Mechanism of Action - Dopamine's Dance
-
Primary Action: Central blockade of dopamine D₂ receptors.
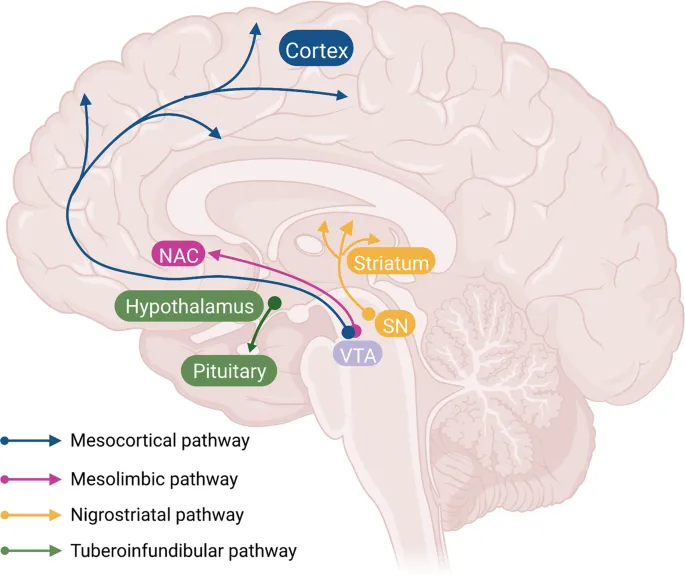
- Mesolimbic Pathway: ↓ Dopamine activity controls positive symptoms (mania, psychosis).
- Nigrostriatal Pathway: D₂ blockade → Extrapyramidal Symptoms (EPS) like parkinsonism, akathisia.
- Tuberoinfundibular Pathway: D₂ blockade → ↑ Prolactin, causing gynecomastia, galactorrhea.
- Mesocortical Pathway: Can sometimes worsen negative symptoms.
-
Atypical (SGA) Advantage: Additional serotonin 5-HT₂ₐ receptor blockade.
- This action ↑ dopamine release in the nigrostriatal tract, reducing the risk of EPS.
⭐ Therapeutic efficacy requires ~60-75% D₂ receptor occupancy; EPS risk sharply rises at >80%.
Indications & Agents - The Right Tool
- Acute Mania/Mixed Episodes: Used as monotherapy or adjunct to mood stabilizers (Lithium, Valproate) for rapid stabilization.
- Agents: Aripiprazole, Olanzapine, Quetiapine, Risperidone, Ziprasidone.
- Bipolar Depression: Crucial for treating depressive episodes without inducing mania.
- Agents: Lurasidone, Quetiapine, Cariprazine, and the Olanzapine-Fluoxetine Combination (OFC) are FDA-approved.
- Maintenance Therapy: Prevents recurrence. Long-acting injectables (LAIs) like Aripiprazole or Risperidone LAI boost adherence.
⭐ Lurasidone is notable for its efficacy in bipolar depression with a low risk of metabolic side effects and minimal weight gain, making it a favorable choice.
Adverse Effects - The Price of Stability
-
Metabolic Syndrome: Common with SGAs. Manifests as weight gain, dyslipidemia, and hyperglycemia.
- Highest risk: Olanzapine, Clozapine.
- Moderate risk: Risperidone, Quetiapine.
- Lower risk: Aripiprazole, Ziprasidone, Lurasidone.
- Monitoring: Check BMI, waist circumference, fasting glucose, and lipids at baseline and regularly.
-
Extrapyramidal Symptoms (EPS): Lower risk than FGAs but still present.
- Highest SGA risk with Risperidone, especially at doses >6 mg/day.
- Includes akathisia, parkinsonism, and dystonia.
- Tardive Dyskinesia (TD): A serious, long-term risk involving involuntary movements.
-
Other Key Effects:
- Hyperprolactinemia: Especially with Risperidone → gynecomastia, amenorrhea.
- Sedation: Prominent with Clozapine, Olanzapine, Quetiapine.
- ⚠️ Black Box Warning: Increased mortality in elderly patients with dementia-related psychosis.
⭐ For new-onset Tardive Dyskinesia, the standard of care is to treat with a VMAT2 inhibitor (e.g., valbenazine, deutetrabenazine) rather than just stopping the antipsychotic.

Clinical Monitoring - The Watchful Guardian
- Baseline & Periodic Checks:
- Weight (BMI), blood pressure
- Fasting glucose or HbA1c
- Fasting lipid panel
- Agent-Specific Monitoring:
- ECG: for QTc prolongation (ziprasidone)
- Prolactin: for hyperprolactinemia (risperidone)
- CBC: for agranulocytosis (clozapine)
⭐ All second-generation antipsychotics warrant vigilant screening for metabolic syndrome, a high-yield exam topic.
High-Yield Points - ⚡ Biggest Takeaways
- Atypical antipsychotics (e.g., olanzapine, quetiapine) are first-line for acute mania, often combined with mood stabilizers.
- Also used for maintenance therapy to prevent both manic and depressive episodes.
- The most significant side effect is metabolic syndrome; regularly monitor BMI, glucose, and lipids.
- Lower risk of extrapyramidal symptoms (EPS) than typicals, but tardive dyskinesia (TD) remains a concern.
- Lurasidone and the olanzapine-fluoxetine combination are approved for bipolar depression.
- Aripiprazole and ziprasidone carry a lower risk of metabolic side effects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

