Angiotensin II Receptors - The Two Flavors
Angiotensin II acts via two main G-protein coupled receptors (GPCRs), AT1 and AT2, with opposing effects.
- AT1 Receptors: Mediate most of the well-known effects of Angiotensin II.
- Location: Vascular smooth muscle, adrenal cortex, kidney, brain, heart.
- Action: Pro-hypertensive, pro-inflammatory, and pro-fibrotic effects.
- AT2 Receptors: Generally counterbalance AT1 receptor actions.
- Action: Vasodilation, anti-proliferative, and anti-fibrotic effects. More prominent in fetal tissues.
⭐ High-Yield: The AT1 receptor is primarily coupled to a Gq protein, activating the phospholipase C pathway, which increases intracellular calcium ($Ca^{2+}$) causing smooth muscle contraction.
AT1 Receptor Actions - The Pressure Cooker
📌 6 S's: Squeeze (vasoconstriction), Salt (aldosterone), Sip (ADH/thirst), Sympathetic, Scarring (hypertrophy), Save GFR (efferent constriction).

- Vasoconstriction: Potent vasoconstrictor (arterioles > veins) → ↑ total peripheral resistance & blood pressure.
- Hormonal Release:
- ↑ Aldosterone from adrenal cortex → ↑ Na⁺ & H₂O reabsorption.
- ↑ ADH (vasopressin) from posterior pituitary & stimulates thirst → ↑ free water retention.
- Renal Effects:
- Preferentially constricts efferent arterioles → ↑ intraglomerular pressure to maintain GFR.
- Stimulates Na⁺/H⁺ exchanger in Proximal Convoluted Tubule (PCT) → ↑ Na⁺, HCO₃⁻, and H₂O reabsorption.
- Sympathetic Facilitation: ↑ Norepinephrine release and inhibits its reuptake, amplifying sympathetic effects.
- Cellular Growth: Promotes long-term cardiac and vascular hypertrophy and remodeling.
⭐ Angiotensin II's effect on GFR is biphasic. Initially, preferential efferent constriction ↑ GFR. At very high levels, it constricts both afferent and efferent arterioles, ↓ renal blood flow and ↓ GFR.
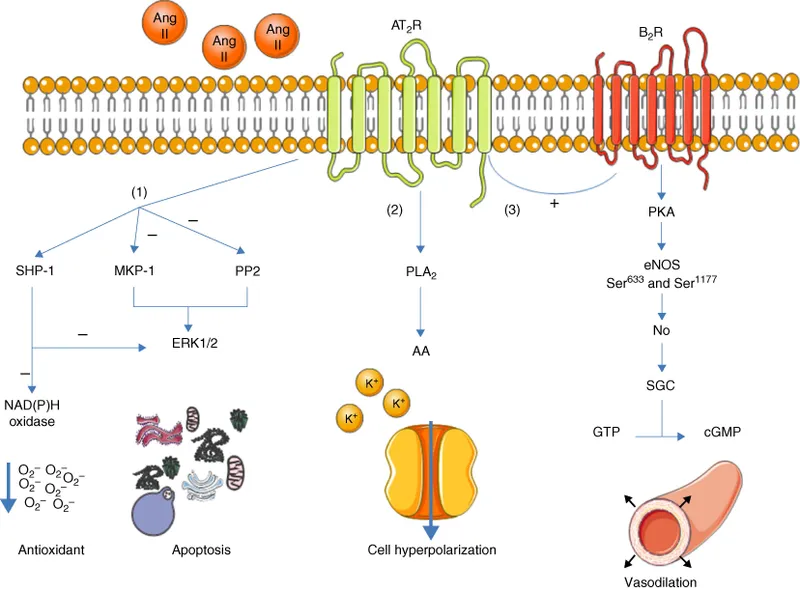
AT2 Receptor Actions - The Counter-Punch
- Provides a counter-regulatory balance to AT1 receptor actions.
- Primary effects are opposite to AT1 stimulation:
- Vasodilation: Mediated by ↑ Nitric Oxide (NO) and bradykinin.
- Anti-proliferative: Inhibits cell growth and promotes tissue repair.
- Apoptosis: Induces programmed cell death, contrasting AT1's growth signals.
⭐ AT2 receptors are abundant in fetal tissues, crucial for development. In adults, their expression is low but can be upregulated in pathological states like tissue injury or inflammation.
Clinical Pharmacology - Taming the Beast
- Angiotensin Receptor Blockers (ARBs): Competitively block Angiotensin II Type 1 (AT1) receptors.
- Drugs: -sartan family (e.g., Losartan, Valsartan).
- Action: Blocks vasoconstriction and aldosterone release → ↓ blood pressure.
- Uses: Hypertension, heart failure, diabetic nephropathy (proteinuria).
- Key Advantage over ACE Inhibitors: ARBs do not inhibit bradykinin breakdown.
- Result: No dry cough.
- ⚠️ Angioedema is still a potential, albeit rare, side effect.
⭐ Exam Favorite: A patient develops a persistent, dry cough on an ACE inhibitor (e.g., Lisinopril). The most appropriate switch is to an ARB (e.g., Valsartan) to resolve the cough while maintaining RAAS inhibition.
High‑Yield Points - ⚡ Biggest Takeaways
- Angiotensin II acts on AT1 receptors (Gq-coupled) for most of its pressor effects.
- It's a potent vasoconstrictor, especially of the efferent arteriole, initially preserving GFR.
- Stimulates aldosterone release from the adrenal cortex, leading to Na+ and water retention.
- Directly increases Na+ reabsorption in the proximal tubule via the Na+/H+ exchanger.
- Promotes ADH release from the posterior pituitary and stimulates thirst.
- Contributes to long-term cardiac hypertrophy and fibrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

