Spirometry Basics - Lung Volume Vitals
- Lung Volumes (single measurements)
- Tidal Volume (TV): Air in a normal breath (~500 mL).
- Inspiratory Reserve Volume (IRV): Max air inhaled post-normal inspiration.
- Expiratory Reserve Volume (ERV): Max air exhaled post-normal expiration.
- Residual Volume (RV): Air left after max expiration.
- Lung Capacities (≥2 volumes)
- Inspiratory Capacity (IC): $IC = IRV + TV$
- Functional Residual Capacity (FRC): $FRC = ERV + RV$
- Vital Capacity (VC): $VC = IRV + TV + ERV$
- Total Lung Capacity (TLC): $TLC = VC + RV$
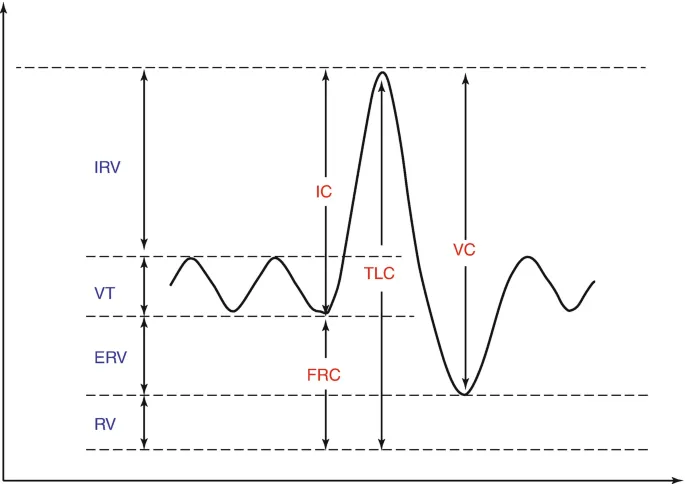
⭐ Residual Volume (RV) and, consequently, FRC and TLC, cannot be measured by simple spirometry. They require techniques like helium dilution or body plethysmography.
The Main Algorithm - Obstructive vs. Restrictive
-
Step 1: Check FEV₁/FVC Ratio
- The primary differentiator. Is the proportion of air exhaled in the first second reduced?
-
Step 2: Interpret the Ratio
- If FEV₁/FVC < 70%: Obstructive defect. Airflow is limited. Proceed to check FEV₁ to grade severity.
- If FEV₁/FVC ≥ 70%: Not obstructive. Now, check lung volumes.
-
Step 3: Evaluate FVC for Restriction
- If FVC is < 80% of predicted, suspect a Restrictive pattern. Reduced volume is key.
- Confirmation requires Total Lung Capacity (TLC) < 80%.
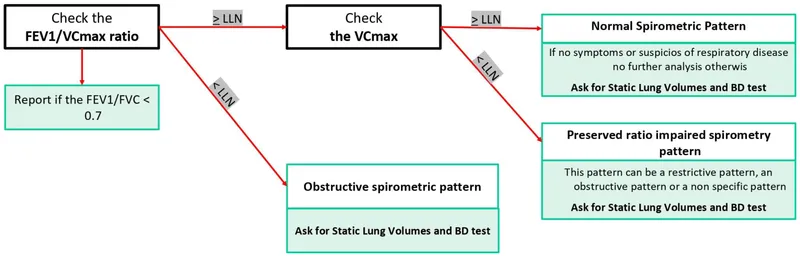
⭐ A "normal" or preserved FEV₁/FVC ratio in the presence of a low FVC and FEV₁ is characteristic of a restrictive pattern. Both volumes are reduced proportionally.
Flow-Volume Loops - Shape Shifters
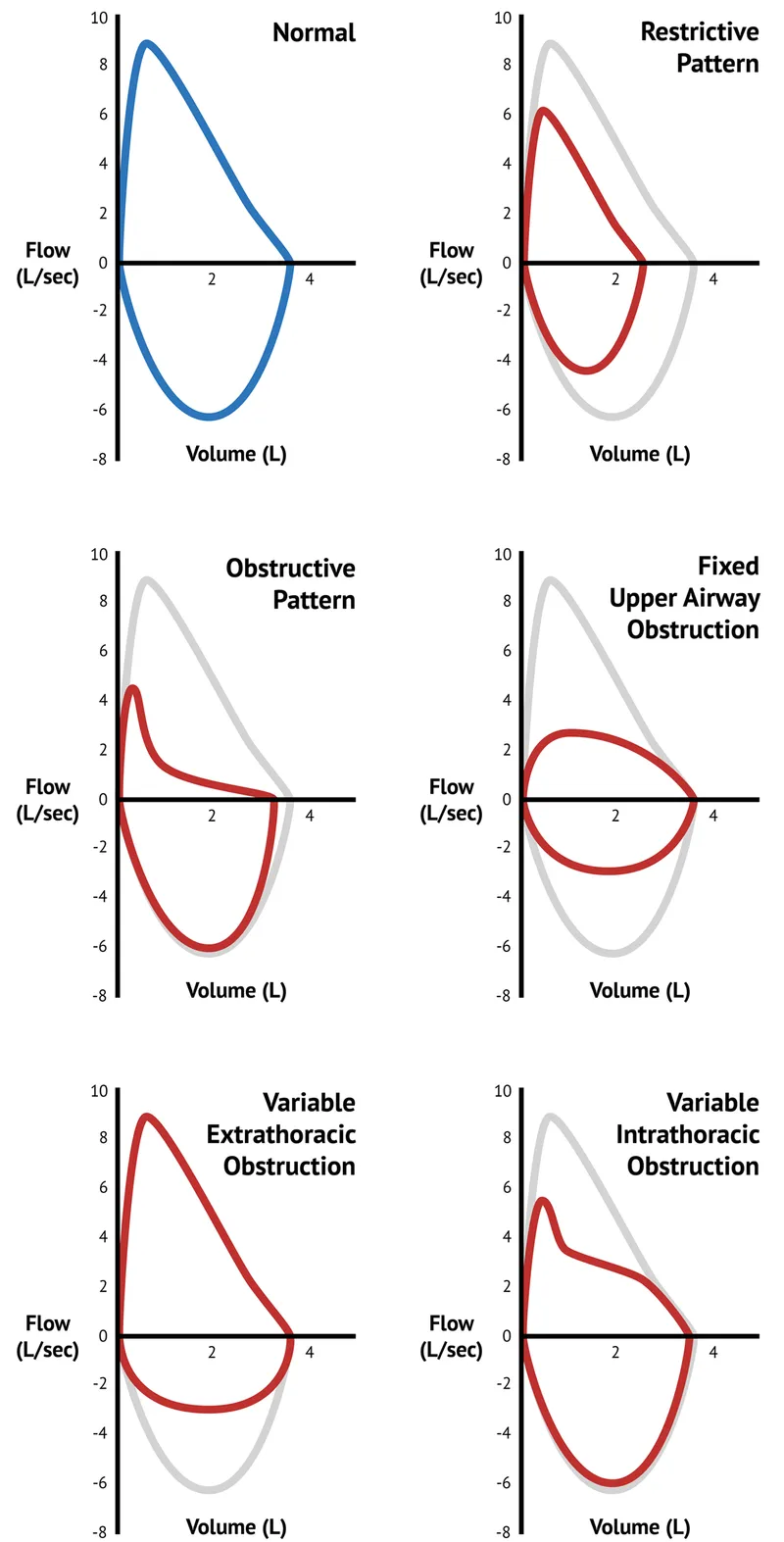
- Obstructive: Classic "scooped-out" expiratory limb from ↓ airflow.
- Restrictive: "Witch's hat" shape; a miniaturized, narrow loop shifted right due to low lung volumes.
- Upper Airway Obstruction:
- Fixed: Flattened top (expiration) and bottom (inspiration).
- Variable Extrathoracic: Flattened inspiratory limb.
- Variable Intrathoracic: Flattened expiratory limb.
- 📌 Mnemonic: Extrathoracic affects Inspiration; Intrathoracic affects Expiration.
⭐ The hallmark of obstructive disease is the "coved" or "scooped-out" shape of the expiratory limb.
Clinical Patterns - The Usual Suspects
Start with the FEV1/FVC ratio to differentiate patterns. A low ratio points to obstruction; a normal ratio with low lung volumes suggests restriction.
-
Obstructive Pattern (e.g., COPD, Asthma)
- Hallmark: ↓ FEV1/FVC (< 0.7)
- ↓ FEV1 is profound; FVC may be normal or ↓.
- TLC is often normal or ↑ (air trapping).
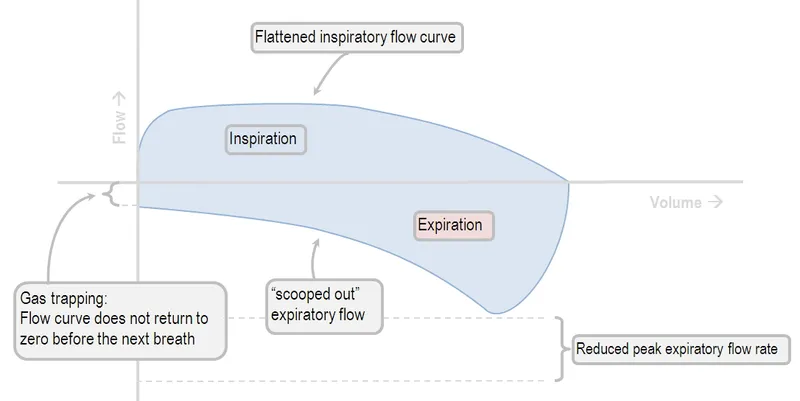
-
Restrictive Pattern (e.g., Fibrosis, Scoliosis)
- Hallmark: ↓ TLC is definitive.
- FEV1/FVC is normal or ↑ (≥ 0.7).
- Both FEV1 and FVC are reduced proportionally.
⭐ A post-bronchodilator increase in FEV1 or FVC by >12% AND >200 mL indicates significant reversibility, classic for Asthma.
High‑Yield Points - ⚡ Biggest Takeaways
- FEV1/FVC ratio is the key: < 70% suggests obstruction; ≥ 70% suggests restriction.
- Obstructive patterns show a disproportionately low FEV1. Severity is graded by FEV1.
- Restrictive patterns show a low FVC and TLC, with a normal or high FEV1/FVC ratio.
- Reversibility with a bronchodilator (>12% & 200 mL ↑ in FEV1/FVC) points to asthma.
- DLCO helps specify the cause: ↓ in emphysema/fibrosis, but normal in asthma or chronic bronchitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

