Neural Control - The Brain's Breath Boss
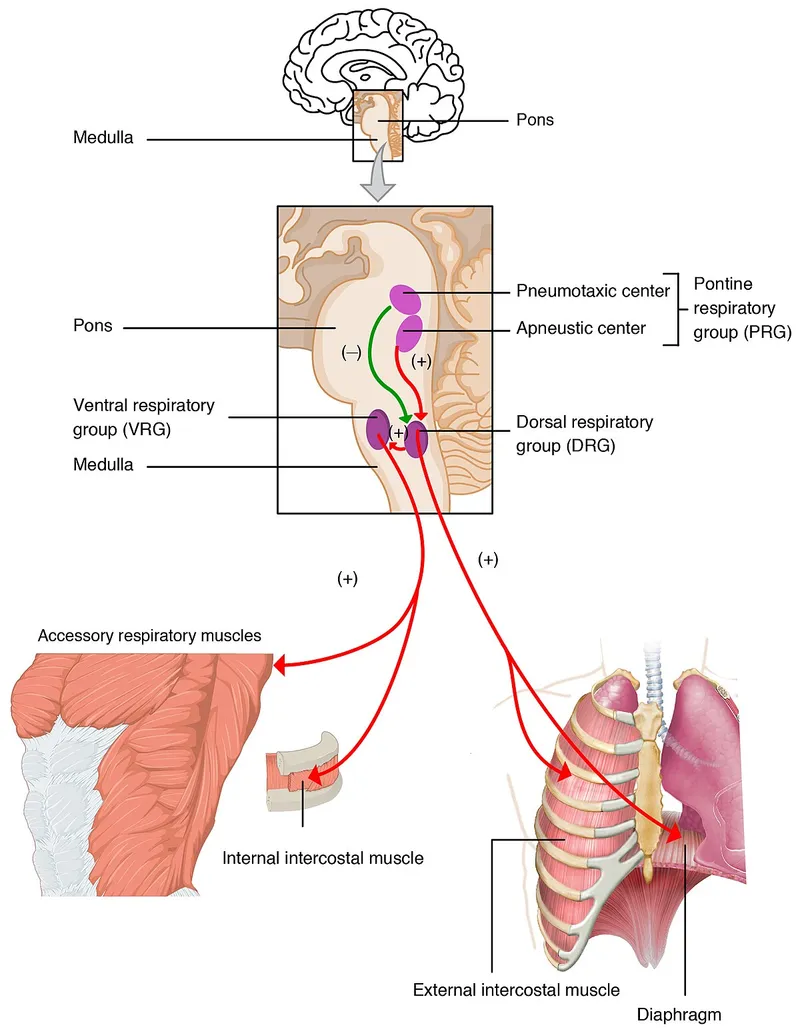
- Medulla Oblongata: The Primary Pacemaker
- Dorsal Respiratory Group (DRG): Inspiratory center. Sets the basic rhythm by stimulating the phrenic nerve.
- Ventral Respiratory Group (VRG): Handles forced breathing (active inspiration/expiration).
- Pons: The Fine-Tuner
- Pneumotaxic Center: Inhibits the DRG, helping to terminate inspiration. Controls respiratory rate and depth.
- Apneustic Center: Stimulates the DRG, prolonging inspiration. Overridden by the pneumotaxic center.
- Higher Input:
- Cortex: Voluntary control (breath-holding).
- Limbic/Hypothalamus: Emotional responses (fear, rage).
⭐ The pre-Bötzinger complex, part of the VRG, is considered the primary pacemaker generating respiratory rhythm.
Chemical Control - CO₂'s Chemical Crew
- Primary Driver: Arterial $PCO₂$ is the most potent stimulus for respiration, mediated by central and peripheral chemoreceptors.
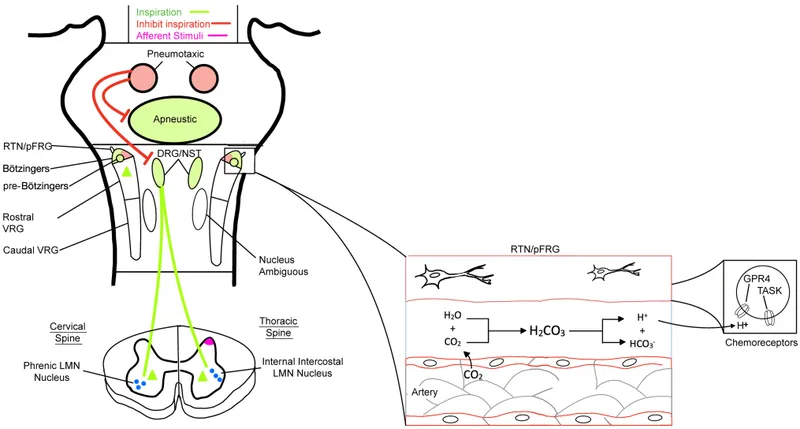
- Central Chemoreceptors (Medulla):
- Sensitive to $[H⁺]$ in cerebrospinal fluid (CSF).
- $CO₂$ freely diffuses across the blood-brain barrier, where it forms carbonic acid: $CO₂ + H₂O \leftrightarrow H₂CO₃ \leftrightarrow H⁺ + HCO₃⁻$.
- This ↑ $[H⁺]$ stimulates medullary centers to increase ventilation.
- Peripheral Chemoreceptors (Carotid & Aortic Bodies):
- Respond to ↑ $PCO₂$, ↓ $PO₂$, and ↑ $[H⁺]$.
- Hypoxic drive is only significant when $PaO₂$ drops below 60 mmHg.
⭐ In chronic hypercapnia (e.g., COPD), central chemoreceptors become less sensitive to $PCO₂$. Respiration then relies more on the hypoxic drive. Administering high-concentration O₂ can suppress this drive, leading to respiratory depression.
Other Receptors - Lung's Little Listeners
-
Pulmonary Stretch Receptors (Slow-Adapting):
- In airway smooth muscle; sense lung distension.
- Afferents via Vagus (CN X) to inhibit inspiration.
- Mediates Hering-Breuer reflex: prevents over-inflation, especially in neonates.
-
Irritant Receptors (Rapidly-Adapting):
- In airway epithelium; triggered by noxious stimuli (smoke, dust).
- Result: Cough, bronchoconstriction, mucus secretion.
-
J (Juxtacapillary) Receptors:
- In alveolar walls; stimulated by ↑ interstitial fluid (edema).
- Cause rapid, shallow breathing & dyspnea.
⭐ J-receptors are key contributors to the sensation of dyspnea (shortness of breath) in patients with pulmonary edema or heart failure.
Integrated Responses - Breath Under Pressure
-
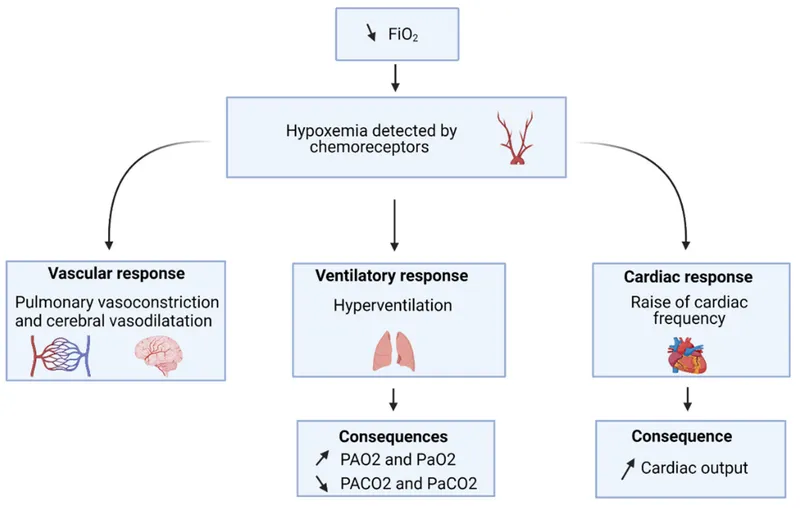
High Altitude (Hypobaric Hypoxia)
- Acute: ↓ Inspired $P_{O_2}$ → Hypoxemia → Peripheral chemoreceptors stimulate ↑ ventilation → Respiratory alkalosis.
- Acclimatization (Days-Weeks):
- Renal compensation: ↑ $HCO_3^-$ excretion to correct alkalosis.
- Hematologic: ↑ EPO → ↑ Hematocrit & Hb.
- Cellular: ↑ 2,3-BPG (right-shifts O2-Hb curve).
-
Diving (Hyperbaric Environment)
- Nitrogen Narcosis: High $P_{N_2}$ at depth causes anesthetic-like effects.
- Decompression Sickness (The Bends): Rapid ascent → dissolved $N_2$ forms bubbles in tissues/bloodstream.
⭐ At sea level, ventilation is driven by $P_{CO_2}$. At high altitude, chronic hypoxemia makes ventilation highly sensitive to and driven by $P_{O_2}$.
High‑Yield Points - ⚡ Biggest Takeaways
Error generating content for this concept group: Invalid JSON response
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

