Pathophysiology - The Base Buildup
- Definition: A primary ↑ in serum $HCO_3^−$, leading to ↑ pH.
- Mechanism: Involves two distinct phases:
- Generation: The initial insult causing acid loss or base gain (e.g., vomiting, alkali ingestion).
- Maintenance: The kidney's failure to excrete the excess $HCO_3^−$. This is the key step and is primarily driven by:
- Volume depletion (Euvolemia or hypovolemia)
- Chloride depletion
- Hypokalemia
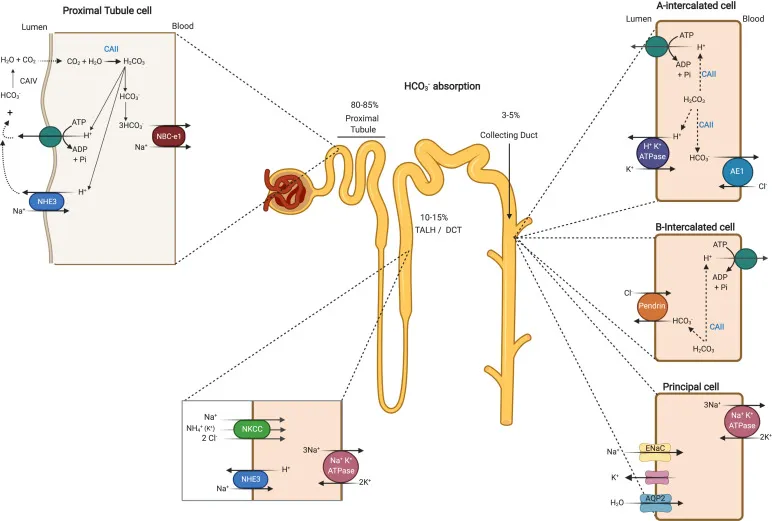
⭐ Contraction Alkalosis: Volume depletion → ↑ Angiotensin II → ↑ Proximal tubule $Na^+-H^+$ exchange → ↑ $HCO_3^−$ reabsorption, thus maintaining the alkalosis.
Etiologies - Acid Out, Bicarb In
- H⁺ Loss (Acid Out):
- GI: Vomiting, nasogastric (NG) suction.
- Renal: Diuretics (loop/thiazide), hyperaldosteronism.
- HCO₃⁻ Gain (Bicarb In):
- Exogenous: Citrate from blood transfusions, acetate in TPN, antacid abuse.
| Category | Urine Chloride ($U_{Cl^−}$) | Key Causes |
|---|---|---|
| Saline-Responsive | < 20 mEq/L | - Vomiting / NG suction - Prior diuretic use |
| Saline-Resistant | > 20 mEq/L | - Hyperaldosteronism (Conn's) - Bartter & Gitelman syndromes |
📌 Mnemonic: 'VOMIT' (Vomiting, Oversecretion of aldosterone, Mineralocorticoid excess, Iatrogenic, Total parenteral nutrition).
Compensation - The Body's Balancing Act
-
Respiratory Compensation: The lungs hypoventilate to retain acidic $CO_2$ and lower pH.
- Formula: Expected PaCO₂ = 0.7 * [HCO₃⁻] + 20 (± 5)
-
Renal Compensation: Kidneys try to excrete excess $HCO_3^−$. This is often impaired by volume depletion or hypokalemia, which maintains the alkalosis.
-
Paradoxical Aciduria: Despite systemic alkalosis, urine becomes acidic. This occurs in volume-depleted states (e.g., vomiting).
⭐ A low urine chloride (< 20 mEq/L) strongly suggests a saline-responsive metabolic alkalosis, where correcting the volume deficit is the primary treatment.
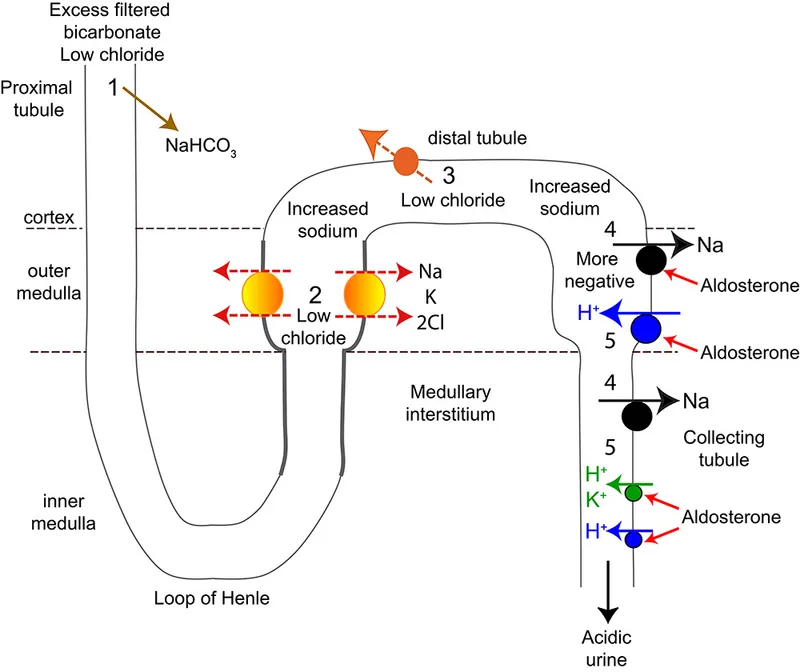
- Metabolic alkalosis is driven by a primary ↑ in serum HCO₃⁻.
- Differentiated by urine chloride (UCl⁻) and response to saline.
- Saline-responsive (UCl⁻ < 20 mEq/L) is caused by volume & Cl⁻ depletion (e.g., vomiting, diuretics) and corrects with IV saline.
- Saline-resistant (UCl⁻ > 20 mEq/L) is due to mineralocorticoid excess (e.g., Conn's, Cushing's).
- Respiratory compensation involves hypoventilation, leading to a predictable ↑ in PaCO₂.
- Often associated with hypokalemia due to intracellular K⁺ shifting.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

