Intestinal Barrier - The Gut's Gatekeepers
-
Function: Regulates passage of luminal contents (nutrients, microbes) into circulation. A selective, semi-permeable barrier.
-
Components & Layers of Defense:
- Physical Barrier: Epithelial cells linked by tight junctions (TJs).
- TJ Proteins: Claudins, Occludins, & Zonulin-1 (ZO-1) form the seal. 📌 Mnemonic: Come On, Zip-it!
- Mucus Layer: Produced by goblet cells; traps debris & bacteria.
- Chemical Barrier: Secretions that neutralize threats.
- Antimicrobial Peptides (AMPs): Defensins & lysozyme from Paneth cells.
- Secretory IgA (sIgA): Binds and neutralizes luminal antigens and pathogens.
- Immunological Barrier: Gut-Associated Lymphoid Tissue (GALT).
- Peyer's patches, intraepithelial lymphocytes (IELs).
- Physical Barrier: Epithelial cells linked by tight junctions (TJs).
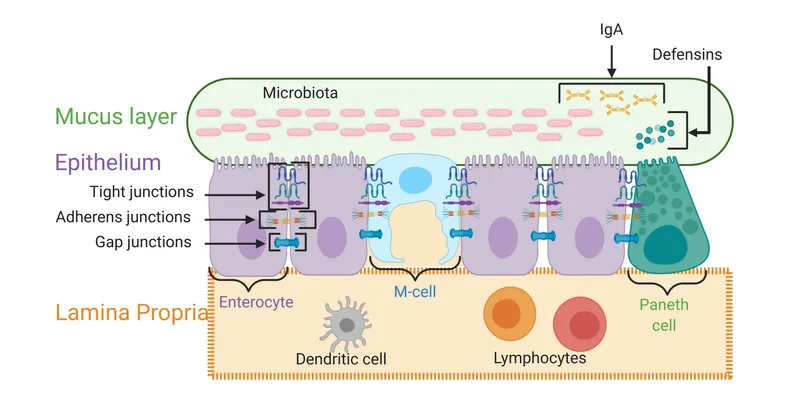
⭐ Exam Favorite: Increased intestinal permeability ("leaky gut") is linked to elevated levels of zonulin, a protein that reversibly opens tight junctions. This is implicated in autoimmune and inflammatory disorders like Celiac disease and IBD.
Barrier Regulation - Opening the Floodgates
- Zonulin: The primary physiological modulator of intestinal permeability, acting as a gatekeeper for tight junctions (TJs).
- Triggers for release include gliadin (from gluten) and bacterial dysbiosis.
- Mechanism of Increased Permeability:
- Inflammatory signals (e.g., TNF-α, IFN-γ) or zonulin upregulate Myosin Light Chain Kinase (MLCK).
- MLCK activation phosphorylates myosin, causing contraction of the perijunctional actin ring.
- This contraction pulls TJ proteins (claudins, occludin) apart, opening the paracellular pathway.
⭐ Elevated zonulin levels are strongly associated with celiac disease and other autoimmune disorders, serving as a biomarker for compromised barrier function ("leaky gut").
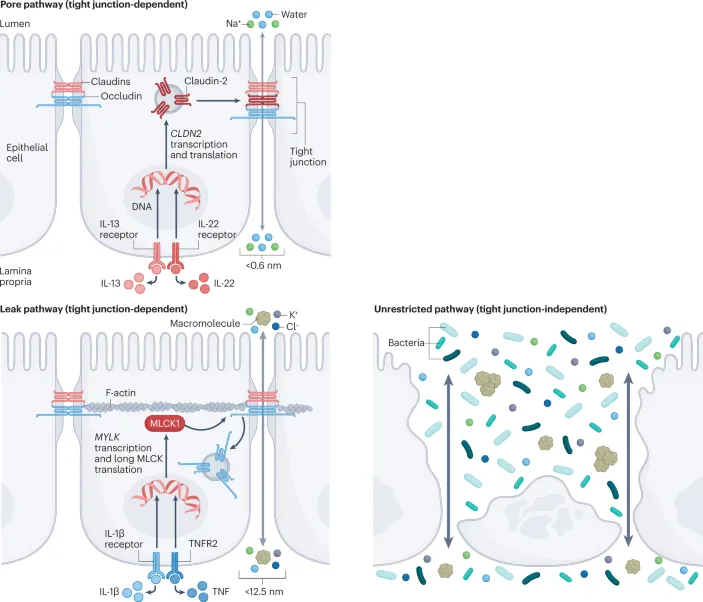
Barrier Dysfunction - When the Walls Fall
- Pathogenesis: Compromise of tight junctions (zonula occludens) & epithelial integrity, leading to ↑ intestinal permeability ("leaky gut").
- Triggers:
- Infections: Viral (Norovirus), bacterial (Salmonella, C. difficile).
- Inflammation: IBD (Crohn's, UC), celiac disease.
- Ischemia: Shock, sepsis, major trauma/burns.
- Toxins/Drugs: Alcohol, NSAIDs.
- Consequences:
- Translocation of luminal antigens (e.g., LPS) into circulation.
- Triggers systemic inflammatory response (↑ TNF-α, IL-1, IL-6).
- Can precipitate Systemic Inflammatory Response Syndrome (SIRS) & Multi-Organ Dysfunction Syndrome (MODS).
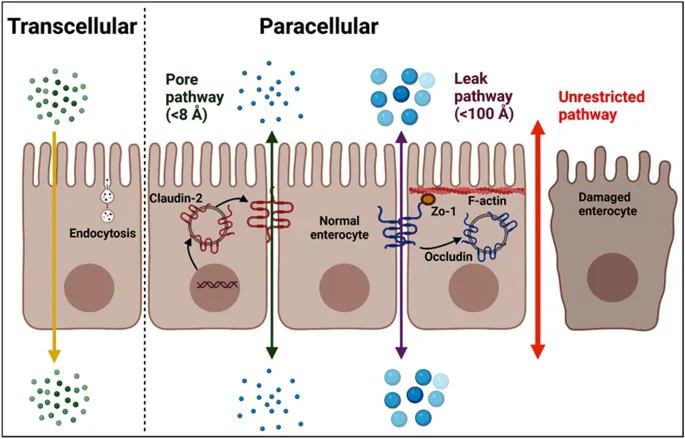
⭐ Zonulin, a protein that modulates tight junction permeability, is a key regulator. Its upregulation, triggered by gliadin and bacteria, is implicated in celiac disease and other autoimmune disorders.
High‑Yield Points - ⚡ Biggest Takeaways
- The intestinal barrier relies on tight junctions (claudins, occludins), a mucus layer, and secretory IgA (sIgA).
- Barrier dysfunction, or "leaky gut," is a key factor in celiac disease and inflammatory bowel disease (IBD).
- Zonulin is a key physiological modulator of intestinal permeability, often upregulated in autoimmune conditions.
- Paneth cells provide innate immunity by secreting antimicrobial peptides (e.g., defensins).
- Goblet cells produce mucus, forming a protective physical and chemical shield.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

