ADHD Pathophysiology - Brain's Busy Wires
- Core Deficit: Dysregulation of catecholamine neurotransmission, primarily Dopamine (DA) and Norepinephrine (NE).
- Key Brain Circuits & Functions:
- Prefrontal Cortex (PFC): ↓ DA & NE activity impairs executive functions → inattention, hyperactivity, impulsivity.
- Basal Ganglia (Striatum): Altered DA signaling disrupts reward pathways & motivation.
- Limbic System (Amygdala/Cingulate): Involved in emotional dysregulation.
- Cerebellum: Contributes to deficits in timing, coordination, and motor control.
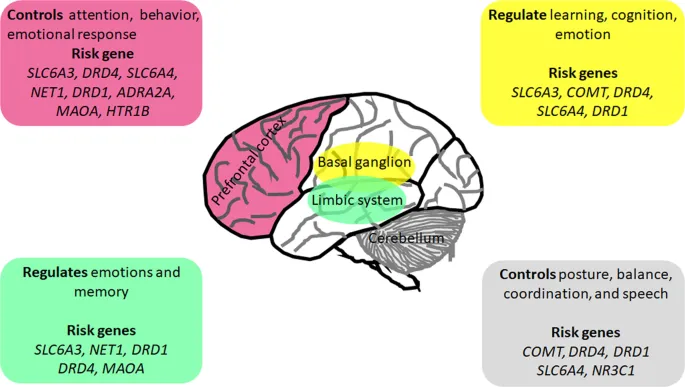
⭐ Brain imaging studies often show a higher density of dopamine transporters (DAT) in the striatum of individuals with ADHD. This leads to excessive reuptake of dopamine from the synapse, reducing its availability.
Key Neurotransmitters - The Dopamine & NE Show
ADHD pathophysiology centers on catecholamine dysregulation, primarily Dopamine (DA) and Norepinephrine (NE), impacting prefrontal cortex (PFC) function.
-
Dopamine (DA): The "Motivation Molecule"
- Functions: Governs reward, motivation, and sustained focus.
- Deficit Impact: Leads to impulsivity, poor self-regulation, and a constant search for rewarding stimuli (novelty-seeking).
-
Norepinephrine (NE): The "Vigilance Vibe"
- Functions: Modulates attention, arousal, vigilance, and executive functions.
- Deficit Impact: Results in inattention, distractibility, and impaired planning/organization.
⭐ Exam Favorite: Structural neuroimaging in ADHD often reveals decreased brain volume in the prefrontal cortex and basal ganglia.

Neuroanatomy - The Control Network
ADHD involves dysfunction in key brain networks responsible for executive control and attention.
- Prefrontal Cortex (PFC): Exhibits ↓ volume and hypoactivation, particularly in the dorsolateral PFC (dlPFC) and anterior cingulate cortex (ACC).
- Clinical link: Correlates with core executive dysfunctions: poor planning, impaired working memory, and weak impulse control.
- Basal Ganglia (Striatum): Reduced volume, especially in the caudate nucleus. Dysfunctional fronto-striatal circuits impair dopamine-rich reward pathways.
- Clinical link: Underlies motivation deficits, impulsivity, and hyperactivity.
- Cerebellum: Smaller volume, particularly the vermis. Contributes to poor motor coordination and emotional dysregulation.

⭐ A key finding is the failure of the PFC to suppress the Default Mode Network (DMN), which is normally active during rest. This results in characteristic attention lapses and mind-wandering.
Neuroimaging Findings - Brain Scan Snapshots
- Structural (sMRI):
- ↓ Total cerebral volume & cortical thickness (esp. prefrontal cortex).
- Smaller volumes in key subcortical structures: basal ganglia (caudate, putamen) and corpus callosum.
- Functional (fMRI):
- Hypoactivation (↓ activity) in the frontal-striatal networks during executive function & attention tasks.
- Altered connectivity in the Default Mode Network (DMN), linked to attention lapses.
⭐ Delayed cortical maturation is a key finding; the prefrontal cortex, crucial for executive functions, shows a developmental lag of up to 3 years in children with ADHD compared to peers.

High‑Yield Points - ⚡ Biggest Takeaways
- ADHD neurobiology centers on dopamine (DA) and norepinephrine (NE) dysregulation, primarily in the prefrontal cortex (PFC).
- Key affected brain circuits involve the fronto-striatal and mesocorticolimbic pathways, impacting executive function and reward processing.
- Neuroimaging often shows a smaller brain volume, particularly in the PFC and basal ganglia (specifically the striatum).
- A strong genetic component is evident, with high heritability rates for the disorder.
- Stimulant medications effectively increase synaptic DA and NE, targeting these core neurochemical imbalances.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

