Hypoxemia Basics - The A-a Gradient
-
A-a gradient: The difference between alveolar ($PAO_2$) and arterial ($PaO_2$) oxygen tension, which helps differentiate causes of hypoxemia.
-
Calculation: $A-a \text{ gradient} = PAO_2 - PaO_2$.
-
A normal gradient is ~5-15 mmHg; it increases with age. Expected A-a gradient = $(Age/4) + 4$.
-
Normal A-a Gradient Causes:
- ↓ Inspired O₂ (e.g., high altitude)
- Hypoventilation (e.g., opioid overdose)
-
Elevated A-a Gradient Causes:
- V/Q Mismatch
- Shunt
- Diffusion Limitation
⭐ A normal A-a gradient in a hypoxemic patient points towards either hypoventilation or a low inspired oxygen level, as the lung parenchyma itself is functioning correctly.
Core Mechanisms - V/Q Mismatch vs. Shunt
| Feature | V/Q Mismatch | Shunt (Extreme V/Q Mismatch) |
|---|---|---|
| Definition | Areas with low ventilation relative to perfusion (V/Q < 1) | Blood bypasses ventilated alveoli; V/Q approaches 0 |
| Pathophysiology | Imbalance between alveolar ventilation and capillary blood flow | Deoxygenated blood mixes with arterial blood (venous admixture) |
| Response to 100% O₂ | Corrects hypoxemia (PaO₂ > 500 mmHg) | Does NOT correct hypoxemia |
| $A-a \text{ gradient}$ | ↑ Increased | ↑ Increased |
| Examples | Pneumonia, PE, COPD, Asthma | ARDS, Pulmonary edema, Intracardiac shunt, Atelectasis |
Other Causes - The Other Oxygen Thieves
-
Cyanide Poisoning:
- Inhibits cytochrome c oxidase → blocks aerobic respiration.
- Cells can't utilize O₂ → ↑ SvO₂ (venous oxygen saturation).
- Presents with almond breath, headache, and confusion.
-
Carbon Monoxide (CO) Poisoning:
- Binds Hb with >200x affinity than O₂ → ↓ O₂-carrying capacity.
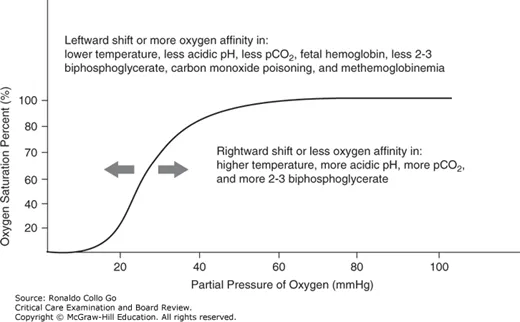
- Causes left-shift of O₂-dissociation curve → ↓ O₂ unloading to tissues.
- Classic sign: cherry-red skin (usually a postmortem finding).
-
Methemoglobinemia:
- Heme iron is oxidized (Fe²⁺ → Fe³⁺); MetHb cannot bind O₂.
- Causes functional anemia & left-shift of O₂-dissociation curve.
- 📌 Causes: Nitrates, dapsone, local anesthetics (e.g., benzocaine).
- Classic sign: chocolate-colored blood.
⭐ In CO poisoning and methemoglobinemia, the measured PaO₂ (dissolved O₂) is normal, but SaO₂ (O₂ saturation) is decreased, creating a saturation gap.
High‑Yield Points - ⚡ Biggest Takeaways
- The A-a gradient is the crucial first step: it's normal in hypoventilation and low PiO2, but elevated in others.
- V/Q mismatch, the most common cause, corrects with supplemental O2.
- A shunt is the only cause that does not correct with 100% O2.
- Hypoventilation is uniquely defined by a concurrent elevated PaCO2 (hypercapnia).
- Diffusion limitation (e.g., fibrosis) characteristically worsens with exercise.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

