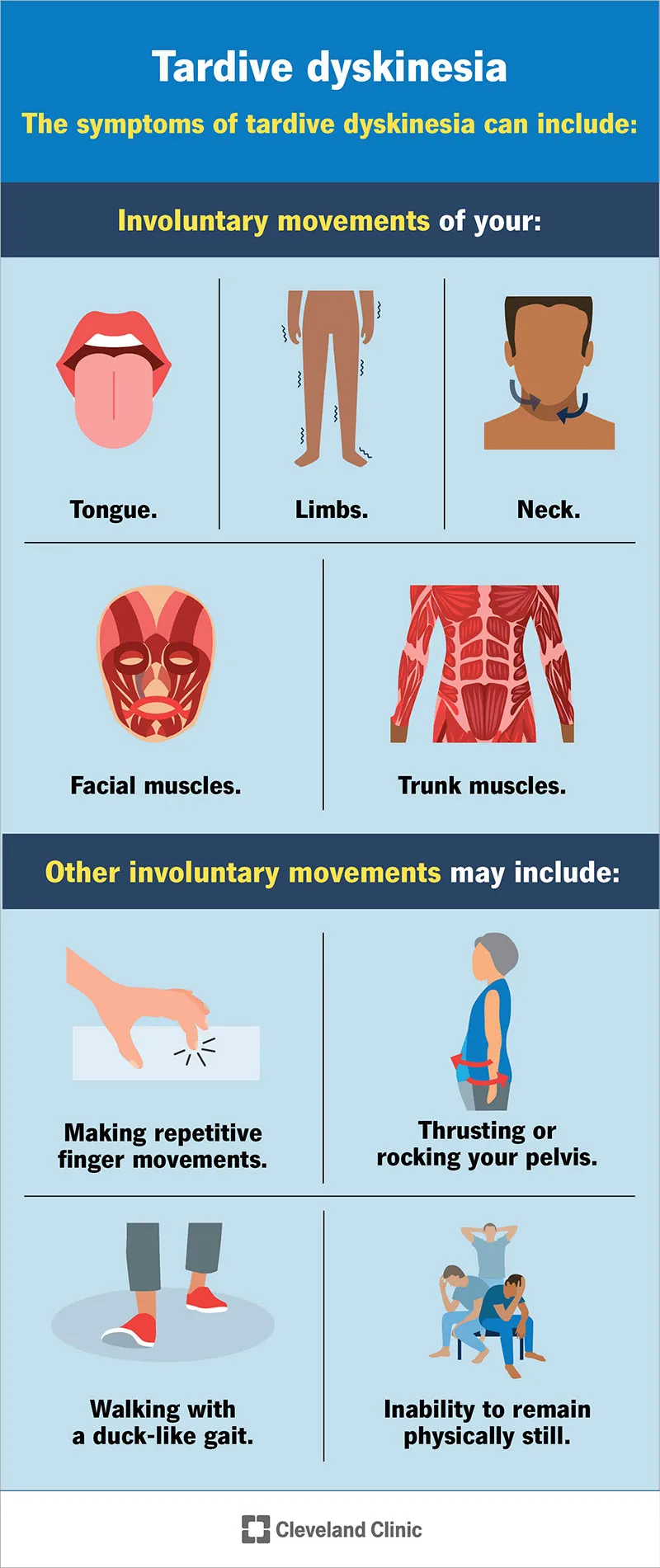
Tardive Dyskinesia - The Late Grimace
- Pathophysiology: Prolonged D2 blockade leads to dopamine receptor upregulation and supersensitivity.
- Clinical: Involuntary choreoathetoid movements, classically orofacial (lip-smacking, grimacing).
- Onset: Late-onset, typically after >6 months of exposure.
- Monitoring: Use the Abnormal Involuntary Movement Scale (AIMS) at baseline and regular intervals.
⭐ Key Fact: While stopping the drug is first-line, symptoms can be irreversible or may even worsen initially upon antipsychotic withdrawal.
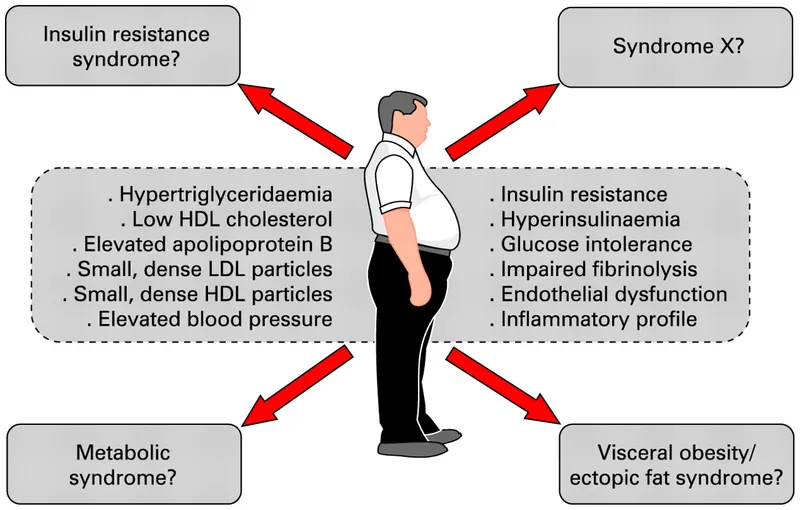
Metabolic Syndrome - The Weighty Sidekicks
Associated with Second-Generation Antipsychotics (SGAs), causing significant weight gain, dyslipidemia, and hyperglycemia.
- Highest Risk: Olanzapine, Clozapine (📌 Mnemonic: Old Clothes are weighty).
- Lower Risk: Aripiprazole, Ziprasidone.
- Monitoring Protocol:
- Baseline & regular checks of: BMI, fasting glucose, lipid panel, blood pressure.
- Weight check at every visit.
- Management:
- Switch to a lower-risk agent.
- Prioritize lifestyle modifications (diet/exercise).
- Consider adding metformin to mitigate weight gain & insulin resistance.
⭐ The risk is not uniform across all SGAs; olanzapine and clozapine carry the highest risk for metabolic disturbances.
Other Major Side Effects - The Rogue's Gallery
- Neuroleptic Malignant Syndrome (NMS): Life-threatening reaction to dopamine antagonists.
- 📌 FEVER: Fever, Encephalopathy, Vitals unstable, Elevated enzymes (CK), Rigidity ("lead pipe").
- Management:
-
Metabolic Syndrome: Common with atypicals (esp. olanzapine, clozapine).
- Monitor: Weight, BMI, fasting glucose, lipids.
-
Anticholinergic: Dry mouth, constipation, urinary retention, blurred vision.
-
Orthostatic Hypotension: Due to α1-blockade. Advise slow position changes.
-
Sedation: Due to histamine (H1) blockade.
⭐ NMS is an idiosyncratic reaction, not dose-dependent, and can occur any time during treatment. Mortality is 5-20%.
- Acute dystonia (torticollis, oculogyric crisis) is an emergency managed with benztropine or diphenhydramine.
- For akathisia (restlessness), beta-blockers (propranolol) are first-line, followed by benzodiazepines.
- Treat drug-induced parkinsonism (bradykinesia, tremor) with anticholinergics like benztropine or amantadine.
- For Tardive Dyskinesia (TD), the key is to switch to clozapine or use a VMAT2 inhibitor.
- NMS is a medical emergency: stop the antipsychotic, provide supportive care, and administer dantrolene or bromocriptine.
- Manage metabolic syndrome by monitoring lipids/glucose and switching to weight-neutral agents like aripiprazole.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

