Galactosemia & Fructose Intolerance - Toxic Treats
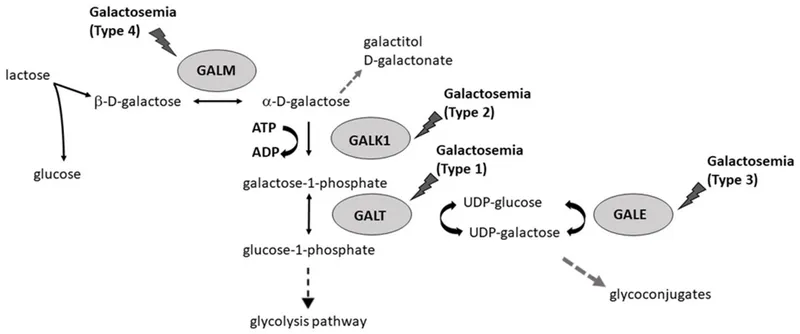
- Galactosemia: AR. Impaired galactose metabolism.
- Classic (GALT deficiency): Most common/severe. Galactose-1-P & galactitol accumulate.
- Features: Jaundice, hepatomegaly, vomiting, FTT, cataracts (oil-droplet), E. coli sepsis, developmental delay.
- Dx: ↑Blood galactose, urine reducing substances (+ve, non-glucose), ↓GALT activity (RBCs).
- Rx: Lifelong galactose-free (lactose-free) diet.
- GALK deficiency: Cataracts.
- GALE deficiency: Variable severity.
- Classic (GALT deficiency): Most common/severe. Galactose-1-P & galactitol accumulate.
- Hereditary Fructose Intolerance (HFI): AR. Aldolase B deficiency.
- Fructose-1-P accumulates → inhibits gluconeogenesis/glycogenolysis.
- Features (post fructose/sucrose/sorbitol): Severe hypoglycemia, vomiting, hepatomegaly, jaundice, FTT.
- Aversion to sweets.
- Dx: History, enzyme assay (liver), DNA. Urine reducing substances (+ve post-fructose).
- Rx: Avoid fructose, sucrose, sorbitol.
⭐ Classic Galactosemia: Despite diet, long-term risks include ovarian failure (females) & developmental delays.
Key GSDs (Von Gierke, Pompe) - Stash & Crash
Impaired glycogen metabolism leads to glycogen "stash" (accumulation) and systemic "crash" (dysfunction).
-
Von Gierke (GSD Type Ia): Liver Stash, Glucose Crash
- Enzyme: ↓Glucose-6-phosphatase (liver, kidney).
- Stash: Glycogen in liver & kidney → massive hepatomegaly, renomegaly.
- Crash: Severe fasting hypoglycemia (seizures), lactic acidosis, hyperuricemia, hyperlipidemia.
- Features: Doll-like facies, protuberant abdomen.
- Rx: Frequent feeds, uncooked cornstarch. Avoid fructose/galactose.
-
Pompe (GSD Type II): Lysosomal Stash, Muscle/Heart Crash
- Enzyme: ↓Lysosomal acid $\alpha$-1,4-glucosidase (acid maltase).
- Stash: Glycogen in lysosomes (all tissues, esp. heart, muscle).
- Crash:
- Infantile: Cardiomyopathy (massive cardiomegaly), profound hypotonia ("floppy baby"), respiratory failure. Death <2 yrs if untreated.
- Late-onset: Progressive muscle weakness, respiratory insufficiency.
- Rx: Enzyme Replacement Therapy (ERT).

⭐ In Von Gierke disease, uncooked cornstarch provides a slow-release form of glucose, crucial for preventing nocturnal hypoglycemia.
📌 Mnemonic:
- Von Gierke: Very low Glucose.
- Pompe: Problems with the Pump (heart) & Posture (muscles).
Other GSDs (Cori, McArdle) & Dx - Fuel Failures
-
Cori Disease (GSD Type III; Forbes Disease; Debrancher Deficiency)
- Enzyme: Amylo-1,6-glucosidase (debranching enzyme).
- Clinical Features:
- Hepatomegaly, ketotic hypoglycemia (milder vs GSD I).
- Muscle weakness, hypotonia, growth retardation.
- Cardiomyopathy (type IIIa).
- Accumulation of limit dextrin (abnormally structured glycogen).
- Labs: ↑CK, AST, ALT. Normal lactate & uric acid.
- Rx: Frequent high-protein meals, uncooked cornstarch.
-
McArdle Disease (GSD Type V; Myophosphorylase Deficiency)
- Enzyme: Muscle glycogen phosphorylase (myophosphorylase).
- Clinical Features:
- Exercise intolerance, muscle cramps/pain, fatigue with intense exercise.
- "Second wind" phenomenon.
- Myoglobinuria (rhabdomyolysis risk).
- Labs: ↑CK (baseline & post-exercise). Ischemic exercise test: Venous lactate fails to rise >1.5x baseline.
- Rx: Oral sucrose before exercise. Avoid intense exercise. 📌 McArdle = Muscle.
⭐ In McArdle's (GSD V), the ischemic forearm exercise test shows a characteristic failure of blood lactate to rise, contrasting with a normal exaggerated rise in ammonia.
- General GSD Diagnostic Approach
- Suspect if: Hypoglycemia, hepatomegaly, muscle symptoms (weakness, cramps).
- Initial tests: Blood glucose, lactate, uric acid, lipids, LFTs, CK.
- Confirmatory:
- Specific enzyme assays (leukocytes, fibroblasts, tissue biopsy).
- Genetic testing.
- Biopsy (liver/muscle): Glycogen content & structure.

High‑Yield Points - ⚡ Biggest Takeaways
- Galactosemia (GALT deficiency): Cataracts, jaundice, hepatomegaly, E. coli sepsis; avoid galactose/lactose.
- Hereditary Fructose Intolerance (Aldolase B deficiency): Hypoglycemia, vomiting, jaundice after fructose/sucrose intake.
- Von Gierke's (GSD I): Severe fasting hypoglycemia, lactic acidosis, hepatomegaly, doll-like facies; Glucose-6-phosphatase defect.
- Pompe's (GSD II): Cardiomegaly, muscle weakness (hypotonia), macroglossia; lysosomal acid α-glucosidase defect.
- McArdle's (GSD V): Muscle cramps, myoglobinuria with exercise, "second wind"; muscle phosphorylase defect.
- Essential Fructosuria: Benign; fructokinase deficiency; fructose in urine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

