Receptor Input - Sensing the Strain
-
Chemoreceptors: Detect chemical changes in blood/CSF.
- Central (Medulla): Sense $\uparrow P_{CO_2}$ via changes in CSF $H^+$.
- Peripheral (Carotid/Aortic Bodies): Sense $\downarrow P_{O_2}$ (< 60 mmHg), $\uparrow P_{CO_2}$, and $\uparrow H^+$.
-
Mechanoreceptors: Gauge the mechanical work of breathing.
- Lungs: J-receptors (C-fibers) in interstitium are stimulated by edema or inflammation.
- Chest Wall: Muscle spindles & Golgi tendon organs signal respiratory muscle effort and fatigue.
⭐ In chronic hypercapnia (e.g., COPD), respiratory drive becomes less sensitive to $P_{CO_2}$, making the peripheral chemoreceptors' response to hypoxemia the primary stimulus for breathing.
Afferent Mismatch - Brain's Air Hunger
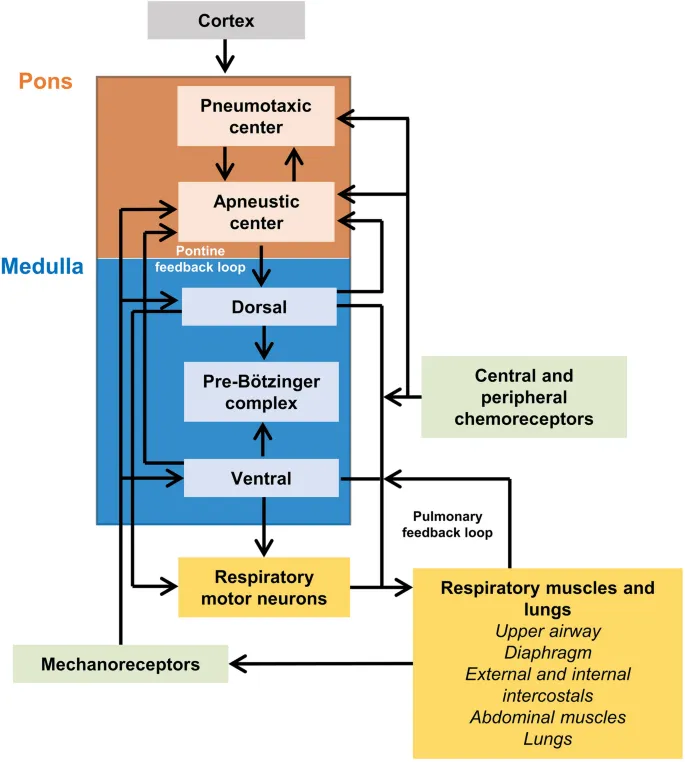
- Core principle: Dyspnea results from a discrepancy between the central respiratory motor command sent to the breathing muscles and the sensory feedback (afferent information) received from the periphery.
- Corollary Discharge: The brain sends a motor command to breathe and simultaneously sends a copy to the sensory cortex. This establishes an expectation of the work of breathing.
- Afferent Feedback: Mechanoreceptors (e.g., stretch receptors) in the lungs and chest wall report the actual movement and lung volume changes back to the brain.
- When feedback doesn't match the expectation (e.g., high effort for low tidal volume in asthma), this mismatch is interpreted as dyspnea.
⭐ The insular cortex is crucial for integrating the sensory-motor mismatch signals, contributing significantly to the unpleasant sensation of "air hunger."
Clinical Causes - Pathologic Triggers
- ↑ Work of Breathing (WOB)
- Obstructive (COPD, Asthma): ↑ Airway resistance & dynamic hyperinflation lead to respiratory muscle fatigue.
- Restrictive (Fibrosis, Kyphoscoliosis): ↓ Lung/chest wall compliance demands greater effort for tidal volume.
- Ventilation/Perfusion (V/Q) Mismatch
- Pulmonary Embolism (PE): ↑ Alveolar dead space (high V/Q) → wasted ventilation.
- Pneumonia, ARDS, Atelectasis: Creates intrapulmonary shunt (low V/Q) → hypoxemia stimulates chemoreceptors.
- Chemoreceptor Stimulation
- Heart Failure: Pulmonary congestion stimulates juxtacapillary (J) receptors. Interstitial edema also ↓ compliance.
- Metabolic Acidosis (e.g., DKA): Direct stimulation of central/peripheral chemoreceptors by $H^+$ ions.
- Neuromuscular Disease
- Myasthenia Gravis, Guillain-Barré: Inefficient respiratory muscle contraction → afferent feedback signals intense effort.
⭐ Orthopnea (dyspnea when supine) is a hallmark of decompensated heart failure. It results from fluid redistribution from the periphery to the pulmonary circulation, raising pulmonary capillary pressure.
High‑Yield Points - ⚡ Biggest Takeaways
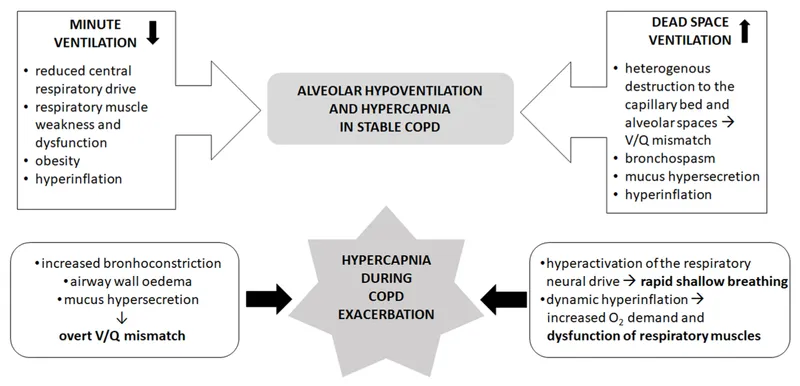
- V/Q mismatch is the most common cause, leading to hypoxemia and/or hypercapnia that stimulate chemoreceptors.
- Increased work of breathing in obstructive or restrictive disease is sensed by chest wall mechanoreceptors.
- Neuromechanical dissociation, a mismatch between central respiratory drive and mechanical response, is a key mechanism.
- Stimulation of J-receptors by interstitial fluid (e.g., pulmonary edema) causes a sensation of breathlessness.
- Vagal afferents in the airways respond to irritants and bronchoconstriction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

